Translate this page into:
Skeletal and Dentoalveolar Changes after Skeletal Anchorage-assisted Rapid Palatal Expansion in Young Adults: A Cone Beam Computed Tomography Study
Address for correspondence: Dr. N. R. Krishnaswamy, Department of Orthodontics, Tamilnadu, India. E-mail: ennarmd3@yahoo.com
This article was originally published by Wolters Kluwer and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Objective
The aim of this study was to evaluate skeletal and dentoalveolar changes before and after skeletal anchorage-assisted rapid palatal expansion in young adults by cone beam computed tomography.
Materials and Methods
This pilot study included ten patients with a mean age of 21.5 years with maxillary transverse deficiency treated with the skeletal expander. Three dimensional evaluation of the changes before and after expansion was evaluated with Cone Beam CT. Statistical analysis was performed using paired t-test.
Results
Skeletal expander produced an increase in maxillary transverse dimension at the skeletal, alveolar, and dental level. The maximum expansion was at the level of dentition, and the least amount of expansion was at the level of the frontonasal suture. There was also evidence of sutural divergence and buccal tipping.
Conclusion
The maxillary skeletal expander is an effective method for correction of maxillary transverse deficiency without surgery in adults.
Keywords
Adults
cone beam computed tomography
expansion
skeletal expander
Introduction
Maxillary transverse deficiency is a common orthodontic finding that is reported in 21% of children and 10% of adult population.[1] Rapid palatal expansion (RPE) is an effective orthodontic approach for widening the maxilla and correct the transverse discrepancy in children. By exerting a rapid transverse force on the maxillary dentition, the midpalatal suture is disrupted and separated, leading to greater cellular activity resulting in bone remodeling along the sutural areas.[2,3] In adults due to the maturation of the midpalatal sutures and resistance from the zygomatic buttress, the response to palatal expansion with RPE is less successful. The resulting widening of the maxillary width is more due to alveolar bone bending and dental tipping in adults.[4]
In addition to its inability to produce complete skeletal expansion in adults, the RPE can bring about unwanted side effects such as arch expansion failure, buccal crown tipping, alveolar bone dehiscence, root resorption, reduction in buccal bone thickness, and marginal bone loss.[5,6] Surgically assisted RPE (SARPE) is a treatment modality that helps to overcome the increased resistance from the bony plates and zygomatic buttress in adults.[7] However, SARPE has been reported to suffer from several limitations including but not limiting to surgical morbidity, high cost, and periodontal complications.[6,8] Recently, miniscrew-assisted RPE (MARPE) appliances that can localize the lateral forces to the midpalatal suture by using mini implants for anchorage have become available for treatment of maxillary constriction in adults.[9]
A bone-borne expander that is purely skeletally anchored and free of alveolar and dental side effects have been utilized to bring about pure skeletal expansion in adults.[10] Of interest is a particular study that compared a surgically assisted, bone anchored RPE and traditional tooth anchored RPE. It concluded that the bone anchored RPE produces more skeletal than dentoalveolar changes.[11] However, it has been reported in an another study that both expansions produce similar results.[12] Although bone-borne expanders are capable of producing greater skeletal expansion, there are concerns regarding its stability. The interlocked suture in mature patients undergoes significant torsion in three dimensions. As it splits the two halves of the maxilla twist away from each other, the implants used to anchor the RPE will experience additional strain and may tip. This will subsequently result either in loosening or breakage of the implant, thereby rendering the expansion device unstable.[13]
Wilmes et al. suggested the use of the term hybrid expander to any device that is used for expanding maxilla that is skeletally and dentally anchored.[14] These devices are reported to produce greater skeletal expansion ensuring minimal alveolar/dental tipping and at the same time offer greater stability. Maximization of the skeletal expansion through skeletal anchorage enhancement is by recruiting both palatal and nasal cortices. At the same time, a support wire connecting the expander to the I molars enhances the stability. This was a recent concept and such expanders are referred to as maxillary skeletal expander (MSE).[13] There are only a few reports on the skeletal and dentoalveolar changes, with this appliance.
The aim of this pilot study was to evaluate the short-term skeletal and dentoalveolar changes before and after MSE in young adults with maxillary transverse discrepancies. We hypothesized that the parameters do not differ significantly between pre- and postexpansion.
Materials and Methods
The sample for the prospective study was recruited from the patients who reported to the Department of Orthodontics at Ragas Dental College and Hospital. Ethical approval was obtained from the Institutional Review Board and informed written consent was obtained from all the participants. The sample consists of ten patients (5 boys, 5 girls) within the age group of 19–24 and with the mean age of 21.5 years.
The inclusion criteria were as follows: maxillary transverse deficiency, skeletal Class 1 malocclusion, no developmental deformity, no cleft lip and palate, no history of previous orthodontic treatment, and need for nonextraction orthodontic treatment. Pretreatment study models, photographs, and cone beam computed tomography (CBCT) were taken at the start of treatment and after completion of stabilization of maxillary expansion.
Appliance design
The expansion device which was used is MSE (BioMaterials, Korea). As per the manufacturer’s instruction, the screw size was selected based on the constriction of the palatal wall; appliance was fabricated by sizing the molar bands, taking a pick-up impression, and pouring it in stone. Placing the appliance 1–2 mm anterior to the junction of hard and soft palate, the lateral arms were contoured to the curvature of the palatal shelves and soldered to the molar bands. The central jack screw expander was flush against the palate and the supporting arm had 2 mm clearance to the lateral wall of palate.[15]
Four orthodontic mini screws (BioMaterials, Korea) measuring 1.8 mm × 11 mm were inserted into the palate using the Mini Handle Driver (BioMaterials, Korea). Care was taken to ensure that opposing screws were fitted first to prevent distortion or movement of the device and lifting up of the appliance on one side and the appliance was installed.
Maxillary expansion was initiated 2 days after insertion of the device. The appliance was then activated 2 turns per day until the required expansion was achieved. After achieving intended expansion, the expansion screw was blocked, and the appliance was left in place for 4 months [Figure 1], following which posttreatment CBCT, models, and photographs were taken.

- Skeletal expander. (a) Pre-expansion (b) Postexpansion
Measurements
Pre- and posttreatment CBCT images were obtained on a Kodak equipment (Model CS 9300, Carestream Health, Inc, Rochester, NY, USA) which was set at 8.0 mA and 70 kV and images were acquired for 6.15 s and with an axial slice thickness of 0.18 mm. During image acquisition, the patients were oriented to ensure that the Frankfort horizontal plane was parallel to the floor.
The Digital Imaging and Communications in Medicine images were imported, and cross-sectional slices were made with the help of Dolphin imaging software (version 11.5, Dolphin Imaging and Management Solution, Chatsworth, CA, USA). Three-dimensional image reconstructions were standardized using the Frankfort horizontal plane (represented by a line on the image) as the X-axis, the transporionic plane as the Y-axis, and the midsagittal plane as the Z-axis [Figure 2].
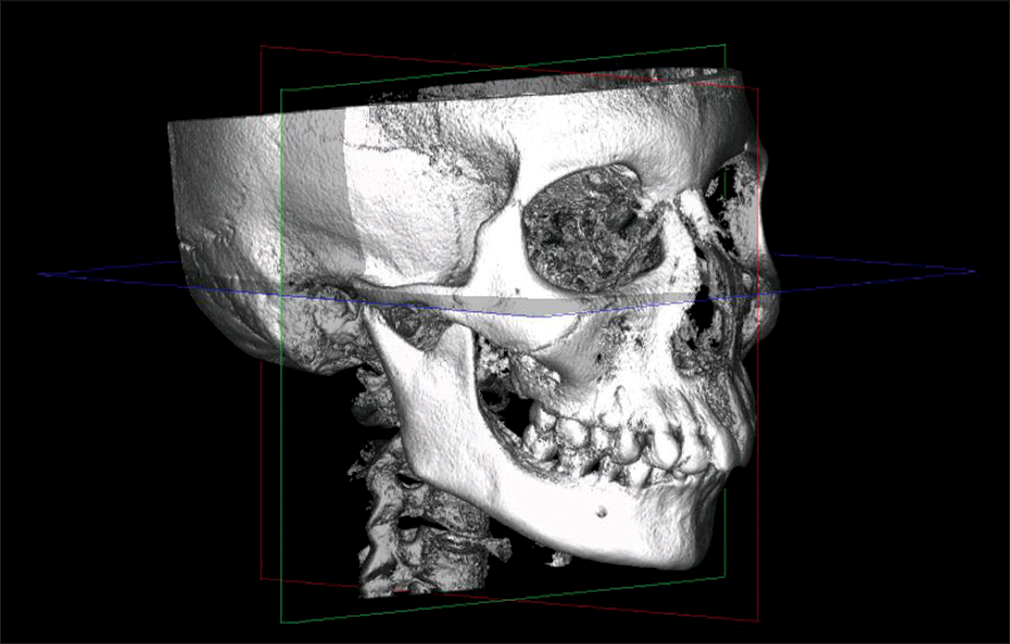
- Cone beam computed tomography image orientation
Transverse expansion was evaluated at the level of maxillary I molars, II premolars (PM), I PM, canines, and incisors on the coronal slice.
Transverse expansion at the sutural level was evaluated at the medial limits of left and right palatine process in the region of maxillary incisor (S1, S2), canine (S3, S4), I PM (S5, S6), II PM (S7, S8), and I molar (S9, S10).
Expansion at the alveolar level was evaluated from the most coronal medial limits of left and right alveolar process in the region of canine (AL1, AL2), I PM (AL3, AL4), II PM (AL5, AL6), and I molar (AL7, AL8).
Dental expansion was evaluated as the distance between the crown tips of I molars, II PM, I PM, and canines to calculate the intercanine width (ICW), inter-PM width (I and II IPMW), and intermolar width (IMW).
Tooth angulation was evaluated by calculating the angle between palatal root axis and the nasal floor at the region of canine (TOR1, TOL2), I PM (TOR3, TOL4), II PM (TOR5, TOL6), and I molar (TOR7, TOL8).
For evaluation of transverse cranial measurements, a posteroanterior view was reconstructed perpendicular to the midsagittal plane, and the bilateral landmarks of nasal cavity (N), zygoma (Z), and frontonasal (F) areas were identified in these images.
The landmarks evaluated in the study and their definition is summarized in Table 1.
| Landmarks | Description |
|---|---|
| S | Medial limits of the palatine process at left and right central incisors - S1, S2 canine (S3, S4), I premolars (S5, S6), II premolars (S7, S8), I molar (S9, S10) |
| AL | Medial limits of the alveolar process at left and right canine (AL1, AL2), I premolars (AL3, AL4), II premolars (AL5, AL6), and I molar (AL7, AL8) |
| IC | Medial points of palatal crown tip at canine |
| I PM | Medial points of palatal crown tip at I premolars |
| II PM | Medial points of palatal crown tip at II premolars |
| IM | Medial points of palatal crown tip at molar |
| TOL and TOR | Inclination between the palatal root axis and NF at left (TOL) and right (TOR) |
| Canine (TOR1, TOL2), I premolars (TOR3, TOL4), II premolars (TOR5, TOL6), and I molar (TOR7, TOL8) | |
| N | Lateral most border of nasal cavity |
| Z | Lateral most border of zygoma |
| F | Lateral most border of frontonasal level |
NF – Nasal floor; IC – Inter-canine
All transversal linear and angular measurements were recorded for each scan before insertion of expansion device (T1) and after stabilization (T2). One investigator performed the measurements. All points measured are depicted in Figures 3 and 4.
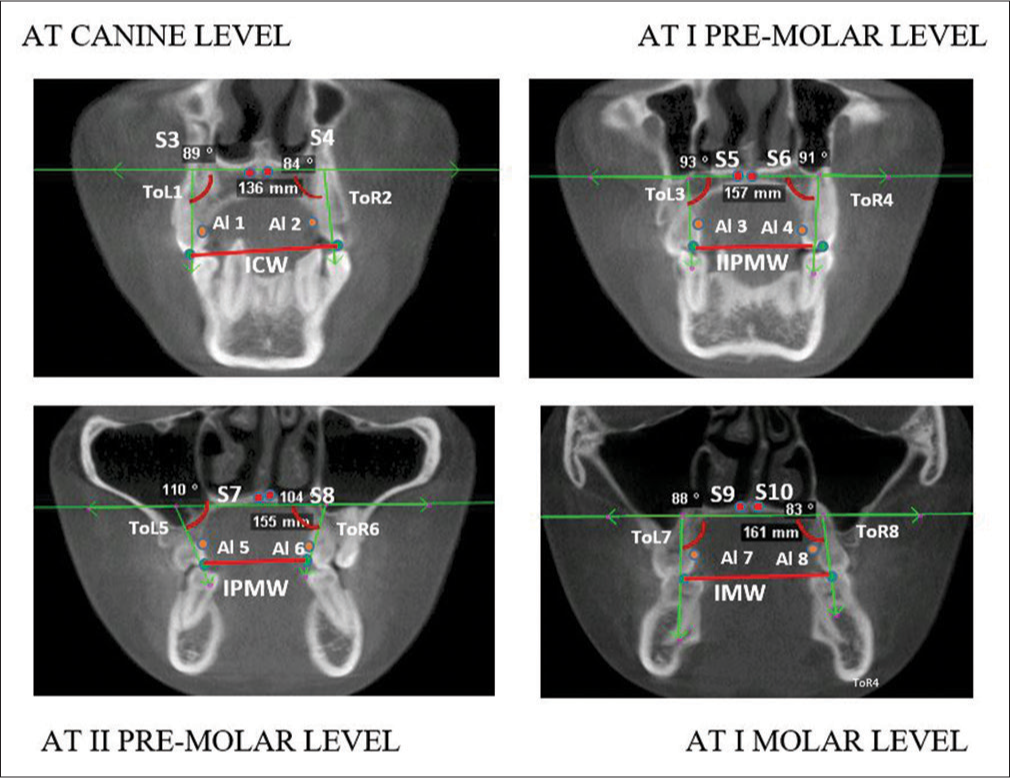
- Cone beam computed tomography coronal slice landmarks. S – Sutural level expansion at the medial limits of the palatine process; AL – Alveolar level expansion at coronal most medial limits of the alveolar process; TOR and TOL – Tooth inclination of palatal root to nasal floor (TOR: Right side, TOL: Left side); ICW – Inter canine width; I PMW – I Inter premolar width; II PMW – II Inter PM width; IMW – I Intermolar width
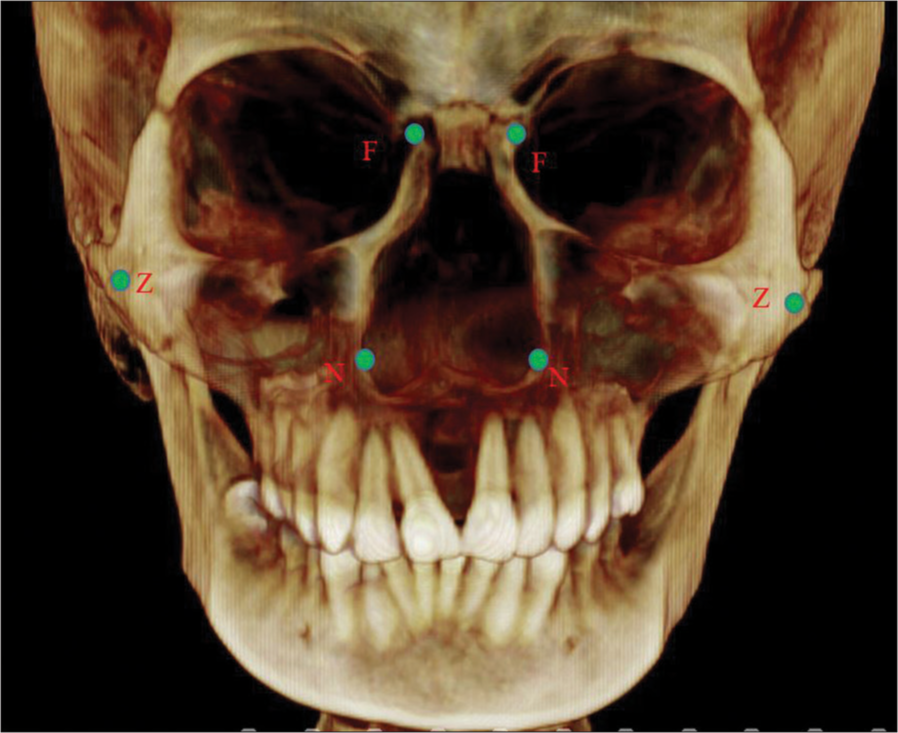
- Landmarks for nasal and cranial structures. Cone beam computed tomography at the nasal and cranial level landmarks. N – Lateral most border of nasal cavity; Z – Lateral most border of zygoma; F – Lateral most border at the frontonasal level
Suture angulation
Using the same software, a section running through the center of the maxillary palatal bone was selected, generating a slice in the horizontal plane to pass the middle of the palatal bone, allowing for the best visualization of the opening of the midpalatal suture.
This axial slice image was used to measure the relative parallelism between the left and right sides of the open palatal suture [Figure 5].
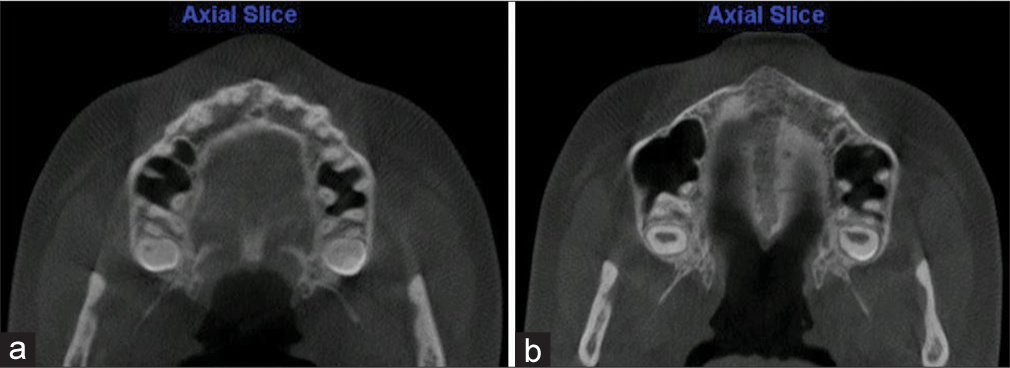
- Axial view showing suture opening before and after expansion. (a) Pre-expansion. (b) Postexpansion
A suture that demonstrated parallel opening (when the amount of expansion achieved in the anterior portion of the palatal suture was the same as the amount of expansion achieved in the posterior portion of the palatal suture) would have a 0° opening.
A suture that achieved more expansion in the anterior portion as compared to the posterior portion of the palatal suture would have a positive degree. The results for patients treated with the expander were then averaged to derive the degree of skeletal opening.
Statistics
All statistics were calculated using SPSS (SPSS, Inc., Chicago, IL) statistical software[16] for each parameter reference. To determine differences between the pre- and posttreatment for each parameter, paired-t-tests were used to calculate because of the small sample size.
The level of significance was defined as P < 0.05. In addition, each pre- and postexpansion parameter was compared to determine if any difference that existed before treatment and after treatment in addition to comparing the differences in treatment changes.
Of the total expansion, the skeletal, alveolar, and dental components were calculated and expressed as a percentage.
Results
The midpalatal suture was separated in all the patients, and the maxilla exhibited significant lateral movement [Tables 2-4].
| Parameter | Mean±SD | 95% CI of difference | P | Effect size | |||
|---|---|---|---|---|---|---|---|
| Sample-pre | Sample-post | Mean difference of sample (T2-T1) | Lower | Upper | |||
| Skeletal level | |||||||
| Suture opening at incisors | − | 5.3333 | 5.3333 | 3.663 | 6.137 | 0.001* | 2.83427 |
| Suture opening at canines | − | 4.833 | 4.833 | 3.76 | 5.44 | 0.000* | 3.918937 |
| Suture opening at I premolar | − | 4.5 | 4.5 | 3.621 | 4.979 | 0.000* | 4.532598 |
| Suture opening at II premolar | − | 4.5 | 4.5 | 3.621 | 4.979 | 0.000* | 4.532598 |
| Suture opening at molar | − | 4.5 | 4.5 | 3.621 | 4.979 | 0.000* | 4.532598 |
| Alveolar level | |||||||
| Alveolar level at canines | 20.5±1.04 | 26.5±1.41 | 6±1.04 | 4.621 | 5.979 | 0.000* | 5.586691 |
| Alveolar level at I premolar | 22.3±1.50 | 28.16±1.86 | 5.83±1.03 | 4.542 | 6.058 | 0.000* | 5.003068 |
| Alveolar level at II premolar | 26±2.68 | 32±2.28 | 6±0.8944 | 4.274 | 5.526 | 0.000* | 5.596194 |
| Alveolar level at molar | 30±1.788 | 36.5±1.378 | 6.5±1.51 | 5.495 | 7.305 | 0.001* | 5.059644 |
| Dental level | |||||||
| IC width | 22.66±1.21 | 28.5±2.42 | 5.83±1.32 | 3.76 | 5.44 | 0.000* | 3.918937 |
| Inter I premolar width | 24.66±1.861 | 30±3.01 | 5.33±1.72 | 3.474 | 5.526 | 0.043* | 3.138686 |
| Inter II premolar width | 28.83±2.31 | 34.5±2.07 | 5.66±1.36 | 3.56 | 5.24 | 0.000* | 3.748548 |
| Intermolar width | 33.66±2.06 | 41±3.40 | 7.33±1.96 | 5.694 | 8.306 | 0.004* | 3.834058 |
| Canine angulation left | 89.5±1.04 | 88.7±0.04 | −0.8±0.41 | − | − | 0.3409 | − |
| Canine angulation right | 89.66±0.516 | 88.94±0.064 | −0.72±0.21 | − | − | 0.4200 | − |
| I premolar angulation left | 90.16±0.4082 | 89.35±0.07 | −0.81±0.73 | − | − | 0.3010 | − |
| I premolar angulation right | 89.83±1.47 | 88.93±1.04 | −0.9±0.83 | − | − | 0.3335 | − |
| II premolar angulation left | 88±1.78 | 86.98±0.0314 | −1.015±0.65 | − | − | 0.4312 | − |
| II premolar angulation right | 88.16±3.81 | 87.25±0.0404 | −0.91±0.83 | − | − | 1.0000 | − |
| Molar angulation left | 80.83±2.48 | 75.83±1.161 | −5±1.09 | −5.539 | −4.06 | 0.039* | −4.64758 |
| Molar angulation right | 81.16±0.983 | 75.66±1.75 | −5.5±0.836 | −5.9 | −4.9 | 0.030* | −7.72305 |
*Statistically significant (<0.05). CI – Confidence interval; SD – Standard deviation; IC – Intercanine
| Parameter | Mean±SD | 95% CI of difference | P | Effect size | ||||
|---|---|---|---|---|---|---|---|---|
| Sample-pre | Sample-post | Mean difference of sample (T2-T1) | Lower | Upper | ||||
| Nasal and cranial level | ||||||||
| Nasal cavity | 22.66±2.50 | 26.83±2.63 | 4.166±0.7527 | 3.572 | 4.628 | 0.043* | 5.556574 | |
| Zygoma | 105.16±7.35 | 107.8±7.44 | 2.666±0.816 | 2.236 | 3.364 | 0.000* | 3.549648 | |
| Frontonasal level | 17.33±2.33 | 17.83±2.13 | 0.5±0.8366 | −0.203 | 1.003 | 0.1739 | 0.474342# | |
*Statistically significant (<0.05), #Statistically not significant. CI – Confidence interval; SD – Standard deviation
| Implant-assisted RME group (%) | |
|---|---|
| Skeletal expansion | 18.3 (61) |
| Alveolar expansion | 6 (20) |
| Dental expansion | 5.73 (19) |
| Total expansion | 30.03 (100) |
RME – Skeletal anchorage assisted rapid palatal expansion
Skeletal changes
The intersutural expansion at the median palatine level of the I molar, II PM, and I PM was on an average 4.5 mm, while at the canine, it was 4.8 mm, and at the incisors, it was 5.3 mm. All values were significant (P < 0.05). This reflects a nonparallel expansion of the midpalatal suture with the greatest widening at the incisor and least at the molar region.
Similarly, on the axial slice, the expansion produced a mean sutural divergence of 3.56° reiterating a nonparallel opening of the midpalatal suture [Table 5].
| n | Left | Right | P | Total mean |
|---|---|---|---|---|
| 10 | 2.41±1.72 | 2.03±1.52 | 0.3632 | 3.56 |
n – Number of patients
Alveolar changes
The expander produced a significant amount of alveolar bending (P < 0.05) as measured at the alveolar process from the canine to the molar.
Dental changes
Dental changes significant amount of expansion was seen in the IMW, Inter II PMW, Inter I PMW, and ICW (P < 0.05) with the greatest change in the width at the level of the molar. Buccal tipping of teeth was also observed with significant greater tipping of I molar compared to PM and canine (P < 0.05).
Since the expansion seen at the IM, II PM, I PM, and IC represents the combined expansion of skeletal, alveolar, and dental structures, the percentage of expansion of each of these areas was calculated and found to be as follows: skeletal 61%, alveolar 20%, and dental 19%.
The zygomatic arch, nasal cavity, and frontonasal area were widened by 4.16 ± 0.7527 mm, 2.6 ± 0.816 mm, and 0.5 ± 0.8366 mm, respectively. The amount of expansion decreased with superior position of anatomical structures, indicating a pyramidal pattern of maxillary expansion.
Discussion
The present pilot study was designed to evaluate the dentoalveolar and skeletal changes of a modified miniscrew-supported palatal expander in young adults using CBCT. The expander is designed in such a way that it delivers the expansion forces to 4 mini implants that are capable of anchoring the device to both nasal and oral cortical layer.[17-19] In addition, the maxillary I molars are used to stabilize the position of the expansion screws rather than for anchorage.[13] The appliance is positioned in the IM area so as to direct the lateral forces against pterygomaxillary buttress which offers resistance to expansion in adults.[20] The participants recruited for the present study were young adults in whom the midpalatal suture and the adjacent articulation would have matured, and same being confirmed as observed in pretreatment CBCT. The study has used CBCT to measure the parameters considered, as the versatility of the CBCT and imaging software[21-23] for identifying the dimensional changes has been reported.
To determine the difference between two time points for each parameter, a paired sample t-test was calculated because of the small sample size, and the level of significance was defined as P < 0.05. The paired sample t-test is considered robust to violations of normality as it is reported to have inbuilt mechanism to account for minor variation in normality distribution.[18]
Clinical translation of the result, as observed by the effect size [Table 2], indicates that the appliance produces a consistent, predictable result. The MSE effectively achieved dentoalveolar as well as skeletal expansion by separating the midpalatal suture in all the participants. The suture expansion was greater along the incisor region than in the molar region. This triangular pattern of sutural expansion is similar to that reported with RPE by Garrett et al.[19] However, the divergence from the posterior to the anterior of the suture in the present study was relatively less compared to those reported with RPE in literature. The reason for difference in degree of divergent opening of suture in the present sample could be due to the more posterior position of jack screw and the parallel placement of the four miniscrews that probably are more effective in overcoming the resistance offered by the zygomatic buttress. A similar but more parallel expansion of suture has been reported with the use of bone-borne expansion device.[21]
The skeletal gain in our sample accounts for 61% of total expansion and is higher than the 50% skeletal expansion that has been reported by Profitt and 40% by Kartalian et al.[24] and 55% reported by Garrett et al.[6] The greater percentage of skeletal expansion in our sample can be attributed to the better anchorage potential of the four miniscrews that are capable of bicortical engagement in this design.[23] Tausche et al.[7] using CT has documented that in their sample, 85%–91% of expansion achieved was skeletal in nature. However, in their participants, a surgical intervention was employed along with distraction unlike in our sample where no surgeries were performed.
The alveolar width increase was significant and contributed to nearly 20% of total expansion. This is similar to 22.2% expansion at cementoenamel junction, as reported with mini implant-assisted RPE (MARPE) by Mary.[25] Handlemen has reported that the quantum of alveolar expansion to be greater in adults than in adolescents and contribute to nearly 33% of total expansion when RPE was used in adults.[4]
The greatest changes following expansion were at the IM level; this reflects the combined skeletal and dentoalveolar expansion. Of the total IM increase of 7.33 ± 1.96 mm, the dental expansion at the level of the molar was found to be 2.83 ± 1.96 mm and accounted for 19% of total expansion. This increase in the IM width at dental level is relatively less when compared to other reports employing MARPE device. The most probable reason could be due to the nature of the design of the MSE, especially the bicortical engagement with the long implants offering greater skeletal anchorage.
Despite the fact that the appliance was skeletally anchored, there was evidence of buccal tipping of the PM and molars in a few cases. This is similar to prior reports employing MARPE and RPE.[12] The molars experienced great tipping than the PM and can be attributed to the inability of the stabilizing wire from transmitting expansion forces to the molars. The crown tipping can also be due to the play between the miniscrew and the insertion slot of miniscrew, as reported by Carlson et al.[15]
The skeletal expansion observed in the present study includes the possible expansion of the nasal cavity, zygomatic arch, and frontonasal area; this reflects a pyramidal pattern of expansion with the base at the nasal cavity and similar to expansion pattern reported by conventional RPE,[2,3] SARPE,[7] and MARPE.[26] The extent of the influence of this pyramidal expansion on the sutural expansion and the dentoalveolar width warrants further study.
Based on the present results and observations, the null hypothesis is rejected. The present pilot study identifies the effectiveness of the new MSE design for maxillary widening, even with small sample size. The extent of the effectiveness and difference in parameters considered, especially those relating to the width of the arch, at several positions as well as those that of dental tipping still remain relatively elusive. Studies using larger sample size perhaps would help to understand the complete dynamics of the expansion when employing MSE.
Conclusion
Within the limitations of this study, our results suggest the following: The skeletal expansion device can be an effective treatment modality for the correction of maxillary transverse deficiency in young adults through separation of the midpalatal suture. Expansion achieved with the appliance exhibits a pyramidal pattern. The degree of skeletal, alveolar, and dental expansion was 61%, 20%, and 19%, respectively. There was evidence of mild buccal tipping of the maxillary teeth. The expansion also caused widening of the nasal cavity, the zygomatic arch, and frontonasal area.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Epidemiology of posterior crossbite in the primary dentition. J Clin Pediatr Dent. 2007;32:73-8.
- [CrossRef] [PubMed] [Google Scholar]
- Gross reactions to the widening of the maxillary dental arch of the pig by splitting the hard palate. Am J Orthod. 1959;45:868.
- [Google Scholar]
- Palatal expansion: Just the beginning of dentofacial orthopedics. Am J Orthod. 1970;57:219-55.
- [CrossRef] [Google Scholar]
- Palatal expansion in adults: The nonsurgical approach. Am J Orthod Dentofacial Orthop. 2011;140:462. 464, 466
- [CrossRef] [PubMed] [Google Scholar]
- Periodontal effects of rapid maxillary expansion with tooth-tissue-borne and tooth-borne expanders: A computed tomography evaluation. Am J Orthod Dentofacial Orthop. 2006;129:749-58.
- [Google Scholar]
- Skeletal effects to the maxilla after rapid maxillary expansion assessed with cone-beam computed tomography. Am J Orthod Dentofacial Orthop. 2008;134:8-9.
- [Google Scholar]
- Three-dimensional evaluation of surgically assisted implant bone-borne rapid maxillary expansion: A pilot study. Am J Orthod Dentofacial Orthop. 2007;131(4):S92-9.
- [Google Scholar]
- Rapid maxillary expansion with palatal anchorage of the hyrax expansion screw – Pilot study with case presentation. J Orofac Orthop. 2004;65:419-24.
- [Google Scholar]
- Miniscrew-assisted nonsurgical palatal expansion before orthognathic surgery for a patient with severe mandibular prognathism. Am J Orthod Dentofacial Orthop. 2010;137:830-9.
- [Google Scholar]
- Transversal palatal expansion using a palatal distractor. J Orofac Orthop. 2003;64:443-9.
- [CrossRef] [PubMed] [Google Scholar]
- Meta-analysis of immediate changes with rapid maxillary expansion treatment. J Am Dent Assoc. 2006;137:44-53.
- [CrossRef] [PubMed] [Google Scholar]
- Tooth-borne vs. bone-borne rapid maxillary expanders in late adolescence. Angle Orthod. 2015;85:253-62.
- [CrossRef] [PubMed] [Google Scholar]
- Letter to editor, what are the limits of microimplant assisted palatal expander. Am J Orthod. 1959;45:868.
- [Google Scholar]
- Application and effectiveness of a mini-implant- and tooth-borne rapid palatal expansion device: The hybrid hyrax. World J Orthod. 2010;11:323-30.
- [Google Scholar]
- Microimplant-assisted rapid palatal expansion appliance to orthopedically correct transverse maxillary deficiency in an adult. Am J Orthod Dentofacial Orthop. 2016;149:716-28.
- [Google Scholar]
- Using SPSS to Understand Research and Data Analysis. Psychology Curricular Materials. Book 1. Available from: http://scholar.valpo.edu/psych_oer/1. Copyright © 2014 by Daniel Arkkelin. This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. [Last accessed on 2016 Jun 28]
- [Google Scholar]
- Miniscrew-assisted rapid palatal expander (MARPE): The quest for pure orthopedic movement. Dental Press J Orthod. 2016;21:17-23.
- [Google Scholar]
- Linear accuracy and reliability of cone beam CT derived 3-dimensional images constructed using an orthodontic volumetric rendering program. Angle Orthod. 2008;78:387-95.
- [CrossRef] [PubMed] [Google Scholar]
- Evaluation of the effects of rapid maxillary expansion in growing children using computer tomography scanning: A pilot study. Eur J Orthod. 2007;29:37-44.
- [CrossRef] [Google Scholar]
- Three-dimensional cone beam computerized tomography in dentistry. Dent Today. 2006;25:130. 132-5
- [Google Scholar]
- Non-surgical treatment of transverse deficiency in adults using Microimplant-assisted Rapid Palatal Expansion (MARPE) Dental Press J Orthod. 2017;22:110-25.
- [Google Scholar]
- Laerd Statistics. Paired-Sample t-Test using SPSS Statistics. Statistical Tutorials and Software Guidance. 2015. Available from: http://www.statistics.laerd.com. [Last accessed on 2017 may 10]
- [Google Scholar]
- University of UCLA, Dissertation Presented for Degree of Masters of Science in Dentistry [Comparison of Skeletal and Dental Changes with MSE (Maxillary Skeletal Expander) and Hyrax Appliance using CBCT Imaging] UCLA Electronic Theses and Dissertations.
- [Google Scholar]
- Cone-beam computerized tomography evaluation of the maxillary dentoskeletal complex after rapid palatal expansion. Am J Orthod Dentofacial Orthop. 2010;138:486-92.
- [Google Scholar]
- Three-Dimensional Evaluation of Implant-Supported Rapid Maxillary Expansion vs. Traditional Tooth-Borne Rapid Maxillary Expansion using Cone-Beam Computed Tomography thesis
- Skeletal and dentoalveolar changes after miniscrew-assisted rapid palatal expansion in young adults: A cone-beam computed tomography study. Korean J Orthod. 2017;47:77-86.
- [CrossRef] [PubMed] [Google Scholar]






