Translate this page into:
Morphological changes of the facial skeleton in Class II/1 patients treated with orthodontic functional appliances
Address for Correspondence: Dr. Dana Feştilă, Department of Orthodontic, Faculty of Dental Medicine, University of Medicine and Pharmacy, “I.Haţieganu”, Cluj-Napoca N. Titulescu Street, no. 147, sc.IV, apt. 33, 400 407 Cluj-Napoca, Romania, 0040 722 286146, E-mail: dana.festila@gmail.com
This article was originally published by Wolters Kluwer and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Aim
The aim of this study was to investigate, using lateral cephalometry, the skeletal changes in maxillary bones induced through functional jaw orthopedic therapy. 30 patients with class II division 1 malocclusion and average age of 10.4 years were included in the study.
Material and Methods
Cephalometric data were analyzed with the following methods: Burstone, McNamara, Rickets, Tweed and Wits and treatment changes were evaluated overlapping the lateral cephalograms on cranial base with sella registered.
Results
The results showed reduced over-jet in average with 2.46 mm, mandibular advancement with a mean value of 2.72 mm and increasing of the total mandibular length with a mean value of 4.17 mm. Although we found an inhibiting in the anterior development of the maxilla with an average of 1.57 degree, the decrease of the anterior-posterior discrepancy was due especially to the mandible.
Conclusions
It can be concluded that functional appliances were effective in correcting class II malocclusion. Changes of the position and mandible’s length determined improved facial profile but did not correct it completely because of the chin that moved not only anterior but also downward, as a result of vertical ramus growth.
Keywords
Facial skeleton
mandibular length
mandibular advancement
functional orthopaedics
INTRODUCTION
Class II malocclusion is the result of the multiple dental and skeletal combinations between mandible and maxilla.[1,2] The name “functional jaw orthopaedic — appliance” refers to a variety of constructions [Figures 1 and 2], all with the same goal: To change the horizontal, vertical and transversal position of the mandible and to produce orthopedic and orthodontic modifications.
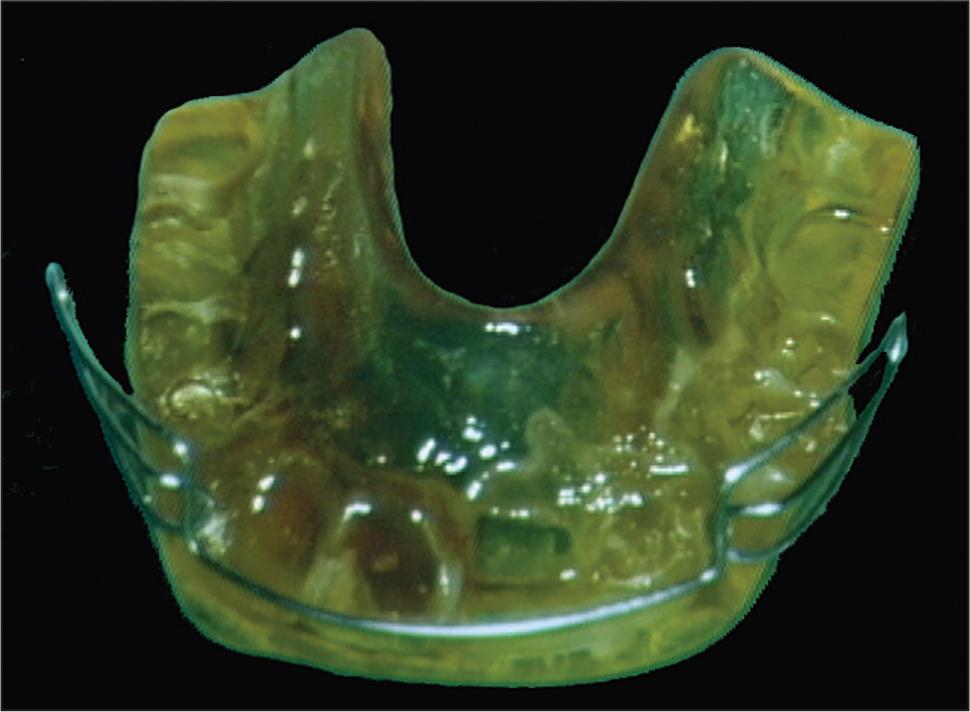
- Classic activator

- Basic bionator
In fact, Class II division 1 (Class II/1) functional treatment stimulates anterior mandibular growth, inhibits the anterior development of the maxilla and produces dental and alveolar changes.
The construction bite is necessary to register the desired intermaxillary relationship in three — dimensions. In other words, the construction bit indicates the therapeutic position of the mandible, to which the appliances will be fabricated [Figures 3, 4a-d and 5a-d].[3]

- Illustration of force vectors when the construction bite positions the mandible forward. A posteriorly directed force is applied to the mandible through the musculature. Force is applied in a posterior direction to the maxillary and in an anterior direction to the mandibular teeth through the intermaxillary dentoalveolar support for the appliance

- Facial and lateral views (a), distal occlusion (b), orthopantomogramm (c) and cephalogramm in the centric relation (d) at the beginning of treatment

- Facial and lateral views (a), Class I occlusion (b), orthopantomogramm (c) and cephalogramm in the centric relation (d) at the end of treatment
Functional jaw orthopedic appliances are designed to take advantage of appliance-induced changes in muscle activity and occlusal functioning rather than extrinsic mechanical forces in the correction of dentofacial malrelationships. Proper application of muscle derived forces can guide and influence the growth of stomatognathic system. The essential factors in achieving morphologic changes are muscle-derived, appliance-induced force application and the restraining of muscle activity. These orthopedic devices are not indicated primarily for the movement of individual teeth, but are of particular value for the following problems: Functional disturbances such as, malrelationships of the jaw in the sagittal, vertical, or transverse dimension, temporo - mandibular joint disturbances, for example, following condylar fracture.
The aim of this study was to investigate, using lateral cephalometry, skeletal changes in maxillary bones induced through functional therapy.
MATERIALS AND METHODS
The sample included 30 patients with class II division 1 malocclusion, 13 boys and 17 girls between 8 and 12.5 years old with an average of 10.4 years. The selection criteria were chosen after those recommended by Bennet in 2007.[4]
Over-jet >11 mm
Dental class II of at least half cusp in molars and canines
Aligned dental arches or light crowding
Skeletal class II (Ao-Bo distance >2 mm)
Hypo divergent or normal facial type
Good compliance • No previous orthodontic treatment
Clinical protocol
All patients were on functional appliance with a mean treatment duration of 2.3 years [Table 1]. For each patient 2 lateral cephalograms, one pretreatment and one at the end of functional phase were traced. The radogrphs were taken using standardized methods and traced with Ony Ceph (version 2.7, Image Instruments GmbH, Germany) and using the following methods: Burstone, McNamara, Rickets, Tweed and Wits.[5] Treatment changes were evaluated overlapping the lateral cephalograms on cranial basal plan with sella point registered and comparing the values of the analyzed issues at the beginning and at the end of treatment.
| Treatment time | Boys (n = 13) | Girls (n = 17) | Total (n = 30) |
|---|---|---|---|
| Initial (T1) | 10.2±1.3 | 10.5±1.4 | 10.4±1.3 |
| Final (T2) | 12.7±1.0 | 12.6±1.4 | 12.7±1.3 |
| Total treatment time (T2-T1) | 2.5±0.9 | 2.1±0.6 | 2.3±0.7 |
The variables used for the assessment of the skeletal facial changes were:
Angular (◦):
Skeletal profile convexity (N-A-Pog)
Facial depth (NPog-POr)
Maxilla depth (NA-POr)
Facial axis (NBa-PtGn)
Relationship of the maxilla to the cranial base (SNA)
Relationship of the mandible to the cranial base (SNB)
Relationship of the mandible to the maxilla and to the cranial base (ANB).
Linear (mm):
Wits appraisal (distance Ao-Bo)
Horizontal ramus length (Go-Pg)
Vertical ramus length (Ar-Go)
Length of the maxilla (ANS-PNS)
Anterior-posterior position of the mandible (N-B, Pn-Pog)
Total length of the maxilla related to the mandible (Co-A)
Total length of the mandible (Co-Gn)
Maxilla-mandible difference (Max-Mandib)
Anterior-posterior position of the maxilla (Pn-A)
Skeletal profile convexity (A-NPog).
The reason for using this large variety of variables belonging to different interpretation methods was to compensate the deficiency of some methods with more information given by others. As for any others anomalies, in Class II/1, skeletal changes might be hidden by dental-alveolar compensations, too. That is why, in some cases, for a single modification, were analyzed more variables.
Statistical data analysis was done with homoscedastic Student,s t-test, which compares two clinical situations with standard-ideal values considered to be characteristic for a control group. The significance of the values was determined by three levels of significance: 0.05 (*), 0.01(**) and 0.001 (***).
RESULTS
The results of this study are shown in Tables 2 and 3.
| Parameters | T1 | SD1 | T2 | SD2 | T2–T1 (Δ) | SD | Significance | Significance level |
|---|---|---|---|---|---|---|---|---|
| Angulars | ||||||||
| N-A-Pog (°) | 7.52 | 7.66 | 5.73 | 7.19 | −1.79 | 4.43 | 0.0354 | * |
| NPog-POr (°) | 86.15 | 3.18 | 86.60 | 1.42 | 0.45 | 2.86 | 0.3920 | NS |
| NA-POr (°) | 89.13 | 5.20 | 90.11 | 3.96 | 0.98 | 2.74 | 0.0599 | NS |
| NBa-PtGn (°) | 85.62 | 3.94 | 86.55 | 3.81 | 0.93 | 3.78 | 0.1880 | NS |
| SNA (°) | 82.33 | 4.22 | 80.77 | 2.99 | −1.57 | 3.19 | 0.0118 | * |
| SNB (°) | 75.40 | 3.63 | 77.93 | 2.99 | 2.72 | 3.67 | 0.0003 | *** |
| ANB (°) | 6.93 | 2.63 | 2.29 | 2.58 | −4.07 | 3.29 | 0.0000 | *** |
| Linears | ||||||||
| A-B (mm) | 3.70 | 1.56 | 1.64 | 2.08 | −2.46 | 1.78 | 0.0000 | *** |
| Go-Pog (mm) | 64.65 | 5.59 | 67.16 | 5.09 | 2.52 | 2.32 | 0.0000 | *** |
| Ar-Go (mm) | 37.86 | 4.52 | 40.30 | 4.36 | 2.44 | 2.96 | 0.0001 | *** |
| ANS-PNS (mm) | 48.03 | 4.56 | 50.96 | 2.78 | 2.94 | 4.58 | 0.0015 | ** |
| N-B (mm) | −12.15 | 5.16 | −8.61 | 3.54 | 3.57 | 3.75 | 0.0000 | *** |
| Cond-A (mm) | 75.93 | 3.31 | 80.00 | 1.55 | 4.07 | 3.81 | 0.0000 | *** |
| Cond-Gn (mm) | 95.33 | 4.38 | 99.50 | 4.08 | 4.17 | 2.94 | 0.0000 | *** |
| Max-Mand (mm) | 19.47 | 2.90 | 19.50 | 4.17 | 0.03 | 2.81 | 0.9486 | NS |
| Pn-A (mm) | −2.03 | 4.48 | −0.17 | 3.07 | 1.93 | 3.01 | 0.0015 | ** |
| Pn-Pog (mm) | −8.53 | 5.05 | −5.10 | 2.90 | 3.43 | 4.45 | 0.0002 | *** |
| A-NPog (mm) | 3.35 | 4.97 | 2.40 | 2.68 | −0.95 | 3.62 | 0.1615 | NS |
SD – Standard deviation; NS – Nonsignificant
| Parameters | T2 | Standard values | Significance | Significance level | ||
|---|---|---|---|---|---|---|
| Mean | SD | Mean | SD | |||
| Angulars | ||||||
| N-A-Pog (°) | 5.73 | 7.19 | 2.6 | 9.31 | 0.1574 | NS |
| NPog-Por (°) | 86.60 | 1.42 | 87 | 5.48 | 0.7049 | NS |
| NA-Por (°) | 90.11 | 3.96 | 90 | 5.48 | 0.9326 | NS |
| NBa-PtG (°) | 86.55 | 3.81 | 90 | 6.39 | 0.0155 | * |
| SNA (°) | 80.77 | 2.99 | 82 | 3.65 | 0.1647 | NS |
| SNB (°) | 77.93 | 2.99 | 80 | 3.65 | 0.0218 | * |
| ANB (°) | 2.29 | 2.58 | 3 | 3.65 | 0.3957 | NS |
| Linears | ||||||
| A-B (mm) | 1.64 | 2.08 | −0.4 | 4.56 | 0.0329 | * |
| Go-Pog (mm) | 67.16 | 5.09 | 74.3 | 10.59 | 0.0018 | ** |
| Ar-Go | 40.30 | 4.36 | 46.8 | 4.56 | 0.0000 | *** |
| ANS-PNS (mm) | 50.96 | 2.78 | 52.6 | 6.39 | 0.2109 | NS |
| N-B (mm) | −8.61 | 3.54 | −6.9 | 7.85 | 0.2894 | NS |
| Cond-A (mm) | 80.00 | 1.55 | — | — | — | — |
| Cond-Gn (mm) | 99.50 | 4.08 | 98.5 | 2.74 | 0.2779 | NS |
| Max-Mand (mm) | 19.50 | 4.17 | 18.5 | 2.74 | 0.2846 | NS |
| Pn-A (mm) | −0.17 | 3.07 | 0.4 | 4.20 | 0.5599 | NS |
| Pn-Pog (mm) | −5.10 | 2.90 | −1.8 | 8.22 | 0.0460 | * |
| A-Npog (mm) | 2.40 | 2.68 | 2 | 3.65 | 0.6364 | NS |
NS – Nonsignificant
Facial profile convexity angle (N-A-Pog) decreased with a mean value of 1.79 degree (P < 0.05). The same linear variable (mm) decreased from 3.35 mm to 2.40 mm, although not statistically significant. Facial depth angle, the angle of the maxilla and facial axis angle increased not statistically significant.
The maxilla moved posterior with respect to the cranial base, SNA angle decreased from 82.33 to — 80.77, with a mean value of 1.57 (P < 0.05). The mandible advanced, SNB angle increased from 75.40 to 77.93, with a mean value of 2.72 (P < 0.001); anterior-posterior discrepancy (ANB angle, Ao-Bo distance) reduced from 6.93 to 2.29 with a mean value of 4.07, from 3.70 mm to 1.64 mm with a mean value of 2.46 mm (P < 0.001) respectively. Mandibular advancement was sustained also by the evaluation of Pn-Pog distance which decreased with a mean value of 3.43 mm (P < 0.001) and N-B distance which decreased with a mean score of 3.57 mm (P < 0.001). On the other hand, posterior orientation of the maxilla is contradicted by the Pn-A distance which increased from −2.03 mm to −0.17 mm (P < 0.01). Even though, the evolution of this variable might be considered favorable if it is related to normal value (0-1 mm).
Regarding the mandible length it can be seen the increased length of both, vertical and horizontal parts (the vertical one, Ar-Go, increased with a mean value of 2.44 mm and the horizontal ramus Go-Gn, increased with a mean value of 2.52 mm) and total mandibular length which is greater with 4.17 mm (mean value). For all these variables, P < 0.001. The length of the maxilla measured at ANS-PNS is greater at the end of treatment (2.94 mm, P < 0.01) too, and also related to the total mandibular length, Co-A (4.07 mm, P < 0.001). The difference between the two bones remains about the same at the end of functional treatment (0.03 mm could be considered a statistically insignificant value). We can say that the two bones were growing in parallel keeping the same ratio under the treatment also.
The skeletal variables that have reached ideal values at the end of treatment (P < 0.05) were:
Those that describe the anterior-posterior position of the mandible (SNB, ANB angles, Ao-Bo, Pn-Pog, N-B distances) and its total length (Co-Gn).
Those that describe the skeletal profile convexity (A-NPog).
DISCUSSION
The necessity of orthodontic treatment in Class II/1 cases is necessary because dental and facial appearance is worsening with growth and there is no tendency for spontaneously correction even in the presence of horizontal growth vector.[6] Appropriate treatment timing guarantee orthopedic changes capable to reduce the anterior-posterior discrepancy by modifying the mandibular position and not through dental camouflage.
The main skeletal change that results from our study is mandibular advancement. Nevertheless, this “advancement” is not only due to changes in mandibular position but also to an increase in horizontal and vertical ramus length as well as to an increase in the total mandibular length. A similar observation was made by Pangrazio-Kulbersh et al.[7] Guney and Ackam have obtained similar results with ours in Class II/1 Turkish patients treated with a conventional activator, total mandibular length in their study being 4.8 mm compared with our value of 4.17 mm.[8]
After 3.8 years of study on a lot of 23 Class II untreated patients, Baccetti et al.have reported that under the influence of normal growth, the length of the mandible is changing with 0 to 1.2 mm.[9] A previous study, 14.5 months long, on Brazilian Class II untreated subjects of Gomes and Lima, has reported an annual growth rate of 2.16 mm for the horizontal ramus, 3.16 mm for the vertical ramus and 4.31 mm for the total mandibular length.[10] Comparing our study with those from Baccetti and Guney, we can conclude that functional treatment induces a supplementary growth of the mandible. From Gomez and Lima aspect, there are no differences between the amount of growth induced by functional therapy and normal growth. The differences could occur because of ethnical individual variations.
Therefore, mandibular advancement could be the result of two processes: Increasing in length and anterior displacement, as a result of temporo-mandibular joint remodeling [Figure 6]. This observation of our study is in accordance with those of Jones, Pangrazio-Kulbersch, Mills, McNamara senior, Birkebaek, Woodside, Arat and Chen.[1,7,11-17] There are also other theories: Johnston and Livieratos say that functional appliances do not produce a supplementary mandibular growth, only accelerate that already existing,[18,19] and Pancherz, Wieslander, Vargevick and Harvold, Paulsen and Ruf state that functional therapy helps the mandible to express its genetic growth potential through anterior repositioning.[20-24] This position could stimulate condylar growth.[25] The fourth category, represented by Gianelly, Andria, Schulhof et al. say that there is no difference between mandibular changes produced by functional therapy and those produced by normal growth or Class II conventional edgewise treatment.[26-28]

- Temporo-mandibular joint remodeling
Although the length of the maxilla increased probably as result of normal growth, decreased value of the SNA angle at the end of treatment demonstrates the inhibition in anterior development of the maxilla and posterior repositioning from cranial base. This is the so-called “head-gear effect” of the functional appliances, referred to many studies belonging to Owen, Hotz, Mills, Harvold, Pancherz, Macey-Dare, Collet and Marçan.[29-37] Taking into account that in our study variation in SNB angle is greater than in SNA and the maxilla-mandible difference remains the same during treatment, we can consider that the horizontal discrepancy correction between the maxilla and the mandible is mainly due to the mandible. This result is in accord with the conclusion of a meta-analyses study of Antonarakis and Kiliarides which states that functional orthopedic treatment effects are more obvious in the mandible except the cases treated with twin-block or associated head-gear which show modifications in both, maxilla and mandible.[38]
Even the mandible changed its position and length, these are not totally reflected in osseous chin advancement, probably because consequently increasing of the facial height as a result of increased vertical ramus length. This aspect is mentioned in literature by Toth and McNamara jr., Livieratos and Lai.[19,39] Although point pogonion (Pog) translated anterior, at the end of treatment it is located at 5.10 mm posterior from the perpendicular through nasion point (N) on Frankfurt plan, too much compared with ideal mean value of 1.80 mm behind this plan. Due to this, the convexity of the facial skeletal profile was not completely reduced.
Chin advancement was confirmed by the decreased distance from B point to the same reference line and the increased value of SNB angle. Three randomized clinical trials of Tulloch, Ghafari, Keeling et al. have proven the correction of chin position because of the anterior moving of point B.[40-42]
CONCLUSIONS
As a result of the functional treatment important changes in the facial skeletal compartment took place. Functional orthopedic treatment produced mandibular advancement.
Functional appliances induced an increase in mandibular length, in both horizontal and vertical ramus and also in the total dimension.
Changes of the position and mandibular length determined improved facial profile but did not correct it completely because of the chin that moved not only anterior but also downward, as a result of vertical ramus growth. Although we found an inhibiting in the anterior development of the maxilla, the decrease of the anterior-posterior discrepancy was due especially to the mandible.
Source of Support:
Nil.
Conflict of Interest:
None declared.
References
- Class II non-extraction patients treated with the Forsus Fatigue Resistant Device versus intermaxillary elastics. Angle Orthod. 2008;78:332-8.
- [Google Scholar]
- Contemporary Orthodontics. St. Louis: Mosby, Elsevier; 2007. p. :160. 207-17
- Orthodontic management of uncrowded class II division 1 malocclusion in children. Eur J Orthod. 2007;29:109-10.
- [Google Scholar]
- Role of lateral cephalograms in assessing severity and difficulty of orthodontic cases. Am J Orthod Dentofacial Orthop. 2001;120:254-62.
- [Google Scholar]
- Treatment effects of the mandibular anterior repositioning appliance on patients with Class II malocclusion. Am J Orthod Dentofacial Orthop. 2003;123:286-95.
- [Google Scholar]
- Treatment timing for functional treatment of class II division 1 malocclusions. Abstract Book 82nd EOS Congress. :102.
- [Google Scholar]
- Dentofacial growth changes in subjects with untreated Class II malocclusion from late puberty through young adulthood. Am J Orthod Dentofacial Orthop. 2009;135:148-54.
- [Google Scholar]
- The effect of functional appliances on the skeletal pattern. Br J Orthod. 1991;18:267-75.
- [Google Scholar]
- Skeletal and dental changes following functional regulator therapy on class II patients. Am J Orthod. 1985;88:91-110.
- [Google Scholar]
- Long-term mandibular adaptations to protrusive function: An experimental study in Macaca mulatta. Am J Orthod Dentofacial Orthop. 1987;92:98-108.
- [Google Scholar]
- A laminagraphic study of the alterations in the temporo-mandibular joint following activator treatment. Eur J Orthod. 1984;6:257-66.
- [Google Scholar]
- The influence of functional appliance therapy on glenoid fossa remodeling. Am J Orthod Dentofacial Orthop. 1987;92:181-98.
- [Google Scholar]
- Changes in the TMJ disc-condyle-fossa relationship following functional treatment of skeletal Class II Division 1 malocclusion: A magnetic resonance imaging study. Am J Orthod Dentofacial Orthop. 2001;119:316-9.
- [Google Scholar]
- Analysis of efficacy of functional appliances on mandibular growth. Am J Orthod Dentofacial Orthop. 2002;122:470-6.
- [Google Scholar]
- Functional appliances: A mortgage on mandibular position. Aust Orthod J. 1996;14:154-71.
- [Google Scholar]
- A comparison of one-stage and two-stage nonextractionalternatives in matched Class II samples. Am J Orthod Dentofacial Orthop. 1995;108:118-31.
- [Google Scholar]
- Treatment of class II malocclusions by jumping the bite with the Herbst appliance. A cephalometric investigation. Am J Orthod. 1979;76:423-42.
- [Google Scholar]
- Intensive treatment of severe Class II malocclusions with a headgear-Herbst appliance in the early mixed dentition. Am J Orthod. 1984;86:1-13.
- [Google Scholar]
- Response to activator treatment in Class II malocclusions. Am J Orthod. 1985;88:242-51.
- [Google Scholar]
- CT-scanning and radiographic analysis of temporomandibular joints and cephalometric analysis in a case of Herbst treatment in late puberty. Eur J Orthod. 1995;17:165-75.
- [Google Scholar]
- Temporo-mandibular joint remodeling in adolescents and young adults during Herbst treatment: A prospective longitudinal magnetic resonance imaging and cephalometric radiographic investigation. Am J Orthod Dentofacial Orthop. 1999;115:607-18.
- [Google Scholar]
- Functional appliance therapy accelerates and enhances condylar growth. Am J Orthod Dentofacial Orthop. 2003;123:40-8.
- [Google Scholar]
- Mandibular growth, condyle position and Fränkel appliance therapy. Angle Orthod. 1983;53:131-42.
- [Google Scholar]
- Early orthopedics In: Stewart RE, Barber TK, Troutman KC, eds. Pediatric Dentistry: Scientific Foundations and Clinical Practice. St. Louis: CV Mosby; 1982. p. :417-50.
- [Google Scholar]
- Morphologic changes in the sagittal dimension using the Fränkel appliance. Am J Orthod. 1981;80:573-603.
- [Google Scholar]
- Application and appliance manipulation of functional forces. Am J Orthod. 1970;58:459-78.
- [Google Scholar]
- Clinical control of cranio-facial growth: A skeptic’s viewpoint In: Mcnamara JA, ed. Clinical Alteration of the Growing Face. Ann Arbor: Center for Human Growth and Development, University of Michigan; 1983. p. :17-39.
- [Google Scholar]
- The mechanism of Class II correction in Herbst appliance treatment. A cephalometric investigation. Am J Orthod. 1982;82:104-13.
- [Google Scholar]
- Functional appliances: Mode of action and clinical use. Dent Update. 1999;26:240-4. 246
- [Google Scholar]
- Current concepts on functional appliances and mandibular growth stimulation. Aust Dent J. 2000;45:173-8.
- [Google Scholar]
- Effects of activator and high-pull headgear combination therapy: Skeletal, dentoalveolar, and soft tissue profile changes. Eur J Orthod. 2007;29:140-8.
- [Google Scholar]
- Short-term anteroposterior treatment effects of functional appliances and extraoral traction on class II malocclusion. A meta-analysis. Angle Orthod. 2007;77:907-14.
- [Google Scholar]
- Treatment effects produced by the twin-block appliance and the FR-2 appliance of Fränkel compared with an untreated Class II sample. Am J Orthod Dentofacial Orthop. 1999;116:597-609.
- [Google Scholar]
- An evaluation of two-phase treatment with the Herbst appliance and preadjusted edgewise therapy. Semin Orthod. 1998;4:46-58.
- [Google Scholar]
- Benefit of early Class II treatment: Progress report of a two-phase randomized clinical trial. Am J Orthod Dentofacial Orthop. 1998;113:62-72.
- [Google Scholar]
- Headgear versus function regulator in the early treatment of Class II, division 1 malocclusion: A randomized clinical trial. Am J Orthod Dentofacial Orthop. 1998;113:51-61.
- [Google Scholar]
- Anteroposterior skeletal and dental changes after early Class II treatment with bionators and headgear. Am J Orthod Dentofacial Orthop. 1998;113:40-50.
- [Google Scholar]






