Translate this page into:
Autism spectrum disorder and compliance with a removable orthodontic functional appliance: A case report

*Corresponding author: Nik Mukhriz Nik Mustapha, Centre for Paediatric Dentistry and Orthodontic Studies, Faculty of Dentistry, Universiti Teknologi MARA, Jalan Hospital, Selangor, Malaysia. nikmukhriz@uitm.edu.my
-
Received: ,
Accepted: ,
How to cite this article: Md Lepi J, Nik Mustapha N. Autism spectrum disorder and compliance with a removable orthodontic functional appliance: A case report. APOS Trends Orthod. doi: 10.25259/APOS_12_2024
Abstract
Autism Spectrum Disorder (ASD) is a multifaceted developmental disability that originates from a neurological disorder, leading to difficulties in the development of social interaction and communication skills. Consequently, this poses a challenge in the provision of oral health care. We report a case of a 13-year-old male with ASD who was concerned about “sticking out upper front teeth.” The patient presented with a Class II Division 1 incisor relationship on a Class 2 skeletal base with retrognathic mandible. The malocclusion was complicated by spacing in the upper and lower arches, proclined upper labial segment, increased overjet 12mm, overbite 90% complete to teeth, and incompetent lip with lower lip trap. The canine relationship was Class II ½ unit bilaterally, and the molar relationship was Class II ½ unit on the right and Class II ¾ unit on the left. The IOTN score was 5a for dental health and 9 for aesthetics. Growth modification to encourage mandibular growth, using a removable Twin Block appliance. The patient displayed excellent compliance with the appliance and effectively addressed his concerns while boosting his self-esteem. By understanding and addressing the unique needs of patients with ASD in orthodontic treatment, patient’s comfort and overall experience can be enhanced along with the likelihood of a successful treatment outcome. Customized treatment plans that respect sensory sensitivities and communication preferences pave the way for a more positive orthodontic journey for individuals with ASD, ultimately leading to enhanced dental well-being and bolstered self-assurance in one’s smile.
Keywords
Autism spectrum disorder
Growth modification treatment
Orthodontics
INTRODUCTION
The initial documentation of autism disorder (AD) can be attributed to Kanner, an American child psychologist, in 1943.[1] The Autism Society of America, through diagnostic and statistical manual of mental disorders (DSM)-4, published in 1994, has defined AD as a complex developmental disability that typically appears during the first 3 years of life and is the result of a neurological disorder that affects the normal functioning of the brain, impacting development in the areas of social interaction and communication skills. The condition is distinguished by atypical emotional, social, and language acquisition.[2] The terminology has evolved, and the diagnostic criteria for autism have been redefined in the DSM-5, published in 2013.[3] The DSM-5 diagnostic criteria for autism spectrum disorder (ASD) encompass two fundamental areas: They exhibit challenges in interpersonal relationships and interaction as well as exhibit limited abilities and repetitive behaviors. These symptoms can significantly impede an individual’s ability to effectively engage in various domains of life, including educational, occupational, and personal spheres.[3] The prevalence rate of ASD has been observed to exhibit an upward trend over recent years. Initial estimates of the prevalence of ASD show considerable variation, spanning from 0.7 cases/10,000 individuals to 72.6 cases/10,000 individuals. The median estimate, however, stands at 13 cases/10,000 children.[4] Children with autism who presented with Class II Division 1 malocclusion may experience significant esthetic concerns as they grow.[5,6] They may face challenges related to self-esteem and self-image due to an increased overjet, which can result in teasing or bullying by their peers,[7,8] exacerbating their existing social and emotional difficulties. A prominent overjet also increases the risk of dental trauma.[9-11] In instances of accidents or falls, the upper anterior teeth are subject to increased exposure and susceptibility to injury, such as chipping or fracturing. Some autistic individuals display habits such as thumb sucking, lip biting, or tongue thrusting, which may worsen the overjet, rendering orthodontic treatment more complex.[12] An increased overjet can lead to functional difficulties, such as difficulty biting into certain foods or maintaining proper lip closure at rest.
Individuals with ASD may face considerable struggle in receiving a removable functional appliance. Various factors can contribute to the intricacy of this process. Among the challenges are sensory sensitivities that can make wearing removable functional appliances uncomfortable.[13,14] The feeling of the appliance in the mouth, the texture of the material, and the pressure on the teeth and jaws can be overwhelming for some individuals, leading to resistance and discomfort. Patients may experience challenges comprehending instructions, articulating their discomfort, or adhering to the orthodontist’s recommendations regarding using orthodontic appliances.[15,16] This can impede the progress of orthodontic treatment. Next, fitting, inserting, and adjusting the appliance can trigger anxiety and resistance.[17] This can lead to delays in treatment and non-compliance. Repetitive behaviors, which include removing or manipulating the appliance, can interfere with the effectiveness of the treatment and may require additional monitoring and support.[15] In addition, orthodontic clinics and dental offices can be overwhelming due to bright lights, unfamiliar sounds, and the presence of other patients.[18] Locating orthodontists or dental professionals with expertise in treating individuals with ASD can be an onerous journey.[18] The limited availability of specialized providers can lead to extended waiting periods and failure to access orthodontic services.
It is essential to recognize that each autistic individual is unique, and the effects of an increased overjet can vary significantly. Orthodontic treatment may be undertaken to correct the overjet, but the approach should be tailored to the specific needs and sensitivities of the patient. Communication strategies and sensory accommodations may also be necessary to facilitate successful orthodontic treatment in this population.
This case report provides an account of the orthodontic treatment delivered to a growing child diagnosed with ASD, presenting with significant overjet and Class II Division 1 malocclusion.
CASE REPORT
Summary
MM, a 13-year-old boy, was referred to the Postgraduate Orthodontic Clinic, Faculty of Dentistry Universiti Teknologi MARA. The patient attended with his mother, and the mother was concerned about the “sticking out upper front teeth.” The patient presented with a Class II Division 1 incisor relationship on a Class II skeletal base with reduced vertical proportion. The malocclusion is complicated by spacing in the upper and lower arches, proclined upper labial segment, increased overjet 12 mm, overbite 90% complete to teeth, and incompetent lip with lip trap on upper incisors. The canine relationship was Class II ½ unit bilaterally, and the molar relationship was Class II ½ unit on the right and Class II ¾ unit on the left. The index of orthodontic treatment need score was 5a for the dental health component and 9 for the esthetic component.
Medical history
MM was diagnosed with mild ASD at the age of 6 years old and not under any medications.
Family history
According to the parents, there were no known cases of ASD among their close or distant relatives.
On the first visit, only a clinical examination was performed. The patient was familiarized with the clinic and allowed to touch the instruments for desensitization. Orthodontic records were taken on the following visit, including study models, extraoral and intraoral photographs, and panoramic and lateral cephalometric radiographs.
Extraoral examination
The patient had a convex profile, Class II skeletal base with retrognathic mandible, reduced Frankfort Mandibular Plane Angle (FMPA), and pleasant facial asymmetry. On soft-tissue assessment, acute nasolabial and labiodental fold angles with protrusive upper and lower lips concerning Ricket’s E-line were observed. Furthermore, the patient presented with incompetent lips and lower lip traps. Smile analysis revealed a consonant smile, a moderate buccal corridor visible, and an upper dental centerline coincident with the facial midline [Figure 1].
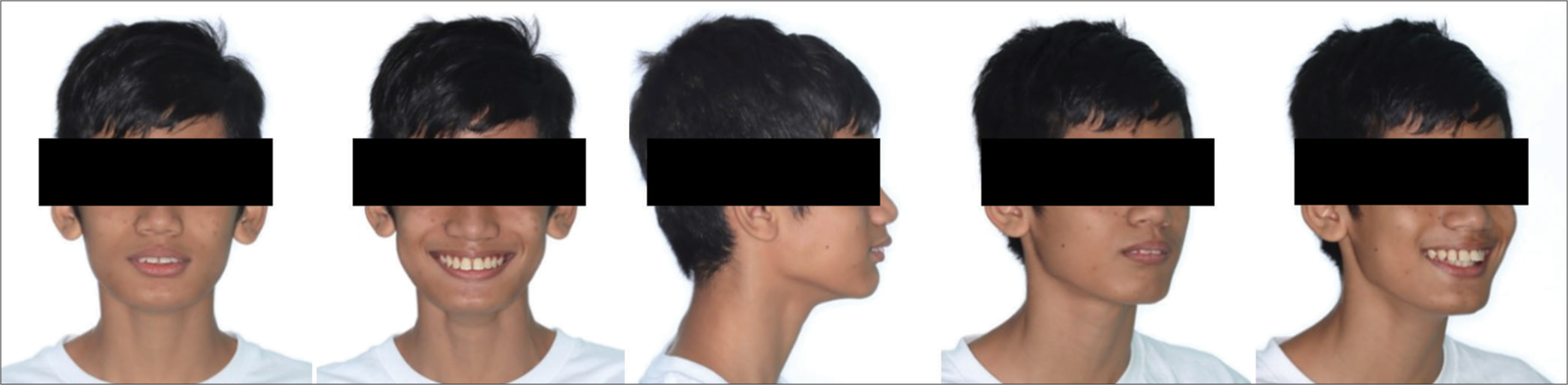
- Pre-treatment extraoral photographs.
Intraoral examination
On conducting an intraoral analysis, it was observed that the patient exhibited adequate oral hygiene practices with good gingival health. Intraoral clinical examination indicated that the patient had good oral hygiene, all permanent teeth were clinically present excluding second and third molars in all quadrants, mild irregularities in the lower labial segment, Class II Division 1 incisor relationship, increased overjet of 12 mm, increased overbite 90% complete to palate with coincident upper lower dental centreline. All canines were upright in angulation. The canine relationship was Class II ½ unit bilaterally, and the molar relationship was Class II ½ unit on the right and Class II ¾ unit on the left [Figure 2].
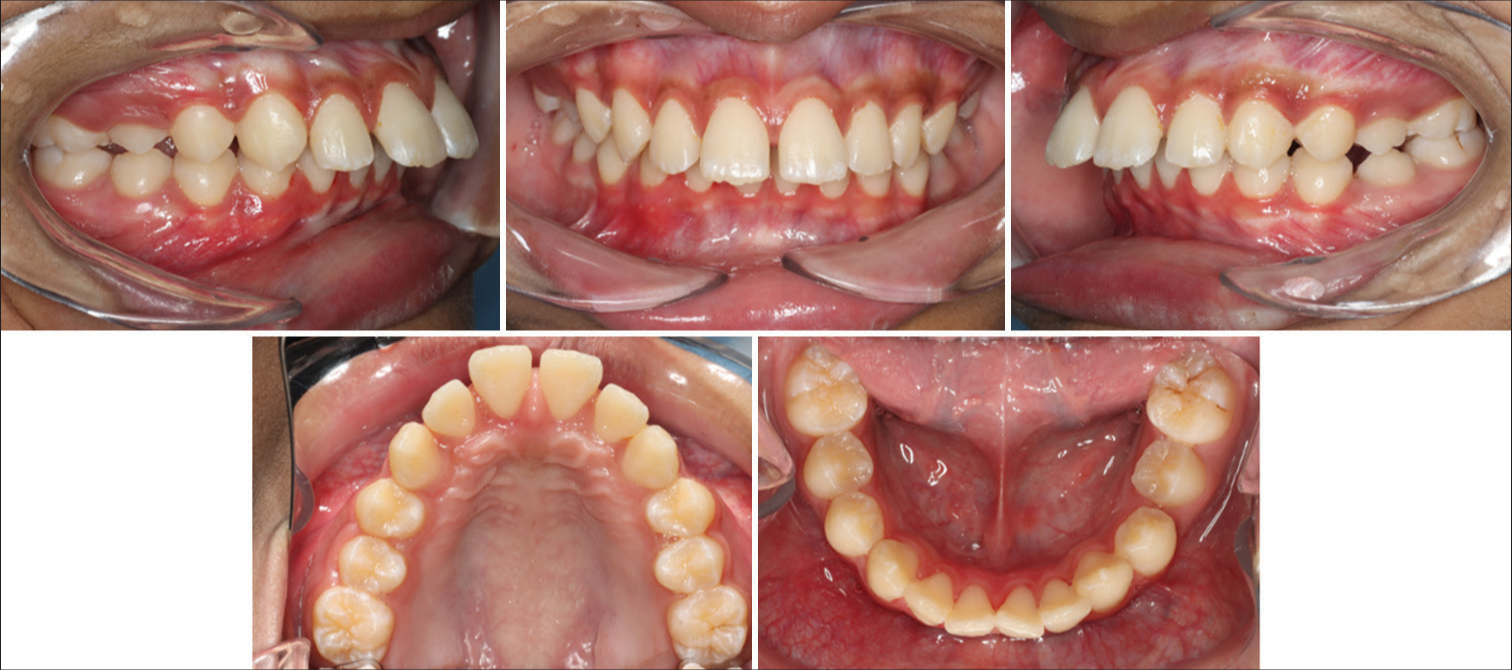
- Pre-treatment intraoral photographs.
Radiographic analysis
The pre-treatment dental panoramic radiograph showed permanent teeth, including all developing permanent second and third molars. The third molar crypt of the upper left quadrant was absent. No obvious dental pathology was observed [Figure 3].
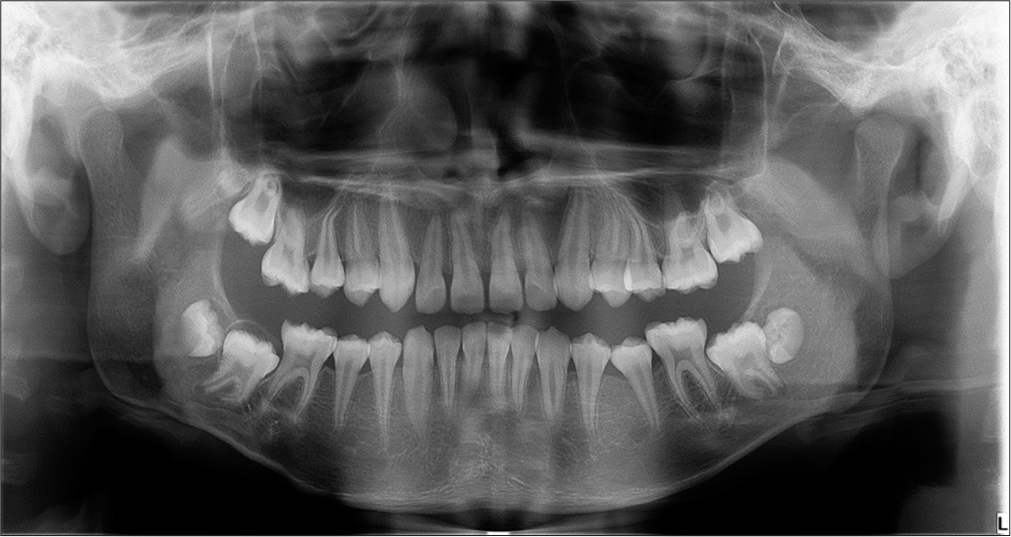
- Pre-treatment dental panoramic tomograph.
The cephalometric analysis showed that the patient presented with a Class II skeletal base due to a retrognathic mandible supported by Witts’s appraisal analysis. A hypodivergent facial pattern was confirmed from the FMPA value and Jarabak ratio. Upper incisors were proclined, lower incisors were retroclined, and there were reduced inter-incisal angles. In addition, nasolabial angles were acute, and there were procumbent upper and lower lip in relation to the Ricketts E-line [Figure 4]. Cephalometric measurements are shown in [Table 1].
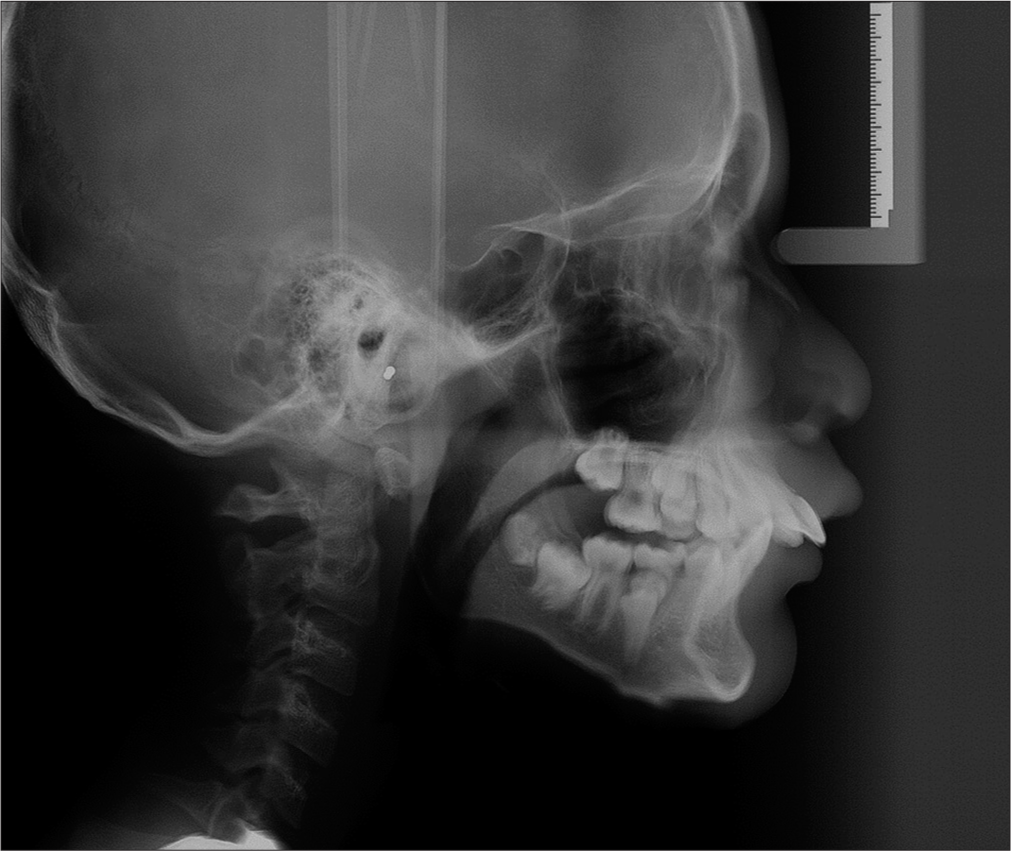
- Pre-treatment lateral cephalogram.
| Value | Patient | Norms |
|---|---|---|
| SNA | 84.90° | 84.5°±4 |
| SNB | 79.39° | 81.2°±4.1 |
| ANB | *5.51° | 3.2°±1.2 |
| SNtoMXPl | 5.18° | 8°±3 |
| MMPA | 21.31° | 24.8°±6.7 |
| %LAFH | 56.98% | 55.7%±2.3 |
| UIA | *129.46° | 117.3°±6.5 |
| LIA | 96.70° (Tweed’s ideal: 98.69°) |
96°±7.1 |
| IIA | 112.53° | 121.8°±8.8 |
| NLA | *67.59° | 100°±10 |
| Analysis | Patient | Normal value |
| Witts Analysis | +7.26 | 0mm |
| Upper lip to E-line | *+3.41mm | -4mm±2 |
| Lower lip to E-line | *+0.23mm | -2mm±2 |
| Jarabak’s ratio | 71.09% | 58-63% |
Sources of normal values
Jacobson A. The “Wits” appraisal of jaw disharmony. Am J Orthod 1975;67(2):125-133.
Houston WJB, Stephens CD & Tulley WJ (1992). A textbook of orthodontics. Wright, Oxford
Norman, N. H., Azmi, N. A. M. K., Amar, S. N. T., & Ghani, S. H. A. (2020). Cephalometric Norms of the Malay Population. International Medical Journal, 27(2).
Diagnosis
Based on clinical presentation and investigations elicited, several problem lists are listed, along with treatment aims, as shown in [Table 2].
| Problem list | Treatment aims |
|---|---|
| 1. Moderate Class 2 skeletal pattern with reduced vertical proportion | 1. To maintain good OH |
| 2. Mild irregularities on LLS | 2. To correct AP skeletal discrepancy by growth modification |
| 3. Spacing 1mm distal to LL4 | 3. To relief crowding on lower arch |
| 4. Spacing and procline upper labial segment | 4. To level and align |
| 5. Class II Division 1 incisor relationship | 5. To improve overbite |
| 6. Increased overjet of 12mm | 6. To correct overjet |
| 7. Increased overbite of 90% complete to palate | 7. To achieve Class I incisor, canine and molar relationship |
| 8. Canine relationship is Class II ½ unit bilaterally | 8. To retain corrected occlusion |
| 9. Molar relationship Class II ½ unit on the right, Class II ¾ unit on the left | 9. To monitor 7 and 8 eruption |
| 10. Incompetent lips | |
| 11. Liptrap on upper incisors |
LLS: Lower labial segment, LL4: Lower left 4, OH: Oral hygiene, AP: Antero-posterior
Treatment objective
The orthodontic treatment aimed to attempt growth modification to improve the anteroposterior skeletal discrepancy.
Treatment plan
Treatment started with oral hygiene instructions and diet advice, maintaining regular visits to the pediatric dentistry clinic. A modified Clark Twin Block functional appliance was prescribed to attempt growth modification and subsequently correct the patient’s skeletal discrepancy.
Design of appliance
The design of the appliance is illustrated in [Figure 5].
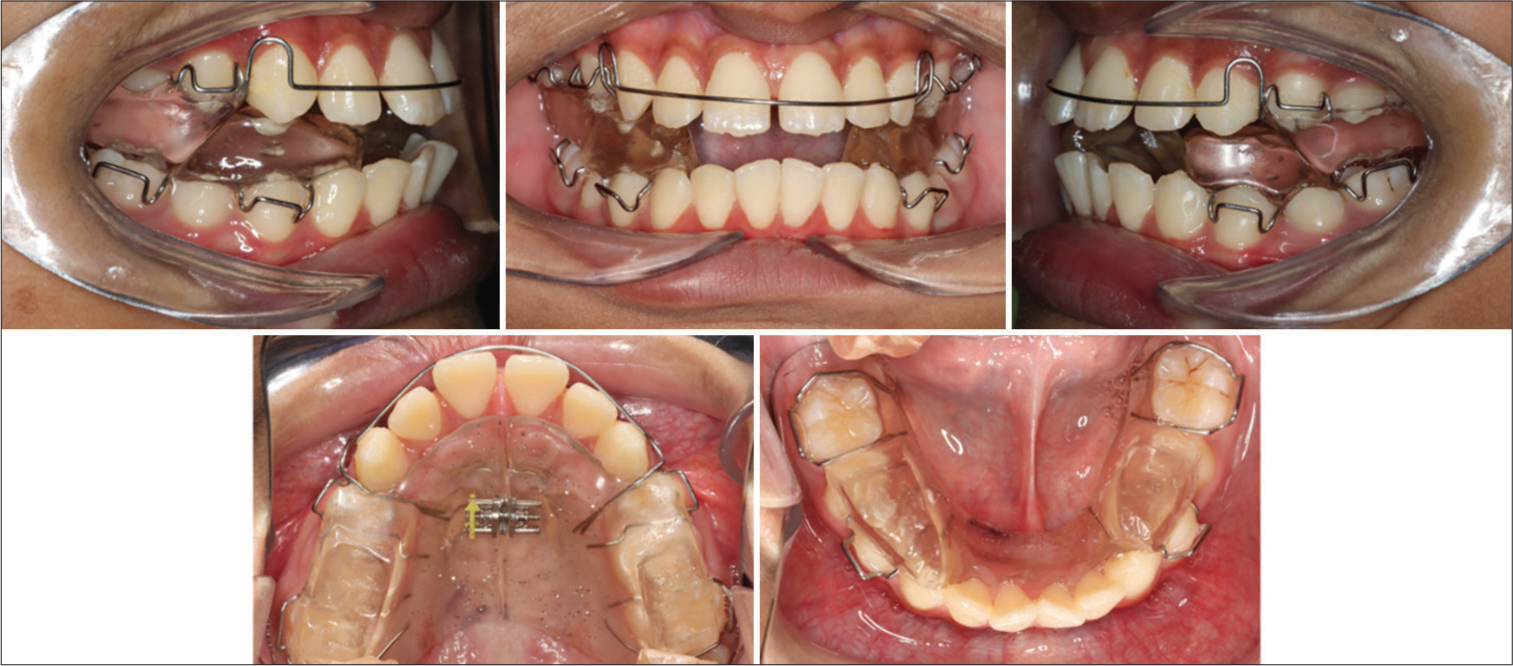
- Modified Clark Twin Block appliance photographs.
Upper appliance
Labial bow from upper canine to canine (0.7 mm SS wire)
70° inclined acrylic block bite planes
Midline expansion screw
Adams clasps on first premolars and first permanent molars (0.7 mm SS wire).
Lower appliance
70° inclined acrylic block bite planes
Adams clasps on first premolars and first permanent molars (0.7 mm SS wire).
Treatment alternatives
Fixed functional appliances
Fixed functional appliances such as Herbst appliance, Forsus, and mandibular anterior repositioning appliance offer several advantages in orthodontic treatment. Being a fixed appliance, it eliminates concerns related to patient compliance, ensuring consistent wear and effectiveness. Its primary function is to promote mandibular advancement, leading to efficient correction of Class II malocclusions. However, the fixed nature of the appliance can pose challenges for oral hygiene maintenance, potentially causing difficulties in cleaning. Patients may also experience initial discomfort and speech difficulties. Regular professional adjustments are necessary to optimize the appliance’s performance, making periodic dental visits a requirement for those undergoing Herbst Appliance treatment.
Comprehensive orthodontic treatment with pre-adjusted edgewise fixed appliance
Comprehensive orthodontic treatment is a valuable approach to rectifying Class II malocclusion with an increased overjet, offering numerous benefits. This method not only corrects malocclusion but also enhances the overall esthetics of the smile, fostering confidence and facial harmony. Beyond cosmetic improvements, comprehensive orthodontics contributes to functional enhancements by ensuring a more effective interdigitation and reducing the risk of trauma. In addition, the treatment aids in preventing potential dental problems associated with malocclusion. However, it comes with certain drawbacks, such as the need for extraction, the time commitment required for treatment, potential esthetic concerns during the process, and challenges in maintaining optimal oral hygiene with orthodontic appliances, which will be the main challenge with autistic patients. Discomfort and periodic adjustments are also considerations, and the financial investment can be significant. Despite these considerations, the stable and long-term results achieved through comprehensive orthodontic treatment underscore its effectiveness in addressing Class II malocclusion with an increased overjet. Deciding on this treatment option should involve carefully considering individual preferences, medical status, and treatment goals.
Orthognathic surgery
It is a comprehensive solution for addressing severe Class II malocclusions when the growth has ceased. Offering a permanent correction, it effectively tackles skeletal discrepancies and can bring about significant esthetic improvements. Despite these advantages, the procedure comes with inherent drawbacks. It is an invasive process involving associated risks, necessitating careful consideration of potential complications. The recovery period is typically prolonged, requiring patience and commitment from the patient. Before undergoing orthognathic surgery, a thorough assessment by an oral and maxillofacial surgeon is imperative to ensure suitability and achieve optimal outcomes. The decision to pursue this treatment option should involve a detailed discussion between the patient and the surgical team, weighing the benefits against the associated challenges.
Treatment progress and result
The modified Clark Twin Block appliance was issued in May 2022. The patient was reviewed 2 weeks after the appliance was issued to assess compliance. Then, he was called regularly every 8 weeks for review. Overjet, overbite, canine, and molar relationships were recorded on every visit. After 6 months of full-time appliance wear, significant improvement was noted in profile and lip competency [Figure 6]. Unfortunately, the patient came with a fractured appliance. A steep and deep appliance was then issued to maintain correction and assess the correction’s stability [Figure 7]. A significant correction in molar and canine relation was obtained, along with a substantial reduction in overjet and overbite [Figure 8].
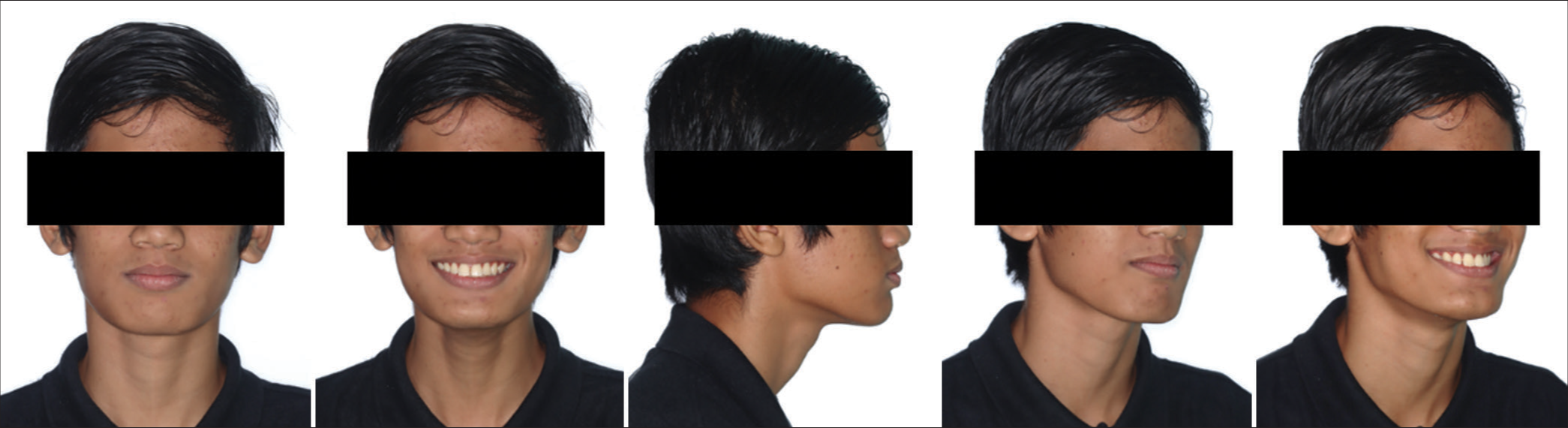
- Post-functional appliances treatment extraoral photographs.
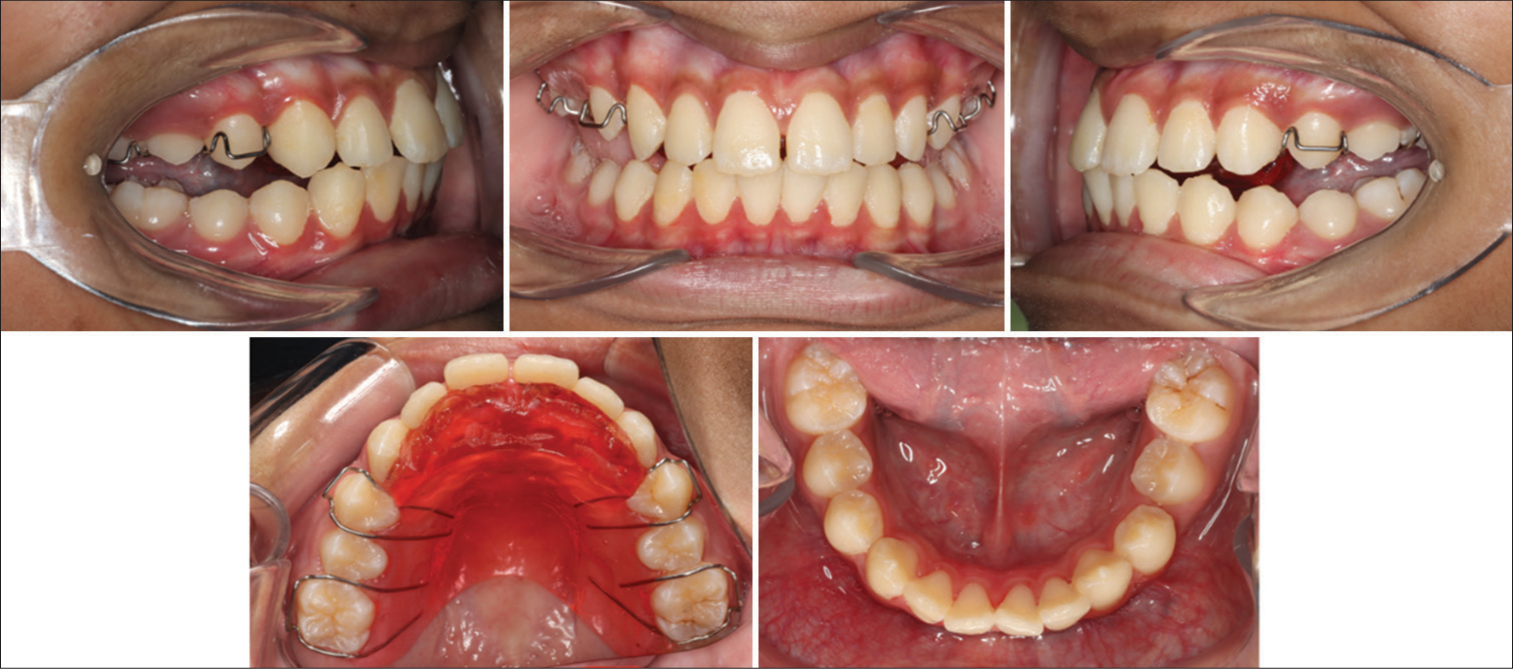
- Steep and deep appliance photographs.
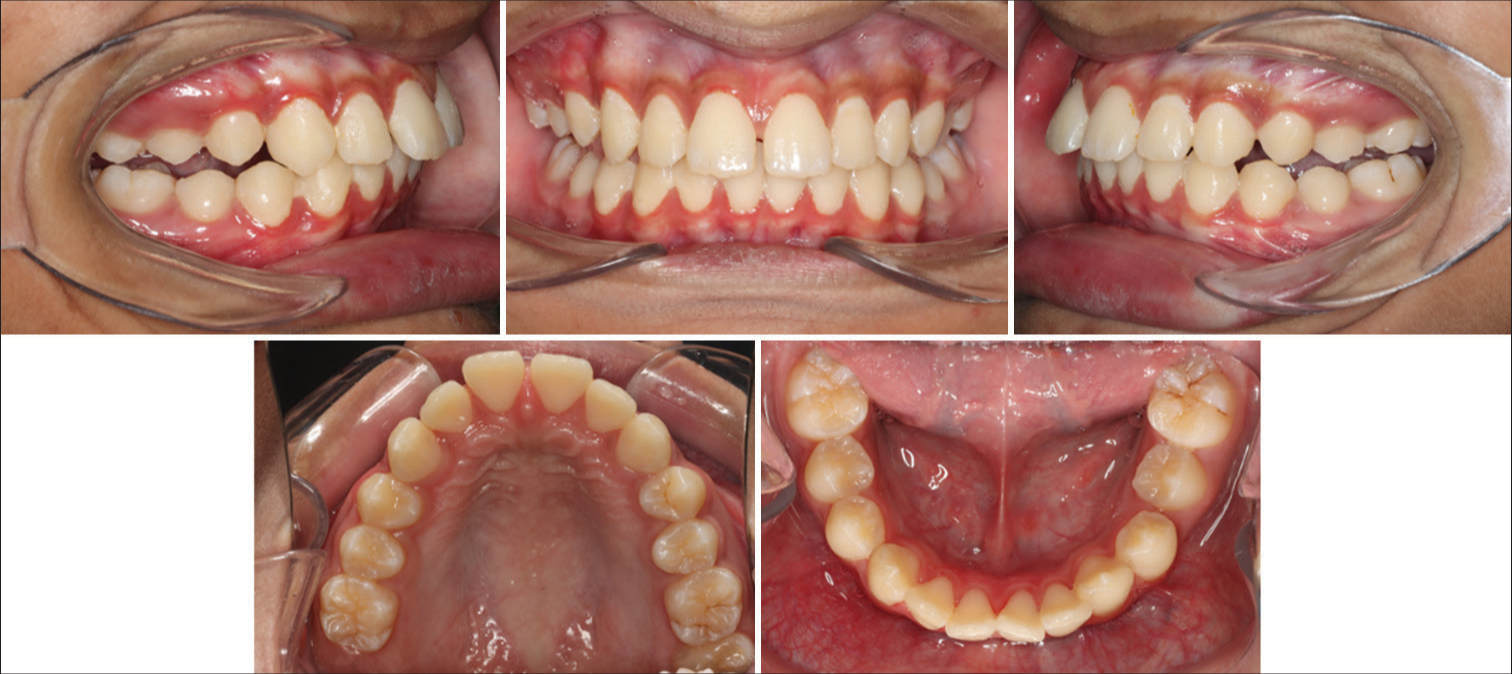
- Post-modified Twin Block appliance photographs.
The removable Twin Block and steep and deep appliance have successfully managed the patient’s malocclusion and achieved the treatment aims of promoting improved dental alignment and oral health 9 months into treatment. Post-treatment lateral cephalogram were taken post removable Twin-Block appliance [Figure 9]. Overall superimposition performed to allow a comprehensive assessment of the skeletal and dental changes that occurred during the treatment [Figure 10].
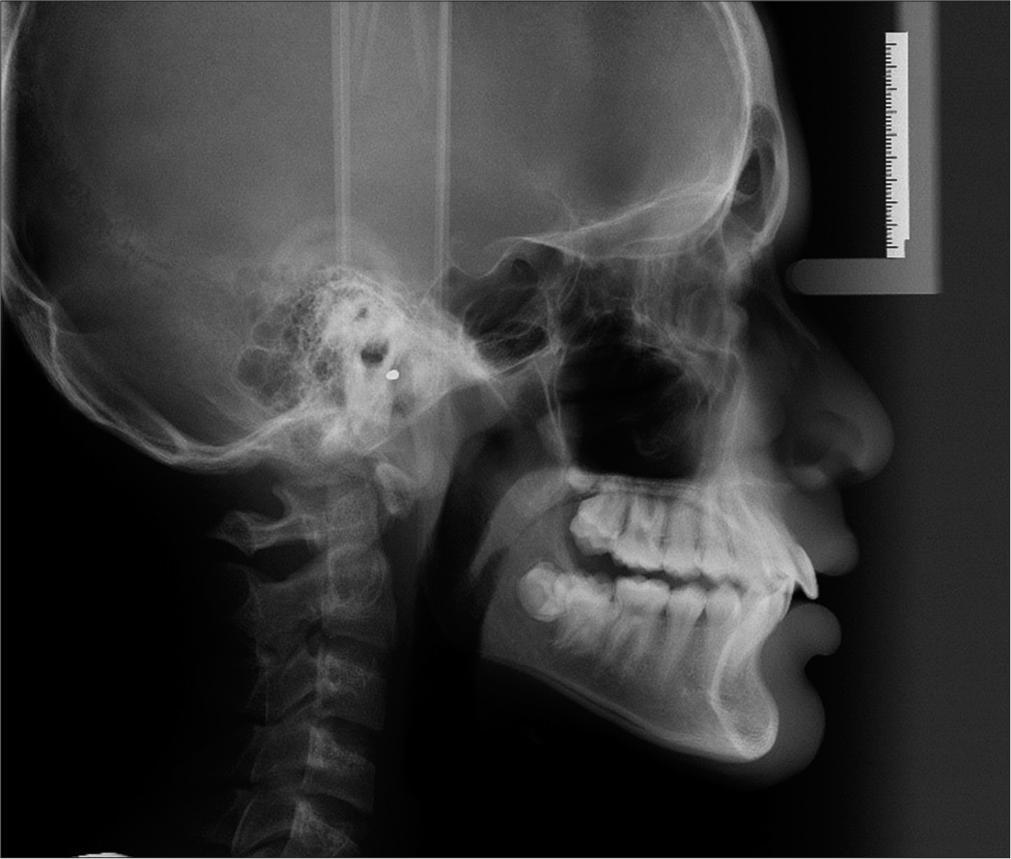
- Post-treatment lateral cephalogram.
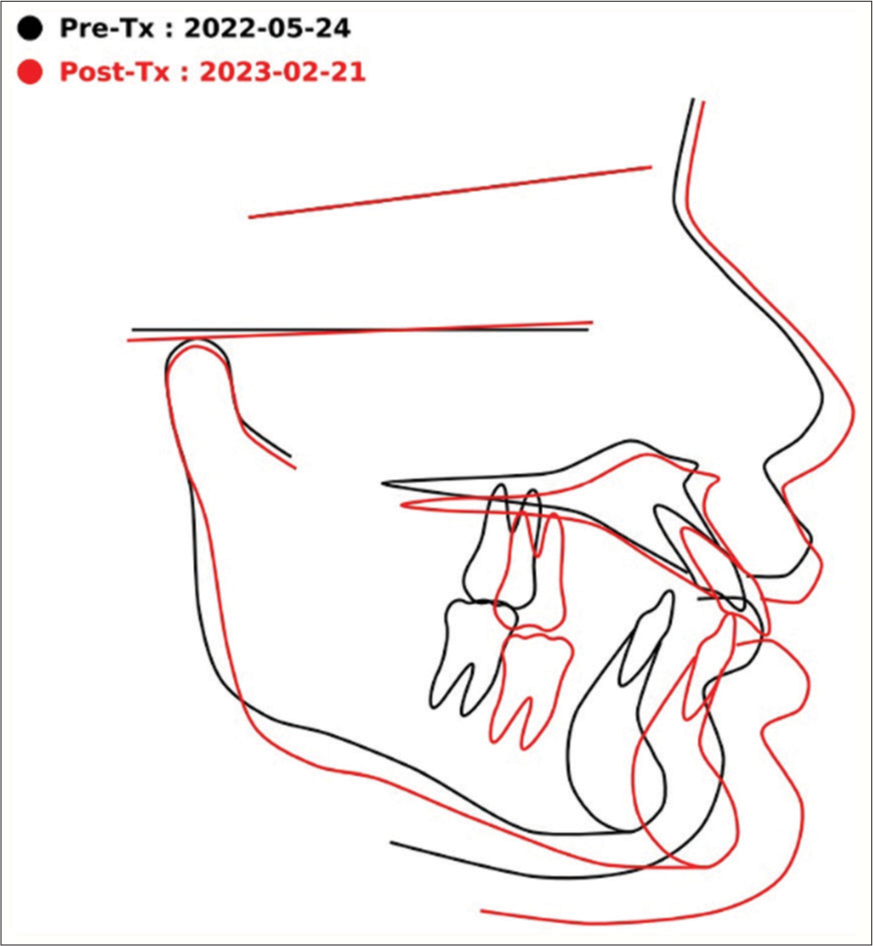
- Overall superimposition. Tx: Treatment
DISCUSSION
In contemporary epidemiological studies, a pronounced and statistically significant increase in the incidence and prevalence of ASD has been documented, reflecting a notable upward trend in diagnostic rates over the past few decades.[19] The most prevalent occlusal deviations reported were increased maxillary overjet and crowding. The current findings additionally offer evidence to substantiate the higher prevalence of Angle’s Class II, Angle’s Class III, open bite, and increased maxillary overjet among individuals with ASD compared to those without ASD.[20-22] For children with ASD, Phase I orthodontic treatment takes on added significance. ASD encompasses a spectrum of neurodevelopmental disorders that can manifest in diverse ways, including sensory sensitivities, communication challenges, and behavioral variations.[23] Therefore, the goals of Phase I treatment must align with these individuals’ specific needs and sensitivities. By addressing orthodontic issues early and with sensitivity to ASD-related considerations, Phase I treatment can enhance oral health, function, and overall well-being for children on the autism spectrum.[18]
When providing orthodontic treatment, particularly Phase I orthodontic treatment, to patients with ASD, we encountered several unique challenges. Some challenges faced during treatment include sensory sensitivities, such as oral sensitivity. MM expresses laughter or other vocalizations in response to the sensation of touch. This reaction does not necessarily imply humor or enjoyment. Alternatively, it could serve as a mechanism for MM to manage the sensory stimuli he is encountering. Laughing or vocalizing can function as a self-soothing mechanism, aiding MM in managing his sensory experiences. This phenomenon can be challenging to understand, but it is essential to recognize that it is a part of their sensory processing differences.[15-18] Individuals with ASD have heightened oral sensitivities, making them more responsive to touch, taste, and texture. This can lead to discomfort or resistance during dental examinations, impressions, and appliance placement. We gradually introduce MM to the dental environment and procedures. Short, low-stress visits at first and gradually increase the complexity of the procedures over time as MM becomes more comfortable. Clear, simple language and communication aids in explaining each step of the process to MM. During impression-taking and bite registration, we employed the “tell-show-do” approach, which involves explaining, demonstrating, and performing the procedure step-by-step to familiarize MM with each step. The dental office environment, with its bright lights, sounds, and unfamiliar sensations, can overwhelm MM, potentially triggering sensory overload. Creating a sensory-friendly dental environment and using specialized dental tools can help reduce sensory sensitivities.[18] Desensitization, positive reinforcement, and distraction can help manage anxiety and improve MM cooperation. We collaborated closely with his mother, who provided valuable insights into the patient’s preferences and comfort strategies. She played an active role in calming and supporting the patient during the visit.
The cooperative attitude of MM in consistently wearing the Twin Block appliance is a remarkable and encouraging aspect of his treatment journey. While ASD is often associated with sensory sensitivities[19,20] and difficulties in adapting to changes or new routines, the successful cooperation of this patient in adhering to orthodontic treatment with a Twin Block appliance underscores their resilience and the effectiveness of tailored strategies for managing sensory challenges. This positive compliance reflects the strategies implied during treatment.[24,25] Effective communication and preparation of sensory accommodation by adapting the Twin Block appliance to be as comfortable and non-intrusive as possible for MM enhance the patient’s acceptance of the appliance.
Next are structured routines and visual supports, whereby visual supports, such as visible schedules or social stories, can assist ASD individuals in comprehending the necessity of wearing the Twin Block appliance as part of their daily routine.[26] Positive reinforcement and reward were tailored to the individual’s preferences and included verbal praise, small treats, or other motivating incentives.[27] Working closely with the patient’s caregivers and the pediatric dentist provided valuable insights and support during treatment.[28,29]
There have been limited documented cases of individuals with ASD receiving orthodontic treatment.[30-32] However, these cases provide valuable insights into the challenges and accomplishments that can arise in such situations. The reported studies for patients with ASD primarily involved simple and non-invasive procedures, including clinical oral examinations, prophylaxis procedures, and fluoride application.[26,33-35] This cooperative engagement of MM successfully underwent a Twin Block Appliance therapy is a testament to the capacity of individuals with ASD to adapt and engage positively when their unique needs are recognized and addressed. An essential insight derived from these exceptional instances is the significance of tailored and patient-focused healthcare.
Orthodontic treatment
Class II correction stems predominantly from dental change (60–70%), with skeletal contribution accounting for the remainder.[36,37] Skeletal change includes an acceleration in mandibular growth during the pubertal growth spurt, leading to improved occlusal and functional outcomes. The initial phase involved growth modification using a modified Clark Twin Block functional appliance to restrain maxillary protrusion and use any remaining mandibular growth of the mandible to improve the facial profile. This approach was justified based on an observed improvement in facial profile when the patient was asked to posture his mandible forward. A Twin Block Appliance can help correct the inter-arch relationships by effectively using it as an anchorage device to retrocline the upper labial segment and correct the overjet and Class II buccal segment relationship.
Moreover, a desired increase in the vertical proportions can be achieved to reduce the deep overbite and improve the lower facial height ratio. For stability, lips competence has been readily established, with the lower lip overlapping the incisal third of the upper central incisors at rest, aiding stability of the corrected overjet. Using a functional appliance has aided in altering the soft-tissue balance to help correct the underlying malocclusion through dentoalveolar changes and favorable skeletal growth to a lesser degree, which may help maintain these changes.
Positive changes in a patient’s oral health, speech, and behavior following Phase I orthodontic treatment, particularly in the context of a patient with ASD, demonstrate the significant impact of early intervention. Proper alignment of teeth and correct malocclusion often make it easier for patients, including those with ASD, to maintain good oral hygiene. Brushing and flossing become more effective. Addressing overjets or protruding teeth can decrease the likelihood of dental injuries. Individuals, including those diagnosed with ASD, are less likely to sustain dental injuries resulting from falls or mishaps. [10] Correcting malocclusion can also alleviate discomfort or pain associated with bite problems. As a result, patients with ASD may exhibit less irritability or discomfort. Enhanced oral esthetics and a more comfortable smile can improve self-esteem and self-image, positively impacting overall behavior and social interactions. For individuals with ASD, addressing oral sensory sensitivities through orthodontic treatment can reduce sensory distress and aversions related to the mouth.
CONCLUSION
Orthodontic treatment can bring about a range of positive changes in a patient’s oral health, speech, and behavior, especially when tailored to the unique needs of individuals with ASD. These changes contribute to improved oral function and esthetics, enhanced overall well-being, and a better quality of life for patients and their families.
Ethical approval
The Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Diagnostic and statistical manual of mental disorders DSM-IV (4th ed). Washington, DC: American Psychiatric Association; 1994. p. :66-71.
- [Google Scholar]
- Diagnostic and statistical manual of mental disorders (DSM-5®) (5th ed). Washington, DC: American Psychiatric Association; 2013.
- [CrossRef] [Google Scholar]
- Epidemiology of autistic disorder and other pervasive developmental disorders. J Clin Psychiatry. 2005;66(Suppl 10):3-8.
- [Google Scholar]
- Dental and social effects of malocclusion and effectiveness of orthodontic treatment: A review. Community Dent Oral Epidemiol. 1980;8:36-45.
- [CrossRef] [PubMed] [Google Scholar]
- Effectiveness of early orthodontic treatment with the Twin-block appliance: A multicenter, randomized, controlled trial. Part 2: Psychosocial effects. Am J Orthod Dentofacial Orthop. 2003;124:488-95.
- [CrossRef] [PubMed] [Google Scholar]
- Bullying in orthodontic patients and its relationship to malocclusion, self-esteem and oral health-related quality of life. J Orthod. 2011;38:247-94.
- [CrossRef] [PubMed] [Google Scholar]
- Is there a relationship between malocclusion and bullying? A systematic review. Prog Orthod. 2020;21:26.
- [CrossRef] [PubMed] [Google Scholar]
- Orthodontic treatment for prominent upper front teeth (Class II malocclusion) in children and adolescents. Cochrane Database Syst Rev. 2018;3:CD003452.
- [CrossRef] [PubMed] [Google Scholar]
- A systematic review of the relationship between overjet size and traumatic dental injuries. Eur J Orthod. 1999;21:503-15.
- [CrossRef] [PubMed] [Google Scholar]
- Children's dental health in the United Kingdom 1983 Survey carried out by the Social Survey Division of the OPCS, on behalf of the United Kingdom health departments, in collaboration with the dental schools of the universities of Birmingham and Newcastle London: HMSO; 1985.
- [Google Scholar]
- Occurrence of oral habits among preschool children with Autism Spectrum Disorder. Pak J Med Sci. 2017;33:1156-60.
- [CrossRef] [PubMed] [Google Scholar]
- Autism and primary care dentistry: Parents' experiences of taking children with autism or working diagnosis of autism for dental examinations. Int J Paediatr Dent. 2018;28:226-38.
- [CrossRef] [PubMed] [Google Scholar]
- Oral health behaviours of preschool children with autism spectrum disorders and their barriers to dental care. J Autism Dev Disord. 2019;49:453-9.
- [CrossRef] [PubMed] [Google Scholar]
- Dental visits for autistic children: A qualitative focus group study of parental perceptions. JDR Clin Trans Res. 2021;8:23800844211049404.
- [CrossRef] [PubMed] [Google Scholar]
- Understanding oral health challenges for children and young people with autistic spectrum conditions: Views of families and the dental team. J Disabil Oral Health. 2018;19:170-4.
- [Google Scholar]
- The experiences of children with autism spectrum disorder, their caregivers and health care providers during day procedure: A mixed methods study. Paediatr Anaesth. 2019;29:927-37.
- [CrossRef] [PubMed] [Google Scholar]
- UK dental professionals' knowledge, experience and confidence when treating patients on the autism spectrum. Br Dent J. 2019;227:504-10.
- [CrossRef] [PubMed] [Google Scholar]
- The rise in the numbers of pupils identified by schools with autism spectrum disorder (ASD): A comparison of the four countries in the United Kingdom. Support Learn. 2020;35:132-43.
- [CrossRef] [Google Scholar]
- Malocclusion characteristics amongst individuals with autism spectrum disorder: A systematic review and meta-analysis. BMC Oral Health. 2022;22:341.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence of malocclusion in Canadian children with autism spectrum disorder. Am J Orthod Dentofacial Orthop. 2017;152:38-41.
- [CrossRef] [PubMed] [Google Scholar]
- Malocclusion complexity and orthodontic treatment need in children with autism spectrum disorder. Clin Oral Investig. 2022;26:6265-73.
- [CrossRef] [PubMed] [Google Scholar]
- The relation of severe malocclusion to patients' mental and behavioral disorders, growth, and speech problems. Eur J Orthod. 2021;43:159-64.
- [CrossRef] [PubMed] [Google Scholar]
- Autism disorder (AD): An updated review for paediatric dentists. J Clin Diagn Res. 2014;8:275-9.
- [Google Scholar]
- Effectiveness of psychological techniques in dental management for children with autism spectrum disorder: A systematic literature review. BMC Oral Health. 2022;22:162.
- [CrossRef] [PubMed] [Google Scholar]
- Evaluation of visual pedagogy in dental check-ups and preventive practices among 6-12-year-old children with autism. J Autism Dev Disord. 2017;47:858-64.
- [CrossRef] [PubMed] [Google Scholar]
- Strategies for success: A qualitative study of caregiver and dentist approaches to improving oral care for children with autism. Pediatr Dent. 2019;41:4E-12.
- [Google Scholar]
- Influence of past advanced behavior guidance experience on parental acceptance for autistic individuals in the dental setting. BMC Oral Health. 2023;23:23.
- [CrossRef] [PubMed] [Google Scholar]
- Management of autistic patients in dental office: A clinical update. Int J Clin Pediatr Dent. 2018;11:219-27.
- [CrossRef] [PubMed] [Google Scholar]
- Removable orthodontic appliance with nickel-titanium spring to reposition the upper incisors in an autistic patient. Spec Care Dentist. 2013;33:35-9.
- [CrossRef] [PubMed] [Google Scholar]
- Extraction orthodontic treatment in an autistic patient. Turk J Orthod. 2017;30:28-32.
- [CrossRef] [PubMed] [Google Scholar]
- Camouflage orthodontic treatment in an autistic class II patient with anterior open bite: Case report. Rev Mex Ortod. 2015;3:e47-55.
- [CrossRef] [Google Scholar]
- Training children with autism spectrum disorder to undergo oral assessment using a digital iPad® application. Eur Arch Paediatr Dent. 2019;20:113-21.
- [CrossRef] [PubMed] [Google Scholar]
- Effectiveness of a preparatory aid in facilitating oral assessment in a group of Saudi children with autism spectrum disorders in Central Saudi Arabia. Saudi Med J. 2017;38:533-40.
- [CrossRef] [PubMed] [Google Scholar]
- Addressing dental fear in children with autism spectrum disorders: A randomized controlled pilot study using electronic screen media. Clin Pediatr (Phila). 2014;53:230-7.
- [CrossRef] [PubMed] [Google Scholar]
- Effectiveness of early orthodontic treatment with the Twin-block appliance: A multicenter, randomized, controlled trial. Part 1: Dental and skeletal effects. Am J Orthod Dentofacial Orthop. 2003;124:234-43. quiz 339
- [CrossRef] [PubMed] [Google Scholar]
- A cephalometric analysis of skeletal and dental changes contributing to Class II correction in activator treatment. Am J Orthod. 1984;85:125-34.
- [CrossRef] [PubMed] [Google Scholar]






