Translate this page into:
The Comparison of Patient Satisfaction after “Surgery First” and Conventional Orthognathic Surgery: An Original Research
Address for correspondence: Dr. Pritam Mohanty, Department of Orthodontics, Kalinga Institute of Dental Sciences, KIIT University, Bhubaneswar - 751 024, Odisha, India. E-mail: drpritammohanty@gmail.com
This article was originally published by Wolters Kluwer and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Aims and Objectives
We evaluated the factors which affect patient satisfaction and their expectations toward “surgery first” and conventional orthognathic surgery.
Materials and Methods
Questionnaires consisting of 17 questions were given to the subjects postoperatively who had undergone Le fort 1 maxillary superior impaction for skeletal gummy smile correction with conventional orthognathic surgery and “surgery first” approach. Eleven-point rating scale based on a (visual analog scale; 0 = poor; 10 = excellent) were used to answer six questions. Ten closed-form questions were also included as well as one open question for “further remarks.”
Results
Nineteen patients (12 females, 07 males; mean age, 23.4 ± 4.9 [standard deviation] years) gave their consent to participate in the study. The intention to undergo surgery only for esthetics was noted in 42.11% of patients; only improvement of chewing function in 21.05% and both in 36.84%.
Conclusion
The most common factor for patient satisfaction after “surgery first” and conventional orthognathic surgery was facial esthetics, but masticatory function and even psychological aspects should be considered equally when planning surgery. The patient satisfaction was more in “surgery first” than conventional orthognathic surgery. The timing of treatment and immediate results are important factors toward patient satisfaction.
Keywords
Esthetics
conventional orthognathic surgery
Le fort 1 osteotomy
patient satisfaction
“Surgery first”
Introduction
The conventional approach to orthognathic surgery involves a variable length of preoperative orthodontics, orthognathic surgery, and a relatively stable period of postoperative orthodontics.[1] The importance of presurgical orthodontics rests on the positioning of the skeletal component during surgery which may be limited by inappropriate dental alignment. However, orthodontic preparation lasts 15–24 months, which involves progressive deterioration of facial esthetics and dental function and thereby causes significant patient discomfort.[2,3]
An alternative methodology is the “surgery-first” approach (SFA). It was first proposed by Nagasaka et al. in 2009, this method proceeds with orthognathic surgery directly without presurgical orthodontics and is followed by regular postsurgical dental corrections.[4,5] The concept implies that the most of the orthodontic treatment is performed postoperatively and compared with the conventional approach. Thereby leading to a significant decrease in the overall total treatment time. This fact has a very positive influence on patients’ satisfaction with treatment.[6,7] The high orthodontic efficiency observed in SFA cases is due to the combination of two factors. First, the correction of the skeletal base, the complexity of orthodontic treatment is decreased, and soft tissue imbalances that might interfere with certain orthodontic tooth movements are eliminated from the beginning. Second, tooth movement is accelerated owing to the greater postoperative metabolic turnover. The optimal esthetic results, the significant reduction in overall treatment duration, and patient satisfaction led to a reasonable, cost-effective method to manage skeletal discrepancies in selected cases and that it has the potential to become a standard approach to orthognathic surgery in the future.[8,9]
Dentofacial deformities have a negative impact on many aspects of life. These include social interactions, professional career, love life, and personality.[10] Patients with skeletal problems may have a lower quality of life. The perception and expectations of a patient are dependent on several factors. These may be not only esthetics and function but also psychological factors.[11-13]
Hence, evaluation of different subjective and objective factors regarding patient satisfaction after conventional orthognathic surgery and SFA is needed. The comparison of patient’s satisfaction after SFA and conventional orthognathic surgery is also needed to be assessed. Keeping these things in mind, a questionnaire was constructed to assess patient’s satisfaction toward facial appearance after SFA and conventional orthognathic surgery.
Materials and Methods
Nineteen patients (12 females, 7 males) agreed to participate in the study. Informed consent was obtained from all the participants, and the confidentiality of the subjects was guaranteed. The questionnaires were made by a group of orthodontists and their patients who discussed on the experience and expectations of a patient undergoing orthognathic surgery. The questionnaires were regarding different subjective and objective factors were given to the subjects postoperatively who had undergone Le Fort I maxillary superior impaction for skeletal gummy smile correction with conventional surgery and SFA. Questionnaires were explained to the patients regarding their perceptions for improvement of orthognathic surgery. The Six questions were answered using an 11-point rating scale based on a (visual analog scale; 0 = poor; 10 = excellent). Ten closed-form questions were included as well as one open question for “further remarks.” [Figures 1-3].

- Questionaire

- Questionaire

- Questionaire
Patients stayed in the hospital for 5 days after surgery. Rigid fixation and an interocclusal splint were applied for 2 weeks, and patients wore light elastics for 2 weeks. Exclusion criteria were patients with mature cleft lip and palate with craniofacial syndromes and patients with orthognathic surgery without orthodontic treatment or with distractor devices. Institutional ethical approval was granted for this work by Kalinga Institute of Medical Sciences.
Statistical analysis
All the questionnaires responses were coded and then analyzed using SPSS version 20.0 (Version 20.0. Armonk, NY: IBM Corp). The significant values were taken at 95% confidence interval with a P < 0.05 value. Chi-square test was used to analyze the difference between the conventional and SFA mode of treatment.
Results
Nineteen patients gave their consent to participate in the study. Eleven had undergone conventional orthognathic surgery, and 8 had opted for SFA. The intention to undergo surgery only for esthetics was noted in 57.89% of the patients; only improvement of chewing function in 10.52% and both in 31.57% [Table 1 and Figure 4].
| Primary Intention | Type of Surgery | Total | P | |
|---|---|---|---|---|
| Conventional | SFA | |||
| Aesthetic Improvement | 6 | 5 | 11 | 0.425 |
| Mastication | 1 | 1 | 2 | |
| Both | 4 | 2 | 6 | |
| Total | 11 | 8 | 19 | |

- Primary intention of surgery
It was also noticed that all patients wanted to see immediate changes in their facial appearance and less treatment time to get the desired results.
When asked about the postoperative results; among the patients who had undergone conventional surgery, 18.18% saw esthetic improvement, 27.27% felt an improvement in their masticatory function, 18.18% felt an improvement in both, and 36.36% were unsure. [Table 2 and Figure 5].
| Type of Surgery | Aesthetic Improvement | Masticatory Improvement | Both | Don’t Know | Total | P |
|---|---|---|---|---|---|---|
| Conventional | 2 | 3 | 2 | 4 | 11 | 0.114 |
| SFA | 5 | 1 | 2 | 0 | 8 | |
| Total | 7 | 4 | 4 | 4 | 19 |
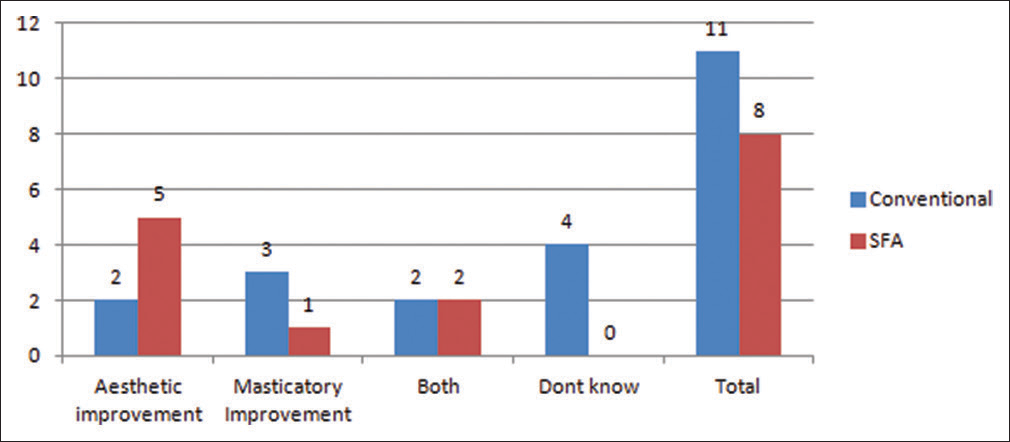
- Postoperative overall result
Among patients who had undergone for SFA; 62.5% saw esthetic improvement, 12.5% felt an improvement in their masticatory function, and 25.0% felt an improvement in both [Table 2 and Figure 5].
There was a significant difference seen in the patient’s perspective regarding pre- and post-surgical results in the case of patients who opted for SFA. The before and after results for patients undergone SFA was more appreciated [Table 3 and Figure 6].
| Score | Frequency | P | ||
|---|---|---|---|---|
| Conventional | SFA | Total | ||
| 6 | 1 | 0 | 1 | 0.00 |
| 7 | 2 | 2 | 4 | |
| 8 | 3 | 2 | 5 | |
| 9 | 3 | 3 | 6 | |
| Median score=7 | Median score=8.5 | Median score=8 | ||
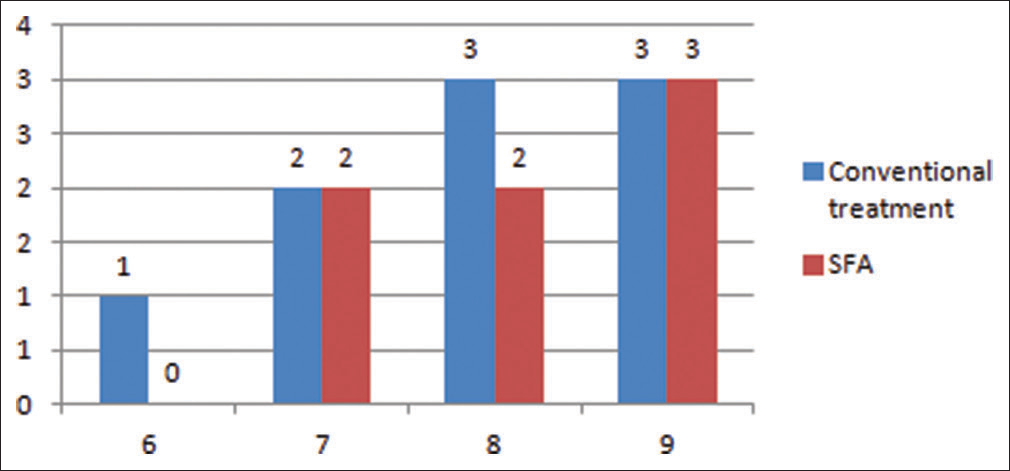
- Appearance of face after surgery (visual analog scale)
When the outcome of both the surgeries was compared on an individual level and on peer level a significant value of P was obtained, suggesting a better response in case of SFA individuals [Tables 4, 5 and Figures 7, 8].
| Satisfaction Score | Frequency | P | ||
|---|---|---|---|---|
| Conventional | SFA | Total | ||
| 6 | 3 | 0 | 3 | 0.01 |
| 7 | 6 | 1 | 7 | |
| 8 | 2 | 3 | 5 | |
| 9 | 0 | 3 | 3 | |
| 10 | 0 | 1 | 1 | |
| Median score=7 | Median score=8.5 | Median score=7 | ||
| Satisfaction Score | Frequency | P | ||
|---|---|---|---|---|
| Conventional | SFA | Total | ||
| 6 | 5 | 0 | 3 | 0.00 |
| 7 | 4 | 1 | 5 | |
| 8 | 2 | 3 | 5 | |
| 9 | 0 | 3 | 3 | |
| 10 | 0 | 1 | 1 | |
| Median score=7 | Median score=8.5 | Median score=7 | ||
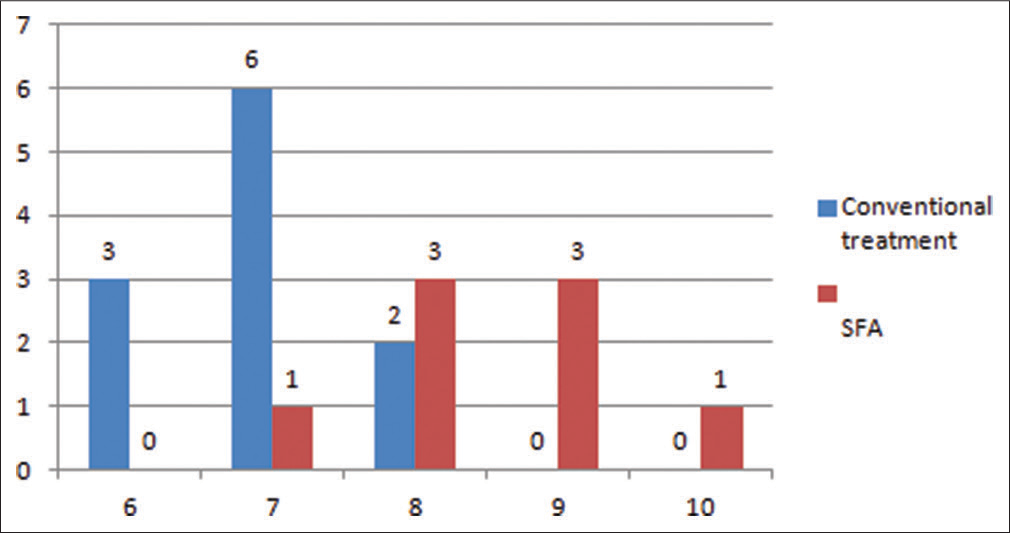
- Outcome of surgery (visual analog scale) on individual level
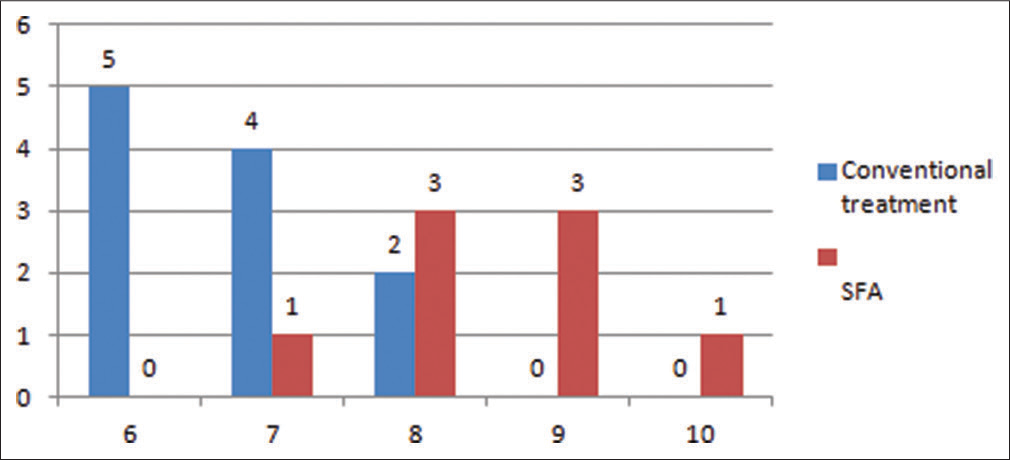
- Outcome of surgery (visual analog scale) on peer review
When the patients were asked about their comfortness after the surgery and on taking photographs. The patients who opted were more comfortable both immediately after the surgery and on taking photographs [Tables 6, 7 and Figures 9, 10].
| Satisfaction Score | Frequency | P | ||
|---|---|---|---|---|
| Conventional | SFA | Total | ||
| 5 | 2 | 0 | 2 | 0.00 |
| 6 | 3 | 0 | 3 | |
| 7 | 3 | 0 | 3 | |
| 8 | 3 | 1 | 4 | |
| 9 | 1 | 5 | 6 | |
| 10 | 0 | 2 | 2 | |
| Median score=7 | Median score=8.5 | Median score=8 | ||
| Satisfaction Score | Frequency | P | ||
|---|---|---|---|---|
| Conventional | SFA | Total | ||
| 6 | 3 | 0 | 3 | 0.00 |
| 7 | 3 | 0 | 3 | |
| 8 | 4 | 1 | 5 | |
| 9 | 1 | 1 | 2 | |
| 10 | 0 | 6 | 6 | |
| Median score=7 | Median score=10 | Median score=8 | ||
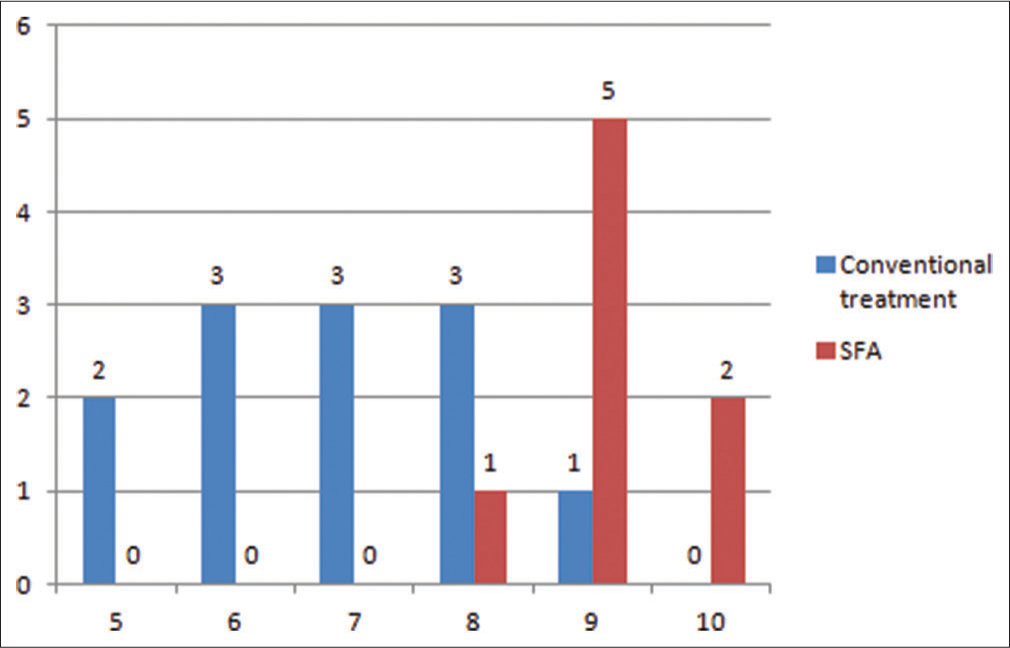
- Comfortness postsurgery
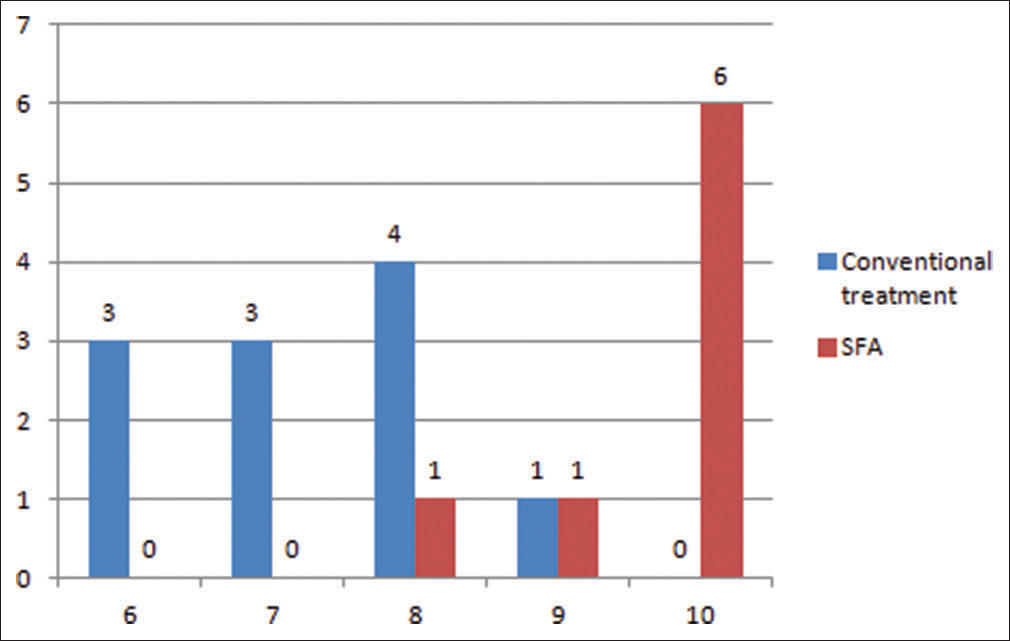
- Confidence after surgery on taking photographs
When the patients were assessed on the satisfaction of the overall treatment effects, time and procedures, 81.81% of patients who had undergone conventional surgery were satisfied, and 63.63% recommended it. While 100% of the patients who had undergone SFA were satisfied and recommended it [Tables 8, 9 and Figures 11, 12].
| Type of Surgery | P | |||
|---|---|---|---|---|
| Conventional | SFA | Total | ||
| Yes | 9 | 8 | 17 | 0.485 |
| No | 2 | 0 | 2 | |
| 11 | 8 | 19 | ||
| Type of Surgery | P | |||
|---|---|---|---|---|
| Conventional | SFA | Total | ||
| Yes | 7 | 8 | 15 | 0.103 |
| No | 4 | 0 | 4 | |
| 11 | 8 | 19 | ||
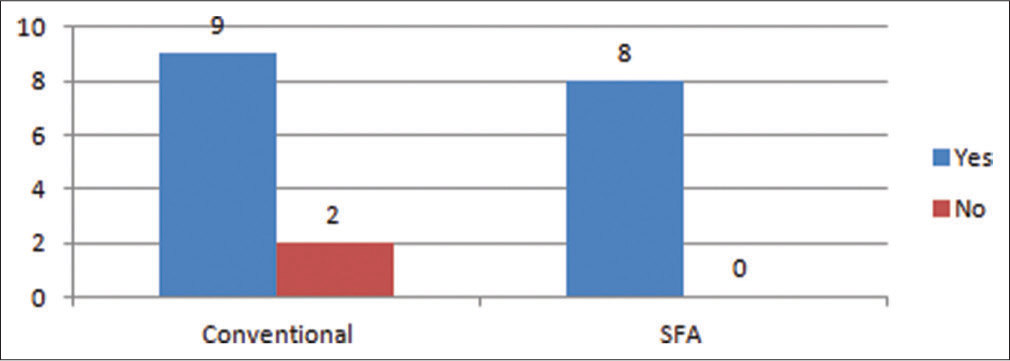
- Patient’s satisfaction with the effects

- Recommendation of the treatment after surgery
Most of the patients in further remarks wrote about their confidence boost and increased self-esteem after the surgery. However, there were also a few who wrote about the disheartening experience during the decompensation period of the conventional treatment. One patient who had undergone SFA wrote: “Right after the surgery, I met my new self.” It is the immediate effect of SFA that impresses the patient and help them to cooperate more.
Discussion
The definition of real success in our field first was initiated from the recognition of the problem and strong will power to overcome such problems by finding solutions. In this perspective, the SFA was successful in terms of focusing on the patients’ chief problem.[14] “Accountability” which is defined as the orthodontist’s ability to explain clearly the specific reason and course of treatment in a predictable way is yet another factor in our field. Orthognathic surgery has a certain amount of relapse, instability, and unpredictability.
Almost all patients are satisfied with the surgical outcomes of orthognathic surgery. This fundamental dilemma concerning “accountability” as a factor can improve our practice and can make a new major progress in our field. In the case of the conventional orthognathic treatment procedure, SFA needs to show scientific evidence as to whether this procedure can have a definitive advantage in terms of accountability.[15-17] SFA is thus believed to be a paradigm shift in the world of orthognathic surgery.
Dental occlusion and facial esthetics can show immediate effects postsurgery when using an SFA.[17,18] The SFA offers an alternative to the orthodontics-first approach for correction of Dentofacial deformities. The advent of postoperatively accelerated orthodontic tooth movement also reduces the difficulties and complications associated with and the time spent on postoperative orthodontics. Both the orthodontist and the maxillofacial surgeon using an SFA should be well-experienced and should cooperate closely with each other to achieve predictable and satisfactory outcomes.[19-21] Orthodontists should be aware of the orthognathic principles, limitations in orthodontic movement and plan postoperative orthodontic treatment to include alignment, incisor decompensation, arch coordination, and occlusal interdigitation. The maxillofacial surgeon should be experienced enough of performing designated osteotomy and intermaxillary fixation with occlusion bite plate on malaligned dental arches and providing the stability after skeletal reposition.
The reduction of the overall orthodontic treatment period and immediate facial changes would be the most significant advantages of this approach. Dentofacial deformity affects patient quality of life in our society.[22,23] The high satisfaction rate according to the questionnaire given to the patients was ranged between 70% and 87%. There was a marked improvement in self-confidence in 67.5% of patients as a result of an improved appearance and chewing function. Patients responded that immediate surgical treatment had a great impact on their friends and family.[24,25] Satisfaction of those correlated significantly with patients’ satisfaction.[26] From the questions asked we get to know that patients’ mental attitude about his/her postoperative appearance may be influenced by the support from family postsurgery. In contrast, the prevalence of postoperative complications such as numbness, prickle-sensations, pain in the temporomandibular joint area, or restrictions in mouth-opening had no overall effect on satisfaction.[27]
The primary factor of satisfaction with surgery first was whether or not the result was perceived to be an esthetic improvement. If there was an esthetic improvement in facial features immediately, the satisfaction was high in comparison to the conventional orthognathic surgery, regardless of functional problems.[28,29] An important result of this study was that a correlation between age, sex, and response to the questionnaire was not found. Young male patients wanted functional improvement, and older male patients showed no alteration in self-esteem or depression with surgery first technique. Young females desired for improvement in self-confidence and older female patients displayed improved self-esteem and diminished depressive symptoms due to surgical intervention.
It is well-known that satisfaction and the perception of surgical outcome depend on two important factors, preoperative expectations and the degree to which the procedure is explained by the orthodontist or the maxillofacial surgeon. Patients who are psychologically depressed before surgery tend to report a higher recovery burden and experience more difficulty with symptoms with social/self-concerns in the initial months of the postsurgery. Various factors may change postoperative satisfaction of the patients like written data about the sequelae and the recovery period.[30]
During conservations, the previously operated patients talked about their experiences, which helped on the emotional preparation of the patients about to undergo orthognathic surgery. This activity did not create negative impressions in the patients because it did not cause distress or anxiety. Visualizing treatment simulation before surgery did not affect the perception of symptoms or satisfaction postsurgery. After surgery first approach, most patients report an improvement in self-confidence, body and facial image, and social adjustment, but some patients are only temporarily satisfied and become litigious or violent.[31,32] Patients who receive an inadequate explanation of the surgery are prone to be emotionally unprepared and anxious after surgery, but orthognathic surgery may not be beneficial for patients who assume that it will solve most of their problems.
A similar study was conducted by Huang et al.,[33] in which there was a comparison of oral health-related quality of life and satisfaction in SFA and conventional orthognathic surgery patients. The quality of life in orthodontic-first group was deteriorated before orthognathic surgery whereas, in surgery-first group, the quality of life was immediately improved which lead to better satisfaction.
The limitations of the study include convenience sampling and a nonvalidated questionnaire thus, making the findings of this study exclusive to a particular sector of population. The result may not have a quantitative accurateness, but qualitatively, it will remain the same as this study is basically the comparison of the SFA and Conventional orthognathic surgery on patient perceptiveness.
Conclusion
The most distinctive factors for patient satisfaction after orthognathic surgery and conventional orthognathic surgery were facial esthetics. The patient satisfaction was more in orthognathic surgery than conventional orthognathic surgery. The timing of treatment and immediate results are important factors toward patient satisfaction. Function, esthetics and even psychological aspects should be considered equally when planning surgery.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Face value: An exploration of the psychological impact of orthognathic surgery. Br J Oral Maxillofac Surg. 2011;49:376-80.
- [Google Scholar]
- Oral health-related quality of life in orthognathic surgery patients. Am J Orthod Dentofacial Orthop. 2010;137:790-5.
- [Google Scholar]
- Patients’ perceptions of orthognathic treatment, well-being, and psychological or psychiatric status: A systematic review. Acta Odontol Scand. 2010;68:249-60.
- [CrossRef] [Google Scholar]
- “Surgery first” skeletal class III correction using the Skeletal Anchorage System. J Clin Orthod. 2009;43:97-105.
- [CrossRef] [Google Scholar]
- Surgery-first approach on patients with temporomandibular joint disease by intraoral vertical ramus osteotomy. Oral Surg Oral Med Oral Pathol Oral Radiol. 2013;116:e429-36.
- [Google Scholar]
- Impact of orthognathic surgery on quality of life. J Oral Maxillofac Surg. 2008;66:1194-9.
- [CrossRef] [PubMed] [Google Scholar]
- Evaluation of life quality of patients submitted to orthognathic surgery. Dental Press J Orthod. 2013;18:107-14.
- [Google Scholar]
- Quality of life in patients with severe malocclusion before treatment. Eur J Orthod. 2010;32:43-8.
- [Google Scholar]
- Patient motivation and response to surgical correction of prognathism. Oral Surg Oral Med Oral Pathol. 1976;41:309-13.
- [CrossRef] [Google Scholar]
- Change in quality of life after combined orthodontic-surgical treatment of dentofacial deformities. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010;109:46-51.
- [Google Scholar]
- Psychosocial considerations in surgery and orthodontics In: Proffit WR, White RP, eds. Surgical-Orthodontic Treatment. St. Louis: Mosby; 1991. p. :421-37.
- [Google Scholar]
- Orthodontic preparation for orthognathic surgery: How long does it take and why? A retrospective study. Br J Oral Maxillofac Surg. 2003;41:401-6.
- [Google Scholar]
- Changes in quality of life after orthognathic surgery: A comparison based on the involvement of the occlusion. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112:719-25.
- [Google Scholar]
- Orthodontic objectives in orthognathic surgery: State of the art today. World J Orthod. 2006;7:177-91.
- [Google Scholar]
- “Surgery first” in bimaxillary orthognathic surgery. J Oral Maxillofac Surg. 2011;69:e201-7.
- [CrossRef] [PubMed] [Google Scholar]
- Oral surgeons’ considerations in surgical orthodontic treatment. Dent Clin North Am. 1988;32:481-507.
- [Google Scholar]
- The duration and sequencing of surgical-orthodontic treatment. Int J Adult Orthodon Orthognath Surg. 1995;10:35-42.
- [CrossRef] [Google Scholar]
- Who needs surgical-orthodontic treatment? Int J Adult Orthodon Orthognath Surg. 1990;5:81-9.
- [Google Scholar]
- Psychometric properties of the Brazilian version of the Orthognathic Quality of Life Questionnaire. J Oral Maxillofac Surg. 2013;71:1762.e1-8.
- [CrossRef] [PubMed] [Google Scholar]
- The impact of malocclusion/ orthodontic treatment need on the quality of life. A systematic review. Angle Orthod. 2009;79:585-91.
- [CrossRef] [PubMed] [Google Scholar]
- The relationship between oral conditions, masticatory performance and oral health-related quality of life in children. Arch Oral Biol. 2013;58:1070-7.
- [CrossRef] [PubMed] [Google Scholar]
- The clinical relevance of orthognathic surgery on quality of life. Int J Oral Maxillofac Surg. 2011;40:926-30.
- [Google Scholar]
- Patients’ preoperative expectations and postoperative satisfaction of dysgnathic patients operated on with resorbable osteosyntheses. J Craniofac Surg. 2011;22:730-4.
- [Google Scholar]
- Changes in quality of life and their relation to cephalometric changes in orthognathic surgery patients. Angle Orthod. 2012;82:235-41.
- [CrossRef] [PubMed] [Google Scholar]
- Changes in quality of life and impact on patients’ perception of esthetics after orthognathic surgery. J Pharm Bioallied Sci. 2012;4(2):S290-3.
- [Google Scholar]
- Effect of orthodontic treatment on oral health-related quality of life. Angle Orthod. 2013;83:892-8.
- [CrossRef] [PubMed] [Google Scholar]
- Quality of Life in orthognathic surgery patients: Post-surgical improvements in aesthetics and self-confidence. J Craniomaxillofac Surg. 2012;40:400-4.
- [CrossRef] [PubMed] [Google Scholar]
- Quality of life assessment in patients with dentofacial deformity undergoing orthognathic surgery – A systematic review. Int J Oral Maxillofac Surg. 2013;42:974-80.
- [Google Scholar]
- Psychosocial factors associated with orthodontic and orthognatic surgical treatment. Semin Orthod. 2000;6:259-69.
- [Google Scholar]
- Health-related quality of life following orthognathic surgery. Int J Adult Orthodon Orthognath Surg. 1998;13:67-77.
- [CrossRef] [Google Scholar]
- Psychologic changes in orthognathic surgery patients: A 24-month follow up. J Oral Maxillofac Surg. 1984;42:506-12.
- [Google Scholar]
- Health-related quality of life and psychosocial function 5 years after orthognathic surgery. Am J Orthod Dentofacial Orthop. 2003;124:138-43.
- [Google Scholar]
- The changes of oral health-related quality of life and satisfaction after surgery-first orthognathic approach: A longitudinal prospective study. Head Face Med. 2016;12:2.
- [Google Scholar]






