Translate this page into:
Root resorption following periodontally accelerated osteogenic orthodontics
Address for Correspondence: Prof. Donald J. Ferguson, Ibn Sina Building, Block D, 3rd Floor, Office 302, Dubai Healthcare City, P.O. Box 53382, Dubai, United Arab Emirates. E-mail: fergusonloud@gmail.com
This article was originally published by Wolters Kluwer and was migrated to Scientific Scholar after the change of Publisher.
How to cite this article: Ferguson DJ, Machado I, Wilcko MT, Wilcko WM. Root resorption following periodontally accelerated osteogenic orthodontics. APOS Trends Orthod 2016;6:78-84.
Abstract
Background
Literature evidence suggests that root resorption, an adverse side effect of orthodontic therapy, may be decreased under conditions of alveolar osteopenia, a condition characterized by diminished bone density and created secondary to alveolar corticotomy (Cort) surgery.
Purpose
To compare root resorption of the maxillary central incisors following nonextraction orthodontic therapy with and without Cort surgery.
Materials and Methods
The sample comprised two groups, with and without Cort and was matched by age and gender: Cort-facilitated nonextraction orthodontics with 27 subjects, 53 central incisors of mean age 24.8 ± 10.2 years, and conventional (Conv) nonextraction orthodontics with 27 subjects, 54 incisors with mean age of 19.6 ± 8.8 years. All periapical radiographs were taken with the paralleling technique; total tooth lengths of the right and left central incisors were measured by projecting and enlarging the periapical radiographs exactly 8 times.
Results
t-tests revealed a significant decrease in treatment time in the Cort group (6.3 ± 8.0 vs. 17.4 ± 20.2 months,P = 0.000). Pretreatment root lengths were not significantly different (P = 0.11), but Conv had significantly shorter roots at posttreatment when compared with Cort (P = 0.03). Significant root resorption (P < 0.01) occurred in both Cort (0.3 mm) and Conv (0.7 mm), but the increment of change was significantly greater in Conv (P < 0.03). The variable SNA increased significantly in the Cort (P = 0.001) group and decreased significantly in the Conv group (P < 0.001).
Conclusions
Based on the conditions of this study, it may be concluded that Cort-facilitated nonextraction orthodontic therapy results in less root resorption and enhanced alveolar support within a significantly reduced clinical service delivery time frame. Rapid orthodontic treatment and reduced apical root resorption are probably due to the transient osteopenia induced by the Cort surgery and inspired by regional acceleratory phenomenon.
Keywords
Alveolar corticotomy
orthodontic treatment
root resorption
INTRODUCTION
Apical root resorption is perceived as an adverse side effect of orthodontic treatment. Ketcham[1] first described root resorption in 1927, and the topic has been the focus of substantial orthodontic research attention ever since. A question still debated is whether the particular method of orthodontic treatment influences the amount of root shortening observed. Brezniak and Wasserstein[2,3] presented a comprehensive review of the literature on root resorption and considered several biological, mechanical, and clinical factors. Identified as the most prevalent factors in root resorption were treatment time, magnitude of force delivered, and distance of tooth movement. The authors concluded that the amount of resorption might not be anticipated with certainty based on any of the reported etiologic factors. The present review of the literature will focus on two factors: Treatment time and bone density.
Several investigations have studied the relationship between bone density and apical root resorption, but there is no consensus. Some authors have reported greater resorption of tooth roots moved orthodontically through bone of high density.[4,5] Goldie and King[6] observed decreased levels of root surface resorption and enhanced tooth movement in lactating rats fed with a diet deficient in calcium. These authors suggested that increased bone resorption and decreased bone density facilitate remodeling of alveolar bone with minimal effects on the roots. Engström et al.[7] also studied rats maintained in dietary hypocalcemia and found an increase in root resorption; it was suggested that the increase in root resorption was related to an enhanced alveolar bone turnover. Wainwright[8] found bone density to be a factor unrelated to root resorption.
Studies regarding the duration of orthodontic treatment and root resorption have yielded contradictory results. Rudolph[9] showed that the incidence of root resorption increases with each year of treatment. DeShields,[10] Stenvik and Mjör,[11] and McFadden et al.[12] revealed that prolonged treatment time was statistically and significantly correlated to root resorption. In a larger study by Linge and Linge,[13] treatment time and therapy with a rectangular arch wire and Class II elastics were found to contribute significantly to root resorption. Results reported by Levander and Malmgren[14] were consistent with Goldson and Henrikson;[15] both studies found that teeth with irregular root contour or minor root resorption after the initial 6 to 9 months indicated a risk for severe root resorption. Baumrind et al.[16] concluded that increased length in treatment time in orthodontically treated adults was indirectly associated with the increased root resorption; Baumrind reasoned that the longer patients were in treatment, the further the teeth were displaced. Taithongchai et al.[17] found a weak but highly significant correlation between treatment time and the amount of apical root resorption. According to this study, treatment time was the best estimator of apical root resorption even though high- and low-risk patients could not be identified. Sameshima and Sinclair[18,19] found a significant correlation between the duration of treatment and the amount of apical root resorption for maxillary central incisor tooth group. In sharp contrast are the results reported by Phillips,[20] VonderAhe,[21] and Mirabella and Artun,[22] who concluded that root resorption does not increase as a function of treatment time.
Corticotomy (Cort) facilitated orthodontics has been presented as a therapy including rapid tooth movement and significantly reduced treatment time. Kole[23] and Suya[24] described Cort as a process of moving blocks of bone rather that moving only teeth themselves. Both authors reported anecdotal findings of little apical root resorption, no loss of tooth vitality, and no pocket formation. These authors surmised that the teeth move faster because the resistance of the cortical bone is reduced by the surgical procedure.
Liou and Huang[25] reported minimal root resorption in a periodontal ligament technique of rapid canine retraction with a distraction device capable of delivering orthopedic force levels. The canine was distracted immediately following extraction of the first premolars and surgical alteration of the socket adjacent to the canine. Liou averaged 6.5 mm of cuspid retraction in 3.5 weeks and contended that the periodontal ligament re-organized with no adverse sequelae or negative impact on the periodontium in long term.
Frost[26] introduced the term regional acceleratory phenomenon (RAP) as an account of the normal, local spatiotemporal soft- and hard-tissue healing events subsequent to a noxious stimulus. Tissue turnover is increased and the intensity of its response depends directly on the magnitude and proximity of the stimulus. RAP healing, according to Frost, involved accelerated bone turnover and decreased bone densities (osteopenia). Healing in response to a stimulus occurs 2–10 times faster than it would in normal regeneration processes. The RAP begins within a few days of the injury and typically peaks at 1–2 months, but it can last from 6 to 24 months. Frost[27] found that when the RAP resolves, the transient osteopenia disappears.
Wilcko et al.[28] introduced a technique called accelerated osteogenic orthodontics (AOO) or periodontally AOO. Immediately following the placement of active, fixed orthodontic appliances for comprehensive therapy, selective labial and lingual decortication of the alveolar bone housing the teeth is performed. An alloplastic bone graft is applied directly on the bleeding labial and lingual alveolar bone, and the soft tissue flap is closed. Two weeks after the surgery and every 2 weeks thereafter, the orthodontic appliance is reactivated. Wilcko protocol results in decreased treatment time, no loss of tooth vitality, no significant apical root resorption, and no periodontal pocketing. Computed tomography scans suggested that the rapid tooth movement was due to de-mineralization of the alveolar bone surrounding the teeth immediately adjacent to the Cort. This finding strongly suggested that rapid tooth movement was due to a process of alveolar de-mineralization and re-mineralization.[29]
Compared to orthodontic therapy without Cort, treatment times were found to be 3–4 times more rapid.[30] Moreover, a significant increase in alveolar bone volume was demonstrated by combining alveolar surgical decortication and alveolar augmentation procedures.[31,32]
The aim of this study was to compare root resorption of the maxillary central incisor following nonextraction orthodontic therapy, with and without Cort surgery. The null hypotheses tested were no difference in root length immediately following active orthodontic treatment, with and without alveolar decortication therapy.
MATERIALS AND METHODS
Sample
The sample comprised two orthodontically treated nonextraction patient groups, with and without alveolar Cort surgery; the nonsurgery group was designated by the term “conventional (Conv).” In the Conv group, there were 27 subjects (20 females and 7 males), who underwent Conv nonextraction orthodontic therapy. In the Cort group, there were 27 subjects (19 females 8 males), who underwent orthodontic nonextraction therapy in combination with alveolar corticotomies and augmentation bone grafting. The two samples were matched (P > 0.05) not only for gender, but also for pretreatment age; Conv mean age was 19.6 ± 8.8 years and Cort mean age was 24.8 ± 10.2 years. Active treatment time was significantly shorter in Cort (6.3 ± 2.4 vs. 17.2 ± 6.5 months,P < 0.001) [Table 1].
| Variable | Corticotomy (n=27) | Conventional (n=27) | X diff | P | ||
|---|---|---|---|---|---|---|
| X SD | X SD | |||||
| Pre-Tx age | 24.8 | 10.2 | 19.6 | 8.8 | 5.2 | NS |
| (years) | ||||||
| Tx time | 6.3 | 2.4 | 17.2 | 6.5 | −10.9 | 0.000 |
| (months) | ||||||
Note there is no difference in pretreatment ages and significantly shorter treatment time for corticotomy. NS – Not significant; SD – Standard deviation
All subjects underwent orthodontic treatment utilizing edgewise, straight wire 0.022” slot brackets and straight wire treatment philosophy (progression through increasing arch wire sizes). The same orthodontic private practice clinician treated all Cort-facilitated patients. All Conv patients were treated by residents in an advanced training orthodontic program under supervision of an orthodontist instructor.
The Cort sample was retrieved from the private practice patient files of Drs. Thomas and William Wilcko; all patient records available satisfying selection criteria were used in the present study. The same operator technician using the same radiographic equipment took all periapical and lateral cephalometric radiographs in the Cort sample. For the Conv sample, periapical and lateral cephalometric radiographs were retrieved from archived patient treatment records at the Saint Louis University Orthodontic Department, starting from most recent until a satisfactory number of patients per age and gender had been retrieved matching the Cort sample. All periapical radiographs were taken using the paralleling technique; a variety of residents and one radiology technician secured the radiographs for the Conv sample.
Criteria for selection included the following:
Availability of pretreatment and posttreatment lateral cephalograms
Availability of pretreatment and posttreatment intraoral periapical radiographs of the maxillary central incisors taken with long-cone, paralleling technique
Presence of the incisal edge and the apex of the maxillary central incisors on the periapical radiograph.
Exclusion criteria were as follows: (1) History of endodontic treatment or trauma as determined from the patient history and/or periapical radiographs, and/or (2) alteration of the incisal edge of a maxillary central incisor.
Periapical radiographic technique
Periapical radiographs were examined for the pretreatment (T1) and posttreatment (T2) study periods for all subjects. The study comprised 54 subjects, which included 107 permanent right and left maxillary central incisors. Each periapical was mounted in a 2 × 2 slides holder and projected onto a wall using a Kodak carousel projector to enlarge the image exactly 8 times the actual size. The projected image of the maxillary central incisors was then traced on a piece of 8.5 × 14 inch white paper with a 2HB lead pencil and appropriately labeled.
Apical root resorption was evaluated utilizing the total tooth length technique described by Mirabella (1995), Lee (1999), and Sameshima (2001a, 2001b). Tooth length was measured from the incisal edge to the root apex along the long axis of the tooth. The amount of root resorption was calculated in millimeters based upon the difference in overall tooth length from pretreatment to posttreatment. A digital vernier caliper (Mitutoyo Mfg. Co., Ltd., Japan) was used to record the tooth length to the nearest 10th of a millimeter [Figure 1].
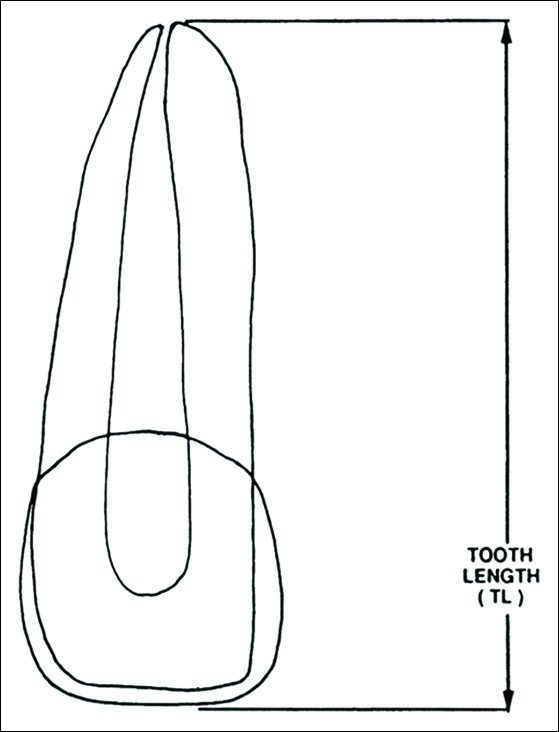
- Calculation of apical root resorption was based on the following computation: TLF = TL1–TL2; where, TLF = Tooth length final, TL1 = Pretreatment tooth length, and TL2 = Posttreatment tooth length
Cephalometric technique
Lateral cephalometric radiographs were examined for the pretreatment (T1) and posttreatment (T2) study periods for all subjects. Each lateral cephalogram was traced on frosted acetate by the investigator, and the most anteriorly positioned central incisor was used in the analysis. The following five cephalometric measurements were made for the purpose of relating the amount of root resorption to the amount of linear and angular change in the axial inclination of the maxillary central incisors: SNA, U1-Sn, U1-NA, U1-NA, and U1-PP [Figure 2].

- Cephalometric angular and linear measurements used in the study. A: SNA (°), B: U1-SN (°), C: U1-NA (°), D: U1-NA (mm), E: U1-PP (°)
Statistical analysis
Statistical analysis of the data was performed using Statistical Package for Social Services (SPSS) software, version 15.0.1, IBM, Armonk, NY, USA. Paired t-test was used to determine intragroup differences due to therapy (T1 to T2 comparisons). Independent t-test was used to identify intergroup differences with significance probability set at P ≤ 0.05.
Experimental error
To evaluate the error in the landmark identification and measurements, 15 pretreatment, posttreatment cephalograms and periapical radiographs were randomly retraced and re-measured at two different occasions separated by 2 weeks. The error of method was calculated with the Dahlberg’s formula: , Where D was the difference between two repeated measurements and N was the number of double measurements made. In the present study, 15 sets of pretreatment and posttreatment cephalograms as well as periapical radiographs were retraced and re-measured to determine the reliability of the measurement technique. According to the Dahlberg formula, the mean error in assessing tooth length was 0.27 mm, SNA was 0.49°, U1-SN was 0.62°, U1-Nad was 0.61°, U1-Namm was 0.52, and U1-PP was 0.49°.
RESULTS
Intergroup comparisons
Independent t-testing between the two study groups matched for gender and pretreatment age demonstrated that treatment time was significantly shorter in the Cort sample (6.3 months) compared with the Conv (17.4 months,P = 0.000) sample [Table 1]. Homogeneity (P > 0.05) was found in pretreatment root length, and only cephalometric study variable SNA was significantly larger in the Conv group (84.0°) compared with Cort (79.4°,P = 0.001) prior to therapy. Intergroup comparisons demonstrated 1.1 mm greater root resorption in the Conv group when compared with Cort (25.7 vs. 26.8 mm,P = 0.03) at posttreatment [Table 2].
| Pretreatment (n=27) | X diff | P | Posttreatment | X diff | P | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Corticotomy Conventional | Corticotomy Conventional | |||||||||||
| X SD X SD | X SD X SD | |||||||||||
| Tooth length | 27.1 | 2.2 | 26.4 | 1.6 | 0.8 | NS | 26.8 | 2.4 | 25.7 | 1.7 | 1.1 | 0.03 |
| SNA | 79.5 | 4.3 | 83.9 | 3.5 | −4.4 | 0.001 | 80.2 | 4.2 | 82.9 | 3.5 | −2.7 | NS |
| U1-SN | 103.7 | 8.6 | 101.3 | 9.5 | 2.4 | NS | 103 | 8.6 | 102.0 | 6.8 | 1 | NS |
| U1-NAa | 23.5 | 7.3 | 18.5 | 8.1 | 5 | NS | 22.7 | 7.3 | 19.5 | 6.9 | 3.3 | NS |
| U1-NAm | 5.9 | 2.9 | 3.8 | 3.1 | 2.1 | NS | 4.9 | 2.8 | 4.0 | 3.4 | 0.9 | NS |
| U1-PP | 111.5 | 8.8 | 108.9 | 10.9 | 2.7 | NS | 110.8 | 7.8 | 110.9 | 7.3 | 0.09 | NS |
NS – Not significant; SD – Standard deviation
Intragroup effects of therapy evaluated using paired t-testing demonstrated significant root shortening in both study groups: Conv roots shortened an average of 0.7 mm from 26.4 to 25.7 mm (P = 0.001) and Cort roots shortened an average of 0.3 mm from 27.1 to 26.8 mm (P = 0.007). Effects of therapy on the cephalometric study variable SNA was significant in both groups: Conv SNA decreased 1.0° from 83.9° to 82.9° (P = 0.000); however, SNA significantly increased in Cort 0.7° from 79.4° to 80.1° (P = 0.001) during therapy [Table 3].
| Variable | T2−T1 (n=27) | |||
|---|---|---|---|---|
| Corticotomy | Conventional | |||
| X diff | P | X diff | P | |
| Tooth length | −0.3 | 0.007 | −0.7 | 0.001 |
| SNA | 0.7 | 0.001 | −1.0 | 0.000 |
| U1-SN | −0.7 | NS | 0.7 | NS |
| U1-NAa | −0.8 | NS | 1.0 | NS |
| U1-NAm | −1.0 | NS | 0.2 | NS |
| U1-PP | −0.7 | NS | 2.0 | NS |
Note that in both groups only variables, tooth length and SNA showed significant change due to therapy. NS – Not significant; SD – Standard deviation
DISCUSSION
This study was conducted to compare root resorption of the maxillary central incisors following nonextraction orthodontic therapy with and without alveolar Cort surgery. In the present study, the permanent maxillary central incisor was selected because this tooth group is one of the most commonly resorbed groups during orthodontic treatment.[20,33,34] Moreover, the maxillary central incisor typically has formed roots completely by the start of fixed, orthodontic treatment.
The amount of root resorption was measured by subtracting each tooth length measurement at T2 from the corresponding measurement at T1. Mirabella and Artun[22] suggested this technique for calculating the amount of root resorption and consider it more valid when compared with the technique proposed by Linge and Linge,[13] in which T2 is adjusted by correcting for any change in the crown length from T1 to T2. Mirabella pointed out that with the Linge technique, the estimate for apical root resorption is reduced and a greater number of teeth showed root elongation. They suggested that a crown reduction will cause an overestimation of the root resorption when using their methods, but this overestimation will be considerably smaller than the corresponding amount of underestimation calculated with the Linge method. Results of the present study were similar to the previous investigations regarding random root elongation.[17-19,22,35,36] Because of overall errors in collecting data and methodology (e.g., tracing error, magnification, etc.,) a few maxillary central incisors demonstrated some elongation from T1 to T2 while most teeth showed resorption.
Because most of the radiographic records were obtained from the same radiographic facility in each group and were made using that same paralleling technique, errors as a result of variations in radiographic projection and enlargement are likely to be small and randomly distributed in the samples.
Mirabella and Artun[22] also suggested that the incisal edge and apex could be identified with a higher degree of accuracy than the cemento-enamel junction. These findings are in agreement with the results found by Sameshima and Sinclair.[18,19]
Results in relation to cephalometric study variables indicated that SNA was significantly larger (84.0° vs. 79.4°,P = 0.001) in the Conv sample representing a more prognathic position. Effects of therapy on study variable SNA was significant in the two nonextraction groups. SNA significantly decreased from 83.9° to 82.9° in Conv whereas SNA significantly increased in Cort from 79.4° to 80.0°. There was no significant difference in posttreatment SNA between the two groups (80.2° vs. 82.9°,P > 0.05); the increase in Cort SNA was logically due to the alveolar augmentation grafting.
Apical root resorption
Pretreatment (T1) root length homogeneity (P > 0.05) was demonstrated between Conv and Cort samples. Paired t-testing to analyze the differences between the right and left incisors also showed homogeneity, and for that reason, right and left central incisors were combined into a single group per sample for the purpose of statistical testing.
The effects of therapy were evaluated using paired t-testing which demonstrated significant root shortening within each of the two study groups, i.e. Cort -0.3 mm, P = 0.007 and Conv -0.7 mm, P = 0.001. This finding is consistent with previous studies on root resorption.[1-22,37] Mean root resorption within the Conv group in this investigation was 0.7 mm, a clinically acceptable amount, and consistent with the mean maxillary central incisor root resorption of 1.24 mm found by Sameshima and Sinclair.[18,19] Moreover, root resorption does not continue following orthodontic appliance removal.[13,21,37,38]
The 1.1 mm greater root resorption in Conv (25.7 mm) when compared with Cort (26.8) cannot be explained by differences in appliance therapy or force delivery, as both groups underwent similar orthodontic biomechanical therapy and arch wire changes; also the amount of maxillary central incisor movement in nonextraction therapy cannot explain the amount of root resorption. Multivariate ANOVA testing resulted in no significant association between the amount of root resorption and amount of change in any of the five cephalometric variables used to assess maxillary central incisor movement pre- to post-treatment.
The relationship between root resorption and RAP and the development of osteopenia is unclear in the Cort sample, but increased tissue turnover commensurate with RAP and diminished bone density would logically favor less root resorption. Iino reported no root resorption in the Cort group, but roots resorbed around the area of hyalinization in the control group.[39] Increased angiogenesis and tissue turnover in the Cort sample likely reduced the hyalinization;[40] hyalinization has been shown to correspond to the extent of root resorption.[41,42]
CONCLUSIONS
This study was conducted to compare root resorption of the maxillary central incisors following nonextraction orthodontic therapy with and without alveolar Cort surgery. The most important results of this investigation were as follows:
Root resorption was statistically greater (1.1 mm,P = 0.03) in Conv than in Cort
Statistically significant (P ≤ 0.007) root resorption was demonstrated in both study groups as a consequence of therapy; however, the amount of root resorption was not clinically significant, i.e., 0.3 and 0.7 mm
Point A, represented by the cephalometric measurement SNA, decreased significantly in Conv, but increased significantly in Cort because A-point was supplemented with alveolar graft augmentation
Cort treatment time was 2.7 times more rapid than Conv treatment time
Based on the conditions of this study, it may be concluded that Cort-facilitated nonextraction orthodontic therapy results in less root resorption and enhanced alveolar support within a significantly reduced clinical service delivery time frame. Rapid orthodontic treatment and reduced apical root resorption are probably due to the transient osteopenia induced by the Cort surgery and inspired by RAP.
Financial support and sponsorship
Nil.
Conflicts of interest
Drs. Wilcko and Wilcko hold a patent related to Accelerated Osteogenic Orthodontics and Periodontally Accelerated Osteogenic Orthodontics. Drs. Ferguson and Machado report no conflicts of interest related to this study.
References
- A preliminary report of an investigation of apical root resorption of vital permanent teeth. Int J Orthod. 1927;13:97-127.
- [Google Scholar]
- Root resorption after orthodontic treatment: Part 1. Literature review. Am J Orthod Dentofacial Orthop. 1993;103:62-6.
- [Google Scholar]
- Root resorption after orthodontic treatment: Part 2. Literature review. Am J Orthod Dentofacial Orthop. 1993;103:138-46.
- [Google Scholar]
- Root resorption and their relation to pathologic bone formation. Am J Orthod Oral Surg. 1942;28:513-26.
- [Google Scholar]
- Root resorption and tooth movement in orthodontically treated, calcium-deficient, and lactating rats. Am J Orthod. 1984;85:424-30.
- [Google Scholar]
- Effect of orthodontic force on periodontal tissue metabolism. A histologic and biochemical study in normal and hypocalcemic young rats. Am J Orthod Dentofacial Orthop. 1988;93:486-95.
- [Google Scholar]
- Faciolingual tooth movement: Its influence on the root and cortical plate. Am J Orthod. 1973;64:278-302.
- [Google Scholar]
- A comparative study in root resorption in permanent teeth. J Am Dent Assoc. 1936;23:822-6.
- [Google Scholar]
- A study of root resorption in treated class II, division I malocclusions. Angle Orthod. 1969;39:231-45.
- [Google Scholar]
- Pulp and dentine reactions to experimental tooth intrusion. A histologic study of the initial changes. Am J Orthod. 1970;57:370-85.
- [Google Scholar]
- A study of the relationship between incisor intrusion and root shortening. Am J Orthod Dentofacial Orthop. 1989;96:390-6.
- [Google Scholar]
- Patient characteristics and treatment variables associated with apical root resorption during orthodontic treatment. Am J Orthod Dentofacial Orthop. 1991;99:35-43.
- [Google Scholar]
- Evaluation of the risk of root resorption during orthodontic treatment: A study of upper incisors. Eur J Orthod. 1988;10:30-8.
- [Google Scholar]
- Root resorption during begg treatment; a longitudinal roentgenologic study. Am J Orthod. 1975;68:55-66.
- [Google Scholar]
- Apical root resorption in orthodontically treated adults. Am J Orthod Dentofacial Orthop. 1996;110:311-20.
- [Google Scholar]
- Facial and dentoalveolar structure and the prediction of apical root shortening. Am J Orthod Dentofacial Orthop. 1996;110:296-302.
- [Google Scholar]
- Predicting and preventing root resorption: Part I. Diagnostic factors. Am J Orthod Dentofacial Orthop. 2001;119:505-10.
- [Google Scholar]
- Predicting and preventing root resorption: Part II. Treatment factors. Am J Orthod Dentofacial Orthop. 2001;119:511-5.
- [Google Scholar]
- Postretention status of maxillary incisors with root-end resorption. Angle Orthod. 1973;43:247-55.
- [Google Scholar]
- Risk factors for apical root resorption of maxillary anterior teeth in adult orthodontic patients. Am J Orthod Dentofacial Orthop. 1995;108:48-55.
- [Google Scholar]
- Surgical operations on the alveolar ridge to correct occlusal abnormalities. Oral Surg. 1959;12:515-29.
- [Google Scholar]
- Corticotomy in orthodontics. In: Hosl E, Baldauf A, eds. Mechanical and Biological Basics in Orthodontic Therapy. Germany: Huthig Buch Verlag Heidelberg; 1991. p. :207-26.
- [Google Scholar]
- Rapid canine retraction through distraction of the periodontal ligament. Am J Orthod Dentofacial Orthop. 1998;114:372-82.
- [Google Scholar]
- The regional acceleratory phenomenon: A review. Henry Ford Hosp Med J. 1983;31:3-9.
- [Google Scholar]
- Rapid orthodontics with alveolar reshaping: Two case reports of decrowding. Int J Periodontics Restorative Dent. 2001;21:9-19.
- [Google Scholar]
- Rapid orthodontics following alveolar decortication: Why the resistance? J Parod d’Implant Orale. 2013;32:121-9.
- [Google Scholar]
- The Influence of Accelerated Osteogenic Response on Mandibular Crowding, Master’s Thesis. St. Louis University
- [Google Scholar]
- Dentoalveolar Bone Density Changes Following Accelerated Orthodontics. AADR/ IADR Meeting. Available from: https://www.iadr.confex.com/iadr/2002SanDiego/techprogram/abstract_19697.htm (accessed )
- Alveolar Bone Changes Following Accelerated Osteogenic Orthodontics, Master’s Thesis. St. Louis University.
- [Google Scholar]
- Possible etiologic factors in external root resorption. Am J Orthod. 1975;67:522-39.
- [Google Scholar]
- JCO/interviews Dr. Bjorn U. Zachrisson on iatrogenic damage in orthodontic treatment (part 1). Interview by Sidney Brandt. J Clin Orthod. 1978;12:102-13.
- [Google Scholar]
- Are dental anomalies risk factors for apical root resorption in orthodontic patients? Am J Orthod Dentofacial Orthop. 1999;116:187-95.
- [Google Scholar]
- Apical Root Resorption and the Maxillary Incisors, Master’s Thesis. St. Louis University;.
- [Google Scholar]
- Root resorption in maxillary central incisors following active orthodontic treatment. Am J Orthod. 1986;89:51-5.
- [Google Scholar]
- Long-term evaluation of root resorption occurring during orthodontic treatment. Am J Orthod Dentofacial Orthop. 1989;96:43-6.
- [Google Scholar]
- Acceleration of orthodontic tooth movement by alveolar corticotomy in the dog. Am J Orthod Dentofacial Orthop. 2007;131:448.e1-8.
- [Google Scholar]
- Surgically facilitated orthodontic treatment: A systematic review. Am J Orthod Dentofacial Orthop. 2014;145(4 Suppl):S51-64.
- [Google Scholar]
- Transition and determinants of orthodontic root resorption-repair sequence. Eur J Orthod. 1995;17:177-88.
- [Google Scholar]
- Hyalinization and root resorption during early orthodontic tooth movement in adolescents. Angle Orthod. 1998;68:161-5.
- [Google Scholar]






