Translate this page into:
Analysis and simulation of heat transfer in human tooth during the curing of orthodontic appliance and food ingestion
Address for Correspondence: J. Velázquez-López, Autonomous University of Puebla, Faculty of Stomatology; Stomatology Master of Science in Orthodontics, Graduate Building, Orthodontics Clinic, 31 Pte St. Num. 1304 Volcanes Colony, ZIP Code 72410, Puebla, México. E-mail: jorgevellop @gmail.com
This article was originally published by Wolters Kluwer and was migrated to Scientific Scholar after the change of Publisher.
How to cite this article: Velazquez-Lopez J, Cruz-Gomez MA, Ruelas- Oronia MA, Dipp-Velazquez F, Dib-Kanan A, Mendez-Mancilla Z. Analysis and simulation of heat transfer in human tooth during the curing of orthodontic appliance and food ingestion. APOS Trends Orthod 2016;6:137-46.
Abstract
The aim of this study was to analyze and simulate the heat transfer in the human tooth undergoing fixed orthodontic appliances and food intake. An in vivo representative mathematic model of a layered thermographic profile was developed during the LED curing of Gemini bracket 0.022 in slot (conventional ligating system) and Transbond XT adhesive. The characterization of the layered thermic response allowed to identify if during the LED curing process, according to manufacturer’s specification (light curing unit, adhesive) can induce pulpar necrosis. The profile’s thermographic model was the simulation basis of many conditions such as food intake, due to in vivo metrology is affected by the impossibility of a correct apparatus position and the physiologic function of the oral cavity which is exposed to uncontrollable temperature changes. The metrology was carried out with a T-440 thermographic camera during LED curing bracket, using a LED curing light (Elipar S10) placed at 3 ± 1 mm for 5 s at each mesial and distal surface. The thermography outcomes were analyzed in the FLIR Tools Software, Microsoft Excel 2013 and SPSS 22. To adjust the mathematic model error, in vitro studies were performed on third molars for the purpose of realizing extreme exposition temperature condition tests caused by the LED curing unit without jeopardizing the human tooth vitality as would it be on in vivo experimentation. The bracket curing results according to manufacturer’s conditions reached 39°C in vivo temperatures and 47°C on in vitro tests, which does not jeopardize human tooth vitality as said by previous researches, although, an LED curing precise protocol established by the manufacturer’s LED curing light is sustained.
Keywords
Heat transfer
human tooth
LED curing bracket
LED curing unit
thermography
INTRODUCTION
Heat transfer in human tooth is a daily[1,2] and common dental clinic[3-6] phenomena. Along the modern odontology approaches, instruments with many energy sources have been used such as dental laser,[7,8] light curing units,[9-11] and high speed hand pieces[12,13] causing damage to the various layers of the human tooth (enamel, dentine, cement, and pulp) by conduction, convection, and thermic radiation[2,14-19] due to temperature changes. Daily and dental clinic heat transfer in human tooth temperatures ranges − 5–76.3°C.[2,20]
The human tooth is a layered hard complex tissue.[21] The enamel layer has a 96% mineralized composition; water and organic material complement the remaining 4%. Dentine is a mineralized connective tissue layer with a collagen protein organic matrix,[22,23] inorganic material comprising ~70%, organic material ~20%, and water ~10%. Dentinal tubules are directed from the pulp chamber to the outside cement or amelodentinal junction.[23] The pulp is a connective tissue containing varying diameter nerve fibers from 1 to 10 μm[24] and sensitive nerve endings in the dentinal tubules,[25] which penetrate about 100–150 μm within the tubules of the wall of the pulp chamber.[26] These pulp nerve endings have an important role in the perception of thermal stimuli.[27]
Heat transfer in the tooth is based on conduction and convection processes, such as dentinal fluid fluency[27] and pulpal blood flow.[28,29] Tooth thermic properties vary among each layer[30] and microstructure.[31] The dentinal fluid fluency heating (or cooling) may increase the heat transfer in the pulp. In addition, the dentinal fluid fluency increases when the pulpar temperatures overtake 42°C and decreases during cooling. [29] Blood perfusion may also act as an important pulpar thermo regulator,[32] functioning as a disseminator when brought under cooling.
The abrupt temperature changes may cause dental pain, by damaging tooth tissues,[17-19,33] restorative interface and tooth-bracket adhesion.[34,35]
Dental pulp is vulnerable when the temperature reached is above ~5.5°C, this produces an irreversible pulpar damage.[18,19] Nonetheless, pulpar cells may overcome such damage,[36,37] as the heat shock proteins synthesis is increased.[38] Previous research has shown that a 42°C stimuli decreases pulpar cell viability, whereas heat shock proteins help in recovery.[39]
EXPERIMENT DETAILS
Specimens
In vivo
In vivo analysis at the Faculty of Stomatology; Stomatology Master of Science in Orthodontics, Graduate Building, Orthodontics Clinic Autonomous University of Puebla, México was developed. 8 patients, 5 females (not ovulating) and 3 males integrated the study. Patients from age 18 to 26 (mean 22 ± 1.1), with no systemic issues, previous fixed orthodontic appliance, root canal treatment, or drug treatment; previous prophylaxis was performed, with full permanent dentition, low or medium crowding level, 70% of clinical crown shown, enamel integrity (no cavities, fluorosis, or hypoplasia), no impacted teeth and full root development (checked in cone-beam computed tomography [CBCT]), third molars absence, no trauma (asked in anamnesis) or related metal allergies (Au, Co, Ni, Cr, Co, Ti, Ag, Fe, Al, Mo) and patients who accepted treatment and informed consent.
In vitro
Three third molars for this test were used. The third molars were extracted from a 23 aged male patient which is part of the in vivo sample, the extractions were made 2 h prior the study implementation.
Test apparatus and used software
A thermographic camera (also called an infrared camera) is a device that forms an image using infrared radiation, similar to a common camera that forms an image using visible light. Instead of the 400–700 nm range of the visible light camera, infrared cameras operate in wavelengths as long as 14,000 nm (14 μm). Their use is called thermography. The used camera was a T-440. It graduates temperatures from 253.15 to 1473.15 K (−20–1200°C), has ×8 continuous zoom, shows a live graph of temperatures across a line on the image, has a frame rate of 60 Hz and a visual range 25° ×19°, a minimal focus range (manual or automatic) from 1.31 ft (0.4 m) and a field of view match where Digital Image Field of View adapts to the IR lens. Works on a spectral range 7.5–13 μm, has a built-in touch-screen 3.5 in color LCD and a standard 25° lens included. It has a video bright LED lamp for a better view of the objective.
A dental curing light is a piece of dental equipment that is used for polymerization of light cure resin-based composites. It can be used on several different dental materials that are curable by light. The light used falls under the visible blue light spectrum. This light is delivered over a range of wavelengths and varies for each type of device. The two main dental curing lights are the halogen and LED. The used lamp was an LED curing lamp S10; works on an operating voltage 100–127 V 50/60 Hz or 230 V 50/60 Hz, a Lithium-ion battery, charges in 1.5 h and functions up to 60 min (new, fully charged battery). An optically active light emission area 60–65 mm2 on an utilizable wavelength range from 430 to 480 nm. Light intensity 1200 mW/cm2 (independent of battery power level).
HD450 light meter is a device used to measure the amount of light. It utilizes a precision silicon photo diode and spectral response filter. It works at a wide range of 40,000 Fc or 400,000 Lux Peak mode (10 μS) captures the highest reading. Relative mode indicates a change in light levels. It has a large backlit LCD display with a 40-segment bar graph and includes a light sensor with a 3 ft (1 m) cable and protective cover.
Flir Tools (FLIR Systems, Wilsonville, Oregon, United States of America) is a software suite specifically designed to provide an easy way to update the thermographic camera and create inspection reports. The main used key is the CSV file format which allows transferring the 60 × 60 grid of database to a data sheet in Microsoft Excel 2013. Key features included permit applying filters when searching for images: As texts in images and text annotations. Other characteristics are layout, move, and resize measurement tools on any infrared image. This program also creates PDF image sheets, adds headers, footers, and logos to the image sheets, as well as it sorts function (by date, groups sorted b path and groups sorted by date).
GALILEOS Viewer (Galileos Viewer, Sirona Dental Systems GmbH, Bensheim, Germany) software provides an anatomically accurate, patient-specific movement of the maxilla and mandible within the 3D volume, offering an integrated 3D workflow for the diagnosis and treatment of craniomandibular dysfunctions. It has an imaging volume of 15.4 cm/0.154m (international unit), a spherical imaging volume 3D resolution: Isotropic voxel size 0.25/0.125 mm in which mean error is 0.01 mm.
SPSS statistics is a software package used for statistical analysis. Companion products in the same family are used for survey authoring and deployment (data collection), data mining (modeler), text analytics, and collaboration and deployment.
Microsoft Excel 2013 software used in data processing.
Methods
Informed consent
A total of 8 patients of which 5 were females and 3 were males integrated the study (patients who attended to the Faculty of Stomatology; Stomatology Master of Science in Orthodontics, Graduate Building, Orthodontics Clinic Autonomous University of Puebla, México). The use of the thermographic camera as a diagnosis method and an explanation of the study were presented to the patients acknowledging that there has been no report of known risk in-between the use of a thermographic camera. Informed consent under the official norm (Norma Oficial Mexicana NOM-012-SSA3-2012) that establishes investigation protocol implementation criteria pro-health in humans was presented to the patients, asking for approval for realizing the study. All patients treated accepted the treatment and experimentation protocol.
In vivo tests
64in vivo thermographies total to the 8 sample patients during brackets protocol cementation were taken. The thermographies were taken at room temperature (20 ± 2°C) in a 62 ± 3% relative humidity. Previous tooth conditioning (deproteinization, etching, and primer), the bracket was placed in the correct position in the tooth, and a 5 s curing time in mesial and distal face at 3 ± 1 mm (specified by manufacturer) was realized [Figure 1]. In the meantime, the curing process was measured with the T-440 thermographic camera placed next to the reflex shield lamp (approximately 0.45 ± 0.2 m distance, ×4 zoom) and one thermography for each light emission at 5 and 10 s was taken, the time was measured by the curing lamp automatic programmation function.

- Intraoral thermography curing a metallic bracket; (a) real representation (b) thermography
Sixty-four total thermographies equals 8 to each patient, 4 mesial and 4 distal. Sixteen thermographies were selected under next criteria: Right focus, clear sharpness at the interest zone, and representative of the curing zone. The 16 selected thermographies were analyzed in the software FLIR Tools to get the 60 × 60 temperature grids. To find only one significant thermography a second filter to the 16 selected thermographies was applied. A differential statistics analysis to the thermographic data was applied, as well as the largest sum of each of the columns and rows that forms the databases of each of the thermal images to identify which presented the maximum temperature at the intersection of lines and columns and smaller standard deviation; the objective was to identify central tendency measurements and a Student’s t-test using SPSS 22 software (SPSS 23, IBM’s Corporate Privacy Office, New York, USA). The selected thermography was analyzed in Microsoft Excel 2013 to design a significant mathematic model of the temperatures’ distribution in the row and column that registered the highest temperature.
In vitro tests
Using the same metrology conditions as in vivo tests, recordings to know the gradual increase temperature according to time were made. The 3 third molars from the in vitro samples were used for this test. The molars were extracted 2 h prior the performance of this study. The molars were disinfected by immersion in a 40 ml solution: 20 ml distillated water and 20 ml NaClO at 6%. Thirty minutes after immersion, the tooth was dried at room temperature for 30 min. To mount the tooth, a resin acrylic base was designed so that it would not alter the heat transfer metrology. The thermographic camera focused at 0.45 ± 0.2 m from the object (×4 zoom) and a tooth preheat was perform to reach oral temperature (36.2°C, checked by the thermographic camera) using the curing light beam, followed by a continuous curing mode (120 s). The light curing unit placement on in vitro tests was 1, 2, 3, 4 , and 5 mm as specified by the manufacturer.
Data obtaining and mathematic model
A total of 8 CBCTs (belonging to study sample) were acquired to obtain enamel and dentine thickness measurements. Using GALILEOS Viewer software, the measured teeth were 11, 12, 13, 14, 15, 16, 17 and 31, 32, 33, 34, 35, 36, 37 in each CBCT. Measurements in sagittal view were performed, placing the cutting beam in the most medial portion from mesial to distal of each tooth and an inclination according to the most incisal to apical distance as it can be seen in Figure 2.

- GALILEOS viewer tomographic view. (a) Correct cutting beam placing. (b) Observable cut
Seven measurements for enamel and seven for dentine were captured under similar measuring anterior teeth previously performed by Sindi[40] and measuring posterior teeth by Smith.[41] A perpendicular trace from the sharpest zone in the pulp chamber to de sharpest zone in the dentinoenamel junction was realized for dentine measuring and a perpendicular trace from the pulp chamber to de sharpest zone in the dentinoenamel junction and the sharpest zone of outer enamel was realized for enamel measuring. Seven measurements were obtained, three in vestibular surface: Incisal third (1/3), medium third (2/3) and gingival third (3/3); similarly for lingual or palatal surface: Incisal third, medium third and gingival third; and a parallel to pulp chamber measurement in the incisal zone of dentine and enamel in anterior teeth, and oclusal zone in posterior teeth [Figure 3].

- Measurement zones. (a) Enamel measurement anterior teeth. (b) Dentine measurement anterior teeth. (c) Enamel measurement posterior teeth. (d) Dentine measurement posterior teeth
A representative mathematic model of the human tooth’s thermographic profile was planned according to mathematic model previously proposed: Conduction by Fourier, convection by Newton and radiation by Laplace, using thermophysic material properties and tissue involved on the oral cavity, previously reported. The profile’s thermographic model was the simulation basis of many conditions such as food intake, due to in vivo metrology being affected by the impossibility of a correct apparatus position and the physiological function of the oral cavity which is exposed to uncontrollable temperature changes.
TEST CONDITIONS
In vivo tests
The descriptive statistics analysis performed in SPSS 22 software of the 57, 600 temperature lectures that formed the 16 study thermographies shown in Table 1.
| n | Range | Minimum °C | Maximum °C | Mean °C | SEM | σ |
|---|---|---|---|---|---|---|
| 57,600 | 13.2 | 25.8 | 39.0 | 34.1 | 0.01 | 2.4 |
SEM – Standard error of mean
To determine the difference between the groups of the anterior and posterior thermography, Student’s t-test for independent groups was applied. The test result was P = 0.74, therefore the differences are not statistically significant.
In Figure 4a, an overlap of study thermography and database is shown, captured in Microsoft Office Excel 2013, to identify and isolate the highest temperatures during light curing (white zone). In Figure 4b, the extraction of interest zone is represented by using FLIR Tools software. The maximum temperature was at 39°C.

- Study thermography. (a) Grid temperatures overlap of interest zone. (b) Interest zone cut of 60 × 60 grids
Figure 5a shows the database of the interest area isolation, which is also the thermography where the highest temperature was found (39°C), as of this temperature grid, a significant equation in horizontal and the vertical plane was obtained (highlighted in white).

- Study thermography during light curing brackets. (a) Interest zone (b) highest temperature row graphic and equation, (c) highest temperature column graphic and equation (d) polynomial and temperatures overlap
The highest sum of each column and row that form the database of each thermography was identified, so was the intersection point of highest temperature (39°C).
The temperature data line and column intersection were plotted in Microsoft Office Excel 2013 to obtain the thermographic profile. Thermographic profile equations were approximated by polynomial trend from first through sixth grade to the equation obtained from the vertical and horizontal plane.
After checking different polynomial equation logarithm degrees in base 10, natural and exponential, the sixth-grade polinomio de presented less error (0.01). Equation characterizations are representative to know the temperature distribution.
Blue lines in graphics represent the determined values from metrology and red lines represent the polynomial fit [Figure 5b-d].
In vitro tests
The highest recorded temperatures on in vitro tests didn’t reach values over 38 °C at 15 seconds during light curing of the tooth at any distance, however a tooth preheating was realized at 36 °C to a similar temperature in oral cavity, it should be noticed that the study didn’t reproduce all environmental factors in oral cavity (such as saliva, initial temperature, biofilm, breath, etc.). For ethical reasons a test applying the curing light beyond 30 seconds in a vital tooth can’t be done, therefore an in vitro 60 and 120 second light curing period is proposed and done to understand what could happen if a tooth is light cured for that amount of time and cause irreversible pulp damage as previous studies reported. Yet, maximum temperatures up to 47 °C were reached when the light curing time was increased to 120 seconds (light curing unit continuous mode) as it can be seen in Figure 6, when the curing time is increased as the distance.

-
In vitro thermography test. (a) Reached temperature at 60 sexposition 1 mm distance. (b) Reached temperature at 120 s exposition 1 mm distance. (c) Reached temperature at 60 s exposition 2 mm distance. (d) Reached temperature at 120 s exposition 2 mm distance. (e) Reached temperature at 60 s exposition 3 mm distance. (f) Reached temperature at 120 s exposition 3 mm distance. (g) Reached temperature at 60 s exposition 4 mm distance. (h) Reached temperature at 120 s exposition 4 mm distance. (i) Reached temperature at 60 s exposition 5 mm distance. (j) Reached temperature at 120 s exposition 5 mm distance
Parameters and mathematic model
Average results in mm for each measured layer and zone are shown in Tables 2-5.
| Third/tooth | 11 | 12 | 13 | 14 | 15 | 16 | 17 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | |
| Incisal-oclusal | 1.49 | 2.48 | 2.16 | 2.54 | 1.63 | 3.16 | 1.40 | 2.32 | 1.69 | 2.73 | 1.65 | 3.32 | 6.28 | 2.76 |
| 1/3 | 1.04 | 1.36 | 1.15 | 1.15 | 1.46 | 1.73 | 1.80 | 2.18 | 1.78 | 3.28 | 1.94 | 5.86 | 1.77 | 5.78 |
| 2/3 | 0.96 | 1.82 | 0.93 | 1.40 | 1.27 | 1.78 | 1.7 | 2.15 | 1.52 | 2.19 | 1.56 | 3.40 | 1.75 | 3.73 |
| 3/3 | 0.57 | 1.59 | 0.74 | 1.54 | 0.72 | 2.34 | 0.85 | 2.10 | 0.84 | 2.15 | 0.79 | 2.74 | 0.70 | 4.02 |
| Third/tooth | 11 | 12 | 13 | 14 | 15 | 16 | 17 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | |
| 1/3 | 0.72 | 1.50 | 0.92 | 0.99 | 1.26 | 1.68 | 1.77 | 3.45 | 1.76 | 4.78 | 2.13 | 6.84 | 2.33 | 5.26 |
| 2/3 | 0.59 | 2.19 | 0.67 | 1.51 | 1.08 | 2.12 | 1.34 | 3.07 | 1.24 | 3.10 | 1.66 | 4.27 | 1.7 | 1.97 |
| 3/3 | 0.34 | 1.89 | 0.55 | 2.21 | 0.75 | 2.65 | 0.82 | 2.34 | 0.88 | 2.53 | 0.69 | 3.15 | 0.93 | 2.01 |
| Third/tooth | 31 | 32 | 33 | 34 | 35 | 36 | 37 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | |
| I/O | 1.95 | 1.74 | 1.43 | 2.65 | 1.38 | 2.98 | 1.31 | 2.63 | 1.92 | 2.53 | 1.56 | 2.78 | 1.82 | 2.96 |
| 1/3 | 1.07 | 0.65 | 0.95 | 0.95 | 1.22 | 1.49 | 1.51 | 1.72 | 1.79 | 2.92 | 1.64 | 3.93 | 1.79 | 6.65 |
| 2/3 | 0.83 | 1.16 | 0.92 | 1.42 | 1.00 | 2.04 | 1.41 | 2.06 | 1.53 | 1.94 | 1.46 | 2.35 | 1.52 | 4.79 |
| 3/3 | 0.47 | 1.46 | 0.59 | 1.75 | 0.62 | 2.26 | 0.86 | 1.86 | 0.67 | 1.89 | 0.92 | 2.54 | 0.76 | 3.76 |
| Third/tooth | 31 | 32 | 33 | 34 | 35 | 36 | 37 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | Enamel | Dentine | |
| 1/3 | 0.85 | 0.68 | 0.70 | 0.80 | 0.75 | 1.65 | 1.11 | 2.35 | 2.35 | 3.54 | 1.44 | 4.45 | 1.73 | 5.39 |
| 2/3 | 0.57 | 1.44 | 0.53 | 1.70 | 0.57 | 2.09 | 1.19 | 2.57 | 1.05 | 2.57 | 1.08 | 2.51 | 1.52 | 4.25 |
| 3/3 | 0.55 | 1.79 | 0.57 | 1.98 | 0.53 | 2.43 | 0.73 | 1.96 | 0.70 | 1.79 | 0.84 | 2.10 | 0.82 | 1.67 |
With a light meter (HD450), the light curing unit Elipar S10 used for the study was checked so the light intensity at an average distance of 3 ± 1 mm was 1200 mW/cm2 and had an active light emission range of 60–65 mm2 specified by the manufacturer (5 LEDs illuminated = 100% intensity).
Using the mathematical model designed, thermographic profiles were plotted to determine the temperature in each of the layers of the tooth. Based on the Fourier conduction law [Equation 1] and Newton convection law [Equation 2] and thermic resistance law [Equation 3], a mix of these models and their application by layers provides the following mathematical model [Equation 4]. The constants references are shown in Table 6.





| T1=Temperature 1 | A=Transfer area | L=Longitude |
|---|---|---|
| T2=Temperature 2 | Δx=Layer thickness | h=Convection constant |
| Φ=Thermic flow | K=Thermal conductivity constant | dQ/ dt=Differential temperature and time |
 =Differential thermic resistance per K =Differential thermic resistance per K |
 =Differential temperature initial layer =Differential temperature initial layer |
The mathematical model was analyzed in a Microsoft Excel 2013 data sheet. The temperature in each of the layers introduced into the model was calculated. It is noteworthy that this model can be added the number of layers required for any study. This model took into account the layers presented when cementing a bracket (metal, resin, enamel, and dentin).
Using the mathematical model and the thermophysic properties of the materials involved [Table 7], the temperature that exists in each of the layers of the tooth and heat loss existing between each were calculated.
| Characteristic Material | Value | Thickness (mm) | |
|---|---|---|---|
| Thermic | Enamel | 0.92α[42] | 0.962† |
| conductivity | Dentine | 0.56α[43] | 1.824† |
| (W/m/k)* | Adhesive | 1.9‡ | 0.83[44] |
| Stainless steel AISI 17-4¥ | 17.9∫ | 0.82≈ | |
After tooth conditioning, the layers included were steel, adhesive, enamel, dentine and pulp. Table 8 shows the layers temperature in wich temperature 1 (T1) equals the highest in vivo temperature registered in the termographic camera and temperature 2 (T2) equals the pulp temperature when physiological balance is stated (36.2°).
| Surface | Steel | Enamel | Dentine | Pulp | Final |
|---|---|---|---|---|---|
| 39 | 38.98 | 38.66 | 37.67 | 36.68 | 36.2 |
The thermographic profile showed in Graph 1, presents the heat loss in each layer and how thermal diffusivity of each material decreases initial temperature to avoid irreversible pulp damage.
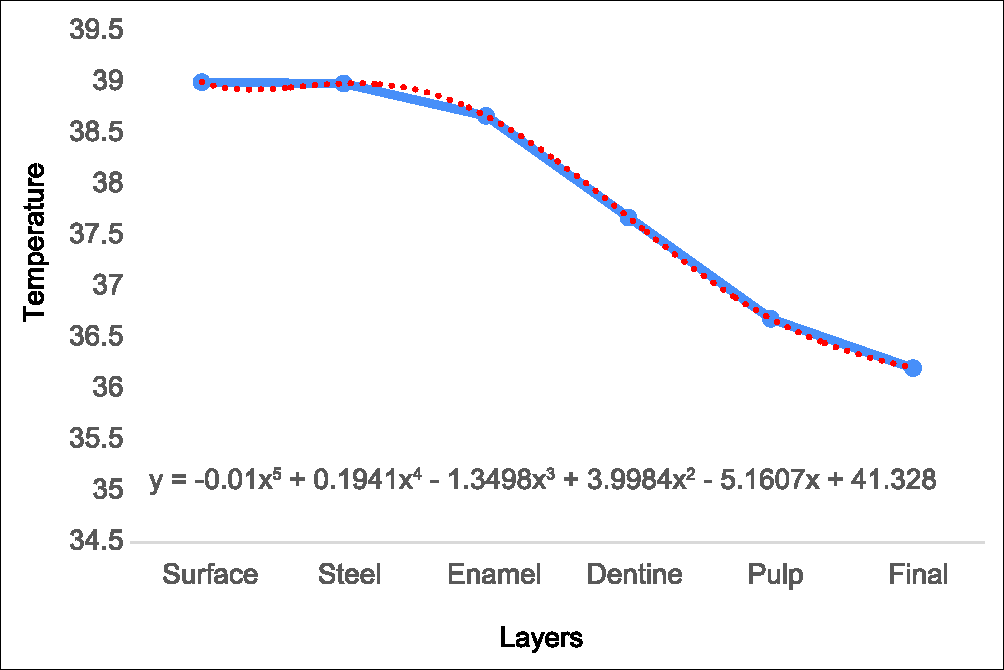
- Thermographic profile curing light application at 39°C
Thus, modifying the mathematic model it is possible to know the irradiated temperature to bone, noticing all the layers energy goes through.
A thermographic profile simulation was done during hot beverage intake at 76.2 °C, see Graph 2. Notice that the temperature the pulp receives is 43.1 °C see Table 9.
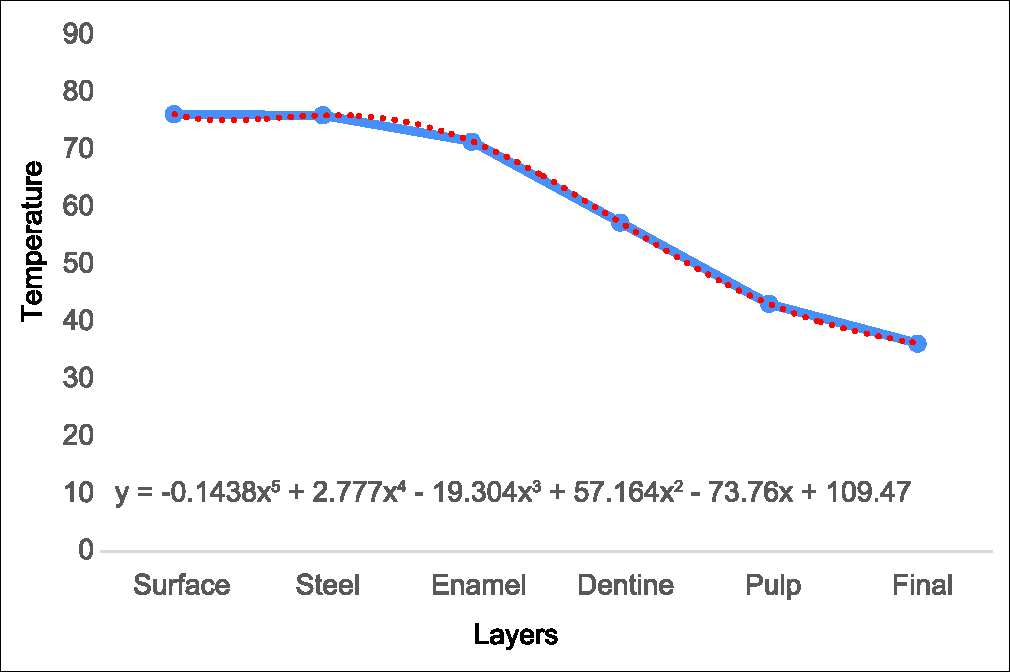
- Thermographic profile intake hot beverage at 76.2°C
| Surface | Steel | Enamel | Dentine | Pulp | Final |
|---|---|---|---|---|---|
| 76.20 | 76.00 | 71.45 | 57.27 | 43.10 | 36.2 |
A thermographic profile simulation was also done during cold food intake at -5 °C, see Graph 3. As the Laplace heat loss radiation theory mentions, the higher temperature of the inner layers is transferred to the layers with lower temperature, thus, when a food is ingested the temperature is rising to the inner layers as seen in Table 10.
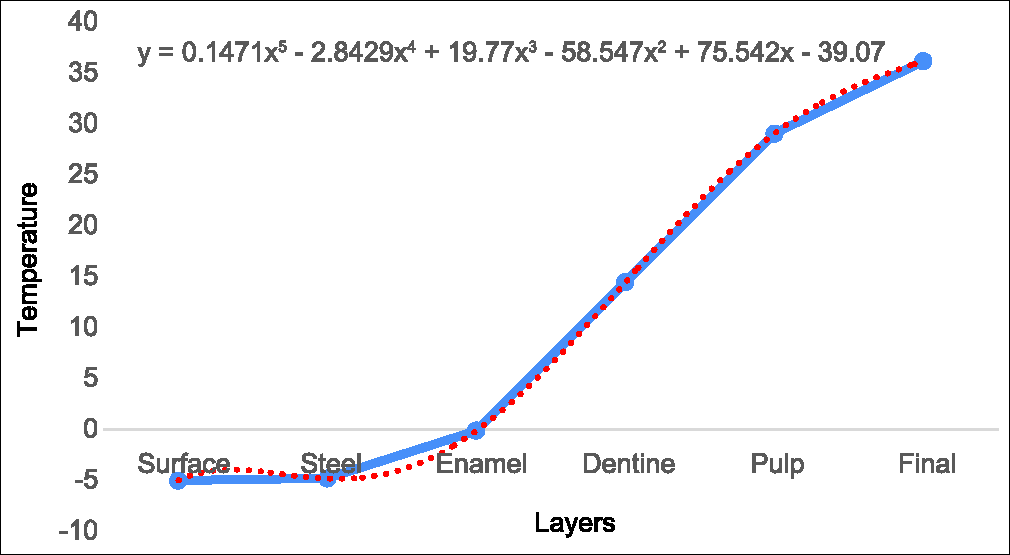
- Thermographic profile intake cold food at −5°C
| Surface | Steel | Enamel | Dentine | Pulp | Final |
|---|---|---|---|---|---|
| −5.00 | −4.79 | −0.10 | 14.48 | 29.08 | 36.2 |
DISCUSSION
Of all light curing units used in history the LED light has proofed being most effective in polymerization and the most reliable with dental pulp.[45]
It has been shown that the factors determining the temperature rise during curing of dental composites are higher photo polymerization power,[46-48] the light source, the type of curing unit, the quality of light filter, the output current and irradiation time[10,48] which we measured in several times in our study.
In this investigation, the distance from the emission of the LED light to the metal bracket, was determined by the interproximal contact of the dental organs (3 + 1 mm.) on in vivo test, and on in vitro test the distance from the emission of the LED light to the metal brackets was determined by the manufacturer; the exposure time of the LED curing light is controlled with the timer lamp; the temperature was measured with a thermographic camera.
Völkel et al., reported that, if the energy speed the pulp receives during light curing is higher than the energy it can dissipate, an irreversible damage will be produced.[47] and in 2006 T. Amano et al., proved that a 42 °C stimuli decreases pulp vitality, as the heat shock protein synthesis increases to help in pulp recovery.[39]
In this investigation, a mathematic model was proposed to calculate the heat transfer occurring at different temperatures: −5°C, 76.2°C and 39°C, as it would occur during food intake or dental procedures; but the model can be simulated with any temperature. In the model we considerate the layers when cementing a mental bracket (steel, adhesive, enamel, dentine, pulp), but it can adapt to any number of layers; and it can be done knowing the thermophysical properties of the material and the thickness of the layer, unique feature in our mathematic model compared with previous studies.
In the literature, no information about the heat transfer on in vivo practice was found using a thermographic cameras measuring tool. This is the first study in leaded to orthodontic practice using as a measuring tool a thermographic camera. Due to thermic safety is a prior consideration in clinic practice, there is a concern about tooth overheating in many odontology specialties, generating an important scientific input of a mathematic model that allowed the heat transfer simulation in human tooth.
The in vivo results give us a clear view that the used lamp can hardly cause pulp necrosis when the manufacturer’s instructions are followed, although, this does not guarantee that al LED curing light manufacturers count with previous detailed thermographic profile studies that their light unit has. However, we should be aware of the curing time when using continuous mode in the light curing unit, knowing that a 10 s exposure can produce a 3°C temperature increase, ergo, a 20 s exposure would produce a 6°C temperature increase and according to Pohto and Scheinin, Zach and Cohen[18,19] that increase can produce pulp necrosis.
The in vitro results comparison gives us an even clearer view that the used lamp in this study can cause a serious damage when a curing protocol is misused. Temperatures that range from 43°C to 47°C can cause pulp necrosis and even light burns in the soft tissue.
It has been reported that cold stimuli causes tooth pain, this may cause acute reversible pulpitis; however, there is no report that the cold causes pulp necrosis.
CONCLUSION
The mathematic model that simulates the thermographic’s profile of the tooth was based on the gotten results by in vivo and in vitro light curing concerning the mean layers thickness that allow us to get the thermographic characterization and could be used to widely simulate many conditions such as food intake and others with a standard error <5%
More studies doing standardization about thickness of layers of the human tooth are needed, taking account factors as: Material isotropy, age, sex, race, habits, etc., of the patient; thus, it can be offered an individual mathematic model and know the specific patient susceptibility.
The light curing protocol as the manufacturers say, did not cause permanent pulpar damage.
The cold (−5°C) or hot food intake (76.3°C) causes thermic stimuli on the tooth in an immediate way, but a physiological reflex of the oral cavity can thermoregulate by physiological fluids and conduction and convection avoiding pulpar damage. When this reflex is affected permanent pulpar damage is assured.
Acknowledgments
We are grateful for the unconditional support of the Autonomous University of Puebla: Faculty of Stomatology; Stomatology Master of Science in Orthodontics, Graduate Building, Orthodontics Clinic, to the Faculty of Engineering; I.M.E. School, Graduate Building, to the academic brigade 189 disasters prevention and sustainable development and to the Mexican Association of Orthodontics.
Likewise we thank , Tribology and Transport Group from the Faculty of Engineering whose members are I.M.E. J. Zilch-Hernandez, J. S. Martínez-Martínez, A. Morales- Herrera, R- Otero-Ahuacatitla.
Special thanks to graduate in Modern Language M. Cervantes Labastida of the Autonomous University of Puebla and to the President of the Asian Pacific Orthodonthic Society Nikhilesh Vaid for the ease in this publication.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Thermal environment of teeth during open-mouth respiration. J Dent Res. 1972;51:75-8.
- [Google Scholar]
- Thermal analysis of teeth irradiated with Er, Cr YSGG at low fluences. Laser Phys Lett. 2007;4:827-34.
- [Google Scholar]
- Influence of heat from light curing units and dental composite polymerization on cells in vitro. J Dent. 2006;34:298-306.
- [Google Scholar]
- Increases in intrapulpal temperature during polymerization of composite resin. J Prosthet Dent. 2006;96:328-31.
- [Google Scholar]
- Ultrasonic versus high-speed cavity preparation: Analysis of increases in pulpal temperature and time to complete preparation. J Prosthet Dent. 2008;100:107-9.
- [Google Scholar]
- Precise dental ablation using ultra-short-pulsed 1552 nm laser. Int J Heat Mass Transf. 2008;51:5732-9.
- [Google Scholar]
- Lasers in prosthodontics: Clinical realities of a dental laser in a prosthodontic practice. Alpha Omegan. 2008;101:188-94.
- [Google Scholar]
- Polymerization and light-induced heat of dental composites cured with LED and halogen technology. Biomaterials. 2003;24:1809-20.
- [Google Scholar]
- In-vitro pulp chamber temperature rise during composite resin polymerization with various light-curing sources. Dent Mater. 1999;15:275-81.
- [Google Scholar]
- Thermal risks from LED- and high-intensity QTH-curing units during polymerization of dental resins. J Biomed Mater Res B Appl Biomater. 2005;72:260-7.
- [Google Scholar]
- High-speed cavity preparation techniques with different water flows. J Prosthet Dent. 2002;87:158-61.
- [Google Scholar]
- Pulpal temperature increases with Er: YAG laser and high-speed handpieces. J Prosthet Dent. 2003;90:447-51.
- [Google Scholar]
- Lasers in dentistry: New possibilities with advancing laser technology? Int Dent J. 1990;40:323-32.
- [Google Scholar]
- Surface and pulp chamber temperature rises during tooth bleaching using a diode laser: A study in vitro. Br Dent J. 2006;200:631-4.
- [Google Scholar]
- Microscopic observations on living dental pulp. II. The effect of thermal irritants on the circulation of the pulp in the lower rat incisor. Acta Odontol Scand. 1958;16:315-27.
- [Google Scholar]
- Pulp response to externally applied heat. Oral Surg Oral Med Oral Pathol. 1965;19:515-30.
- [Google Scholar]
- Investigation of thermal stresses in dental restoration by mathematical method. J Eur Ceram Soc. 2007;27:899-902.
- [Google Scholar]
- Ultrastructural patterns of human dentinal tubules, odontoblasts processes and nerve fibres. Tissue Cell. 2006;38:141-50.
- [Google Scholar]
- Ultrastructure of human dentine 40 years ago–progress and perspectives. Arch Oral Biol. 1999;44:979-84.
- [Google Scholar]
- An investigation of thermal stimulation in intact teeth. Arch Oral Biol. 2007;52:218-27.
- [Google Scholar]
- Temperature related changes in pulpal microcirculation. Proc Finn Dent Soc. 1992;88(Suppl 1):469-79.
- [Google Scholar]
- Experimental studies on the nature of property gradients in the human dentine. J Biomed Mater Res. 2000;51:650-9.
- [Google Scholar]
- Measurement of thermophysical properties of human dentin: Effect of open porosity. J Dent. 2008;36:588-94.
- [Google Scholar]
- Temperature-dependent changes in the microcirculation of the dental pulp. Dtsch Zahnarztl Z. 1989;44:496-7.
- [Google Scholar]
- The effect of thermocycling regimens on the nanoleakage of dentin bonding systems. Dent Mater. 2002;18:189-96.
- [Google Scholar]
- Thermo-debonding mechanisms in dentin bonding systems using finite element analysis. Biomaterials. 2001;22:113-23.
- [Google Scholar]
- The influence of simultaneous mechanical and thermal loads on the stress distribution in molars with amalgam restorations. J Mater Sci Mater Med. 2000;11:133-40.
- [Google Scholar]
- Evaluation of thermal cycling and mechanical loading on bond strength of a self-etching primer system to dentin. Dent Mater. 2002;18:269-75.
- [Google Scholar]
- Mathematical modeling of heat shock protein synthesis in response to temperature change. J Theor Biol. 2009;259:562-9.
- [Google Scholar]
- Modern human molar enamel thickness and enamel-dentine junction shape. Arch Oral Biol. 2006;51:974-95.
- [Google Scholar]
- In vivo reproducibility study of ultrasound for monitoring enamel thickness. Oral Maxillofac Radiol. 2014;118:126-34.
- [Google Scholar]
- Heat conduction in teeth and the effect of lining materials. J Dent Res. 1964;43:315-22.
- [Google Scholar]
- Thermal properties of human teeth and dental cements. Shika Zairyo Kikai. 1990;9:633-46.
- [Google Scholar]
- Determination of optimum adhesive thickness using varying degrees of force application with light-cured adhesive and its effect on the shear bond strength of orthodontic brackets: An in vitro study. Orthodontics (Chic). 2013;14:e40-9.
- [Google Scholar]
- Light-emitting diode (LED) polymerisation of dental composites: Flexural properties and polymerisation potential. Biomaterials. 2000;21:1379-85.
- [Google Scholar]
- Effect of light guide tip diameter of LED-light curing unit on polymerization of light-cured composites. Dent Mater. 2005;21:217-23.
- [Google Scholar]
- Pulp response to externally applied heat. Oral Surg Oral Med Oral Pathol Oral Radiol. 1965;19:515-30.
- [Google Scholar]
- Effect of composite temperature on in vitro intrapulpal temperature rise. Dent Mater. 2007;23:1283-8.
- [Google Scholar]






