Translate this page into:
Diagnostic assessment of skeletal maturity through dental maturation in Hispanic growing individuals
Address for Correspondence: Dr. Rodrigo W. Oyonarte, Universidad de Los Andes, Facultad de Odontología, Monseñor Álvaro del Portillo 12.455, Las Condes, Santiago, Chile. E-mail: royonarte@miuandes.cl
This article was originally published by Wolters Kluwer and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Background
The aim of this study was to explore dental maturation as a diagnostic test for skeletal maturation.
Materials and Methods
Six hundred and fifty-seven growing individuals were classified according to their cervical vertebral maturity and dental maturity, both determined in lateral cephalograms and panoramic radiographs, respectively. The correlation between cervical and dental stages was established for each gender. A receiver operating characteristic curve analysis was made, and sensitivity and specificity values were established.
Results
Correlation was found between cervical and dental maturation for females (r = 0.73; P < 0.001) and males (r = 0.60; P < 0.001). Sensitivity for dental Stage F, as an indicator of a postmaturation peak stage, was 87.21% for females and 97.1% for males, whereas specificity for the same stage was 82.92% and 72.3% for females and males, respectively.
Conclusions
Dental maturation evaluation could contribute determining whether a patient is in a pre- or post-growth spurt stage.
Keywords
Cervical vertebrae
dental maturation
diagnostic test
growing individuals
skeletal maturation
INTRODUCTION
The assessment of skeletal maturation is a relevant factor in treatment planning for several orthodontic and orthopedic intervention modalities.[1,2] Despite it has been proven that chronological age has a high correlation with skeletal maturity when measured on the average patient, this indicator is not accurate for the whole population since body mass index, ethnic and metabolic factors may predispose an early or late skeletal development. Hence, it is necessary to manage other indicators for a precise determination of the growth spurt.[3-7]
One of the most common ways of determining the skeletal maturation is the hand and wrist ossification method.[1] A drawback of this technique is that patients need to be exposed to additional radiation,[8,9] so to avoid this exposure, some authors have proposed to assess skeletal maturation using dental and osseous structures, such as the cervical vertebrae, which are available on routine orthodontic radiographs.[10-12]
Another method for skeletal maturation determination is through the study of dental maturation. Demirjian et al. method, first described in 1973, has been widely used for this purpose given its simplicity and ease of use.[13-15] As well, different authors have modified it to increase its clinical efficiency, obtaining equivalent results regarding its ability to determine skeletal maturation.[16-20] On the other hand, cervical vertebral maturation assessment has become an accepted alternative diagnostic method to hand–wrist analysis for the determination of skeletal maturation, allowing a reduction of radiation exposure since this method is applied using lateral cephalometric radiographs.[10,21-23] Skeletal and dental maturation indices have been found to be correlated. One of the strongest correlations between dental and cervical maturation has been found with the left mandibular second molar as assessed on the panoramic X-ray.[24-28] Besides, If an orthodontic/orthopedic population of growing children is to be evaluated, the observation of this tooth seems appropriate due to its long formation time span and calcification chronology.
One key aspect of establishing a diagnostic test based on panoramic films is that this radiographic examination is broadly ordered by general practitioners during their routine patient examination. This means that general practitioners would have the opportunity to assess skeletal maturation based on panoramic radiographs without asking for an additional X-ray and, consequently, allowing them timely referral of their patients to the orthodontist if deemed necessary.
Although high levels of correlation have been reported between dental and skeletal maturation,[12,16,17,29] this relationship has not been systematically analyzed in Hispano-Americans, an ethnically different population from those previously reported. This becomes a relevant issue, as dental development follows a differential timing among different ethnic groups.[29] Therefore, diagnostic performance data are missing regarding the relationship between dental and skeletal maturation in South American Hispanic population.
The present study aimed at exploring dental maturation assessed at the lower left second molar as a diagnostic test for skeletal maturation in a sample of growing individuals in Chile.
MATERIALS AND METHODS
Population
A collection of panoramic and lateral cephalometric radiographs from children aged 5–15 years old was used. Both radiographs were acquired the same day, between June 2011 and July 2012 at Universidad de Los Andes, located in San Bernardo, Metropolitan Region, Chile. Every patient’s legal guardian signed an informed consent allowing the use of his or her radiographs for research purposes. This study is in accordance with the Helsinki Declaration and had the approval of the Research Committee, Faculty of Odontology of the Universidad de Los Andes.
Selection criteria
Panoramic radiographs showing the left mandibular second molar and lateral cephalograms correctly showing the cervical vertebral bodies were included in the study. Patients lacking personal data (gender or date of birth), presenting syndromes or pathologies that affect dental eruption, and dental developmental anomalies affecting the teeth were not included in the study.
Acquisition
A trained operator obtained the panoramic and lateral cephalometric radiographs with an Orthophos XG5 (Sirona Dental Salzburg, Austria) X-ray machine. The exposition parameters for panoramic radiographs were 75 kV, 15 mA, and 14.1 s, while for lateral cephalograms were 73 kV, 15 mA, and 9.4 s. Both radiographic examinations were assessed using the SIDEXIS XG software (Sirona Dental, Salzburg, Austria).
Variables
Patients were classified by gender, dental, and cervical vertebral maturation stage. Dental maturation assessment was done using Demirjian et al. method published in 1973, applied to the left mandibular second molar,[13] which was classified in one of eight stages as described in Table 1.
| Stage | Meaning |
|---|---|
| A | Isolated occlusal calcifcation points |
| B | Fusion of calcifed points, outlined occlusal surface |
| C | Enamel formation is complete at the occlusal surface |
| D | Crown is completed down to the cementoenamel junction, beginning of root formation |
| E | Root length is less than the crown height, initial formation of the radicular furcation |
| F | Root length is equal to or greater than the crown height, furcation has developed enough to give the roots a more defned and distinct outline |
| G | Distal apex is still partially open |
| H | Distal apex is completely closed |
The cervical vertebral maturation was assessed using Baccetti et al. method published in 2005.[30] Patients were classified according to the shape of their C2, C3, and C4 vertebral bodies, as seen in lateral cephalograms, into one of the six cervical vertebral stages (CVSs) as described in Table 2.
| Stage | Meaning |
|---|---|
| CVS 1 | C2, C3, and C4 lower borders are flat. C3 and C4 are trapezoid in shape |
| CVS 2 | Concavity on the inferior border of C2 is present. C3 and C4 are still trapezoid in shape |
| CVS 3 | Both C2 and C3 have concavities on their inferior border. C3 and C4 are trapezoid or rectangular horizontal |
| CVS 4 | Inferior borders of C2, C3, and C4 have concavities. C3 and C4 are rectangular horizontal |
| CVS 5 | C3 or C4 are squared shaped, the other one is rectangular horizontal in shape |
| CVS 6 | C3 and/or C4 is rectangular vertical in shape |
CVS – Cervical vertebral stage
To evaluate dental maturation as an indicator of skeletal maturation, pre- and post-growth spurt phases were established. Stages CVS 1, 2, and 3 were defined as pregrowth spurt, whereas stages CVS 4, 5, and 6 were postgrowth spurt.
Radiographic stage assessment
Panoramic and lateral radiographs were reviewed by one previously calibrated researcher (AC). Intraobserver agreement was calculated using the kappa index from two cervical and dental maturation assessments of ten patients carried out 3 weeks apart.
Statistical analysis
The correlation between dental and cervical maturation was assessed by gender using the Spearman’s coefficient. For each gender, receiver operating characteristic (ROC) curves were made after logistic regression to determine predicted probability. Sensibility and specificity were calculated for best cutoff value, looking for the dental stage that better represented the change from pre- to post-pubertal growth spurt (probability cut-off). It was considered that a better sensibility was more useful, patient that will be under discussion later. The diagnostic value of this test was analyzed by calculating prevalence, positive predictive value (PPV) and negative predictive value (NPV), and positive and negative likelihood ratios. Statistical analysis was carried out with the Stata 11® software (StataCorp LP, Texas, USA).
RESULTS
Intraobserver agreement was calculated using the kappa statistic. For dental maturation, kappa value was 1.00, whereas for cervical vertebral maturation, kappa value was 0.94.
Six hundred and fifty-seven patients were included in the sample. Three hundred and twenty-six patients (49.62%) were female and 331 (50.38%) were male. 81.58% presented a prepubertal maturational stage (CVS 1–3). Descriptive data regarding the cervical maturational status of the sample are presented in Table 3.
| Female (%) | Male (%) | Total (%) | |
|---|---|---|---|
| CVS 1 | 98 | 108 | 206 |
| 14.92 | 16.44 | 31.36 | |
| CVS 2 | 78 | 110 | 188 |
| 11.87 | 16.74 | 28.61 | |
| CVS 3 | 64 | 78 | 142 |
| 9.74 | 11.87 | 21.61 | |
| CVS 4 | 54 | 29 | 83 |
| 8.22 | 4.41 | 12.63 | |
| CVS 5 | 27 | 6 | 33 |
| 4.11 | 0.91 | 5.02 | |
| CVS 6 | 5 | 0 | 5 |
| 0.76 | − | 0.76 | |
| Total | 326 | 331 | 100 |
CVS – Cervical vertebral stage
Spearman’s correlation (r) shows a statistically significant correlation for dental and cervical maturation for both genders, which is stronger in females (r = 0.7334, P < 0.001) than in males (r = 0.6, P < 0.001).
The area under the ROC curves, representing in this study the probability of correctly classifying a pair of individuals in pre- and post-pubertal stages of development, were assessed using stages CVS 1, 2, and 3 as pregrowth spurt and stages CVS 4, 5, and 6 as postgrowth spurt. Our results indicated an area under the ROC curve of 0.896 for females and 0.914 for males.
The analyses of cutoffs for sensitivity and specificity for each gender are seen in Figure 1. This test has a sensitivity of 87.21% and a specificity of 82.92% for women and a sensitivity of 97.1% and specificity of 72.3% for men. According to this values of specificity and sensitivity, the presence of dental Stage F represents, for both genders, the best cutoff point for assessing when the postpubertal growth spurt phase starts.
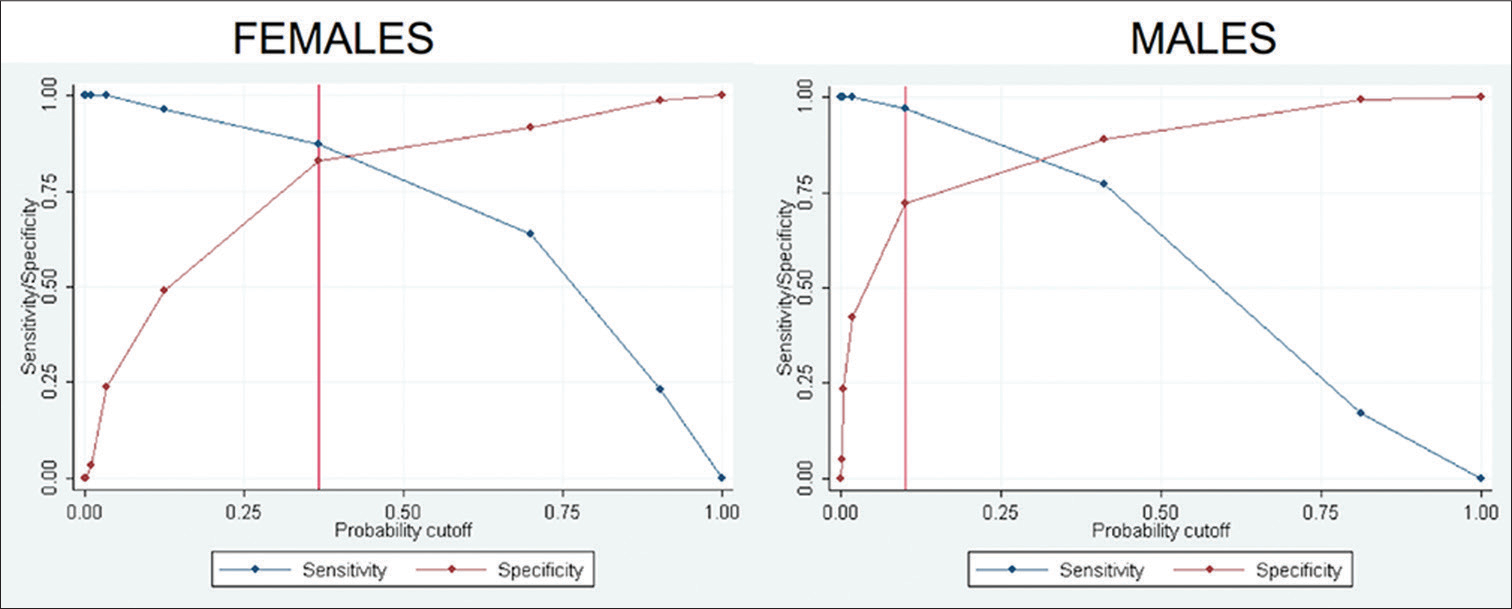
- Receiver operating characteristic curves showing probability cutoffs for females and males
Using the dental Stage F as the cutoff point, the PPV was found to be 94.8% for females and 99.5% for males. The assessment of this diagnostic test for each gender is summarized in Table 4. Positive likelihood ratios for females and males were 5 and 4, respectively, whereas negative likelihood ratios for females and males were 0.15 and 0.04, respectively.
| Results | Females (%) | Males (%) |
|---|---|---|
| Prevalence | 26 | 11 |
| Sensitivity | 87 | 97.10 |
| Specificity | 82.9 | 72.3 |
| PPV | 64.7 | 29.3 |
| NPV | 94.8 | 99.5 |
PPV – Positive predictive value; NPV – Negative predictive value
DISCUSSION
In this study, dental maturation assessment was analyzed as a diagnostic test of skeletal maturation. For that, the correlation between dental and cervical maturity was initially assessed. As expected, a significant positive correlation was obtained for both genders, which is consistent with correlations found in several other publications.[16,17,24,26,27,31-33]
The relevance of skeletal maturity in dentofacial orthopedic treatment planning is widely recognized. For example, it is clinically beneficial to identify if a Class II individual seeking orthodontic treatment is in a pregrowth spurt phase.[34] This is why the cutoff point was set favoring a good sensitivity over specificity, where the patients who are diagnosed as postgrowth spurt, are so indeed. This offers relevant information if dentofacial orthopedic procedures are to be carried out. The reported areas under the ROC curve indicate that this test is accurate for both females and males.[35]
In the present study, the best dental maturity indicator for the beginning of a postgrowth spurt phase was found to be Demirjian’s dental Stage F for both genders, as identified at the left second mandibular molar. This means that between dental Stages A and E, an individual would be in a pregrowth spurt phase and during Stages F through H, in a postgrowth spurt phase. In practice, once the left mandibular second molar has developed its furcation enough to show the radicular shape and the root length is equal or greater than the crown height, the patient has probably already surpassed the peak of pubertal growth speed.
According to our data [Table 4] regarding the assessment of this diagnostic test, the prevalence represents the probability of finding an individual aged 5–15 years old that already has gone through his or her growth spurt, being 11% and 26% for females and males, respectively. Sensitivity, which is here the ability to identify an individual in a postpubertal growth spurt stage when having a dental Stage F, G, or H is 87% for females and 97.1% for males. Specificity, the ability to identify that has not gone through pubertal growth spurt yet when having a dental Stage A–E, is 82.9% for females and 72.3% for males.
PPV is defined as the probability of being healthy when the diagnostic test gave a negative result.[36] In this study, it means that the chances of a patient not being in a postgrowth spurt yet while having a dental Stage A to E is high. This is relevant because knowing accurately when the patient has not gone through his or her growth spurt, improves dentofacial orthopedic treatment planning and performance.
Others studies about skeletal spurt assessment have stated that for positive likelihood ratios, a threshold equal to or >10 must be reached to establish that a diagnostic test is reliable.[29,37] Following this principle, our test would not be diagnostically reliable. Other authors,[38] however, propose that this is an arbitrary threshold and we should not ignore lower than ten likelihood ratios, especially when considering that the test we are studying is a screening tool proposed for helping general practitioners on their way for a timely referral to the orthodontist.
Although the use of dental maturity assessment-based Demirjian’s method for skeletal assessment has been questioned beyond the prepubertal phase,[29] our results suggest that this method is useful for identifying whether a patient has not gone through the growth spurt yet. This can enable the use of treatment strategies that benefit from the inclusion of this accelerated skeletal growth, as Class II dentofacial orthopedic interventions.[30] The evaluation of dental maturity stages in panoramic X-rays could expand the role of the dental practitioner in the context of the treatment of growing individuals, favoring the timely referral to the orthodontic specialist.
Although the present study shows that dental maturation evaluation is highly correlated with CVM, displaying good performance as a diagnostic test, these results may be cautiously interpreted as they were obtained from a cross-sectional sample of consecutively radiographed individuals. Certainly, the use of longitudinal records may improve the study model to allow a better understanding of dental maturation analysis relative to other skeletal maturation indicators.
CONCLUSIONS
Both the CVM and the Demirjian’s method for dental maturation may be applicable in practice. There is a strong correlation between dental and cervical maturation. Dental Stage F, measured in left mandibular second molar, can be used as a developmental indicator of the beginning of a postpubertal growth spurt phase which shows a good sensitivity and specificity. Dental maturation can be useful to determine whether the patient has started a postpubertal peak growth stage.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Treatment timing for twin-block therapy. Am J Orthod Dentofacial Orthop. 2000;118:159-70.
- [Google Scholar]
- Long-term effectiveness and treatment timing for bionator therapy. Angle Orthod. 2003;73:221-30.
- [Google Scholar]
- Interrelationships among measures of somatic, skeletal, dental, and sexual maturity. Am J Orthod. 1985;88:433-8.
- [CrossRef] [Google Scholar]
- Standard RUS skeletal maturation of Tokyo children. Ann Hum Biol. 1996;23:457-69.
- [CrossRef] [Google Scholar]
- Bone age: Assessment methods and clinical applications. Clin Pediatr Endocrinol. 2015;24:143-52.
- [CrossRef] [PubMed] [Google Scholar]
- Relationship between body mass index percentile and skeletal maturation and dental development in orthodontic patients. Am J Orthod Dentofacial Orthop. 2013;143:228-34.
- [CrossRef] [PubMed] [Google Scholar]
- Childhood obesity and skeletal-dental maturity. Eur J Paediatr Dent. 2012;13:128-32.
- [CrossRef] [Google Scholar]
- Skeletal stages of the hand and wrist as indicators of the pubertal growth spurt. Acta Odontol Scand. 1980;38:187-200.
- [CrossRef] [PubMed] [Google Scholar]
- The male adolescent facial growth spurt: Its prediction and relation to skeletal maturation. Angle Orthod. 1972;42:319-38.
- [Google Scholar]
- Skeletal age assessment utilizing cervical vertebrae. Am J Orthod. 1975;67:458-9.
- [CrossRef] [Google Scholar]
- An improved version of the cervical vertebral maturation (CVM) method for the assessment of mandibular growth. Angle Orthod. 2002;72:316-23.
- [Google Scholar]
- Mandibular growth changes and maturation of cervical vertebrae – A longitudinal cephalometric study. Angle Orthod. 1988;58:179-84.
- [Google Scholar]
- Reliability of the methods applied to assess age minority in living subjects around 18 years old. A survey on a Moroccan origin population. Forensic Sci Int. 2005;154:3-12.
- [Google Scholar]
- The A.B.F.O. study of third molar development and its use as an estimator of chronological age. J Forensic Sci. 1993;38:379-90.
- [Google Scholar]
- Dental and skeletal maturity – A biological indicator of chronologic age. J Clin Diagn Res. 2014;8:ZC60-4.
- [Google Scholar]
- Relationship between dental age according to Demirjian and cervical vertebrae maturity in Polish children. Eur J Orthod. 2011;33:75-83.
- [CrossRef] [PubMed] [Google Scholar]
- Dental age assessment of Southern Chinese using the United Kingdom Caucasian reference dataset. Forensic Sci Int. 2012;216:68-72.
- [CrossRef] [PubMed] [Google Scholar]
- Demirjian’s system for estimating the dental age of Northeastern Brazilian children. Forensic Sci Int. 2010;200:177.e1-4.
- [CrossRef] [PubMed] [Google Scholar]
- Assessment of dental maturity of Western Chinese children using Demirjian’s method. Forensic Sci Int. 2010;197:119.e1-4.
- [CrossRef] [PubMed] [Google Scholar]
- Skeletal maturation evaluation using cervical vertebrae. Am J Orthod Dentofacial Orthop. 1995;107:58-66.
- [CrossRef] [Google Scholar]
- A comparison of hand-wrist bone and cervical vertebral analyses in measuring skeletal maturation. Angle Orthod. 2006;76:984-9.
- [CrossRef] [PubMed] [Google Scholar]
- Validity of the assessment method of skeletal maturation by cervical vertebrae: A systematic review and meta-analysis. Dentomaxillofac Radiol. 2015;44:20140270.
- [CrossRef] [PubMed] [Google Scholar]
- Skeletal maturation evaluation using mandibular second molar calcification stages. Angle Orthod. 2012;82:501-6.
- [CrossRef] [PubMed] [Google Scholar]
- Relationship of dental and skeletal radiograph: Maturity indicator. Internet J Biol Anthropol. 2008;2:1-5.
- [Google Scholar]
- Relationships between dental calcification stages and skeletal maturity indicators in Thai individuals. Angle Orthod. 2002;72:155-66.
- [CrossRef] [Google Scholar]
- Relationships between dental and skeletal maturity in Turkish subjects. Angle Orthod. 2004;74:657-64.
- [Google Scholar]
- Cervical vertebral and dental maturity in Turkish subjects. Am J Orthod Dentofacial Orthop. 2007;131:447.e13-20.
- [Google Scholar]
- The diagnostic performance of dental maturity for identification of the circumpubertal growth phases: A meta-analysis. Prog Orthod. 2013;14:8.
- [Google Scholar]
- The cervical vertebral maturation (CVM) method for the assessment of optimal treatment timing in dentofacial orthopedics. Semin Orthod. 2005;11:119-29.
- [CrossRef] [Google Scholar]
- Correlation between dental maturity and cervical vertebral maturity. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010;110:777-83.
- [CrossRef] [PubMed] [Google Scholar]
- Correlation between cervical vertebral and dental maturity in Iranian subjects. J Calif Dent Assoc. 2011;39:891-6.
- [CrossRef] [Google Scholar]
- Correlation among chronologic age, skeletal maturity, and dental age. World J Orthod. 2010;11:e78-84.
- [Google Scholar]
- Mandibular changes produced by functional appliances in class II malocclusion: A systematic review. Am J Orthod Dentofacial Orthop. 2006;129:599.e1-12.
- [Google Scholar]
- Epidemiología Clínica (4th ed). Barcelona: Lippincott Williams & Wilkins; 2008.
- Dental maturation is not a reliable indicator of the pubertal growth spurt. Am J Orthod Dentofacial Orthop. 2016;150:4-6.
- [Google Scholar]






