Translate this page into:
Comparison of rate of maxillary canine movement with or without modified corticotomy facilitated orthodontic treatment: A prospective clinical trial
Address for Correspondence: Dr. Harshal Suryavanshi, Dr. G. D. Pol Foundation’s YMT Dental College and Hospital Campus, Sector 4, Kharghar, Navi Mumbai - 410 210, Maharashtra, India. E-mail: dentistharshal@gmail.com
This article was originally published by Wolters Kluwer and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Background and Objectives
The average orthodontic treatment time for extraction therapy is 31 months. One of the main disadvantages of orthodontic treatment is time. Alveolar corticotomies have been used in conjunction with orthodontics to reduce the treatment time by increasing the rate of tooth movement. Concerns about the possible risks of corticotomy procedure have led to the modification of this technique. Germeç et al. reported a case treated by their modified corticotomy technique and noted reduced treatment time without any adverse effects on the periodontium and the vitality of teeth with their new conservative corticotomy technique. This study was undertaken to clinically evaluate the efficacy of the aforesaid technique.
Materials and Methods
A split-mouth study design was carried out to compare the rate of maxillary canine movement with and without modified corticotomy facilitated orthodontic treatment in 10 patients requiring maxillary first premolar extractions. The modified corticotomy procedure was performed on the maxillary arch unilaterally. The upper arch was immediately activated bilaterally after surgical procedure using equal orthodontic forces for retraction of the maxillary canines. The amount of tooth movement was recorded at an interval of every month till the completion of canine retraction. The rate of canine movement on experimental and control site was compared. The patients were followed for 6 months to check the occurrence of undesired effects such as root resorption, periodontal damage and loss of vitality of teeth on the experimental side.
Results
Higher mean velocity was observed in canines with modified corticotomy facilitated retraction compared to conventionally retracted canines; with the difference in mean velocity between the two groups was found to be clinically significant as well as statistically significant (P < 0.001).
Interpretation and Conclusion
The results suggested that modified corticotomy technique serves as an effective and safe way to accelerate orthodontic tooth movement, without adversely affecting the periodontium, root resorption, and the vitality of the teeth, as concluded by clinical and radiographic examination.
Keywords
Canine retraction
modified corticotomy
rapid tooth movement
treatment time
INTRODUCTION
Many surgical procedures have been combined with conventional orthodontics for improved and speedy treatment. Surgical alveolar corticotomy have been used for years as an adjuvant in orthodontic treatment. The purpose of using corticotomy is proposed to be shortened retraction time. In literature, the term corticotomy is vaguely defined and is often confused with osteotomy. The corticotomy procedure is a surgical technique in which a fissure or bur hole is made through both the buccal and/or lingual cortical plates that surround the tooth, so that the tooth sits in a block of bone connected to other teeth and structures only through the medullary bone. In contrast, osteotomy is defined as cuts though the entire thickness of both buccal and lingual cortical plates and the interposed medullary bone, potentially creating a mobilized segment of bone.
The original corticotomy technique described by Kole in 1959 was a combination of inter-radicular corticotomies and supra-apical osteotomies.[1] Since the pioneering work of Kole, many clinicians have performed the procedure and reported similar outcomes.[2-4] Corticotomies have been applied to a variety of treatment modalities, such as retraction of the anterior teeth for bimaxillary dentoalveolar protrusion in combination with skeletal anchorage,[5,6] intrusion of overerrupted molars with magnets[6] or miniplates,[7] molar distalization to correct class II malocclusion,[7,8] closing of anterior open bite[3,4,9,10] and correction of cross bites,[11,12] exposure of palatally impacted canines,[13] maxillary or mandibular posterior displacement of anterior alveolar segment.[14,15]
Much of the literature on corticotomy is largely based on empirical evidence and case reports. Long-term controlled clinical trials are needed to evaluate efficacy, the advantages and disadvantages of this technique. This study was undertaken to compare the rate of maxillary canine movement with and without modified corticotomy facilitated orthodontic treatment. Modified corticotomy facilitated orthodontic treatment; proposed by Germeç et al.[2] in 2006, is a relatively new treatment in the orthodontic realm. It promises to radically shorten the time of orthodontic treatment with an oral surgical procedure.
To date, there have been no extensive studies evaluating this efficacy of this technique. Hence, this study has been taken up to comparing the rate of maxillary canine movement with and without modified corticotomy facilitated orthodontic treatment.
MATERIALS AND METHODS
A split mouth design was followed. A sample size of 10 patients and 20 sites were selected. A random sampling method was followed for sampling. The patients having large overjet, requiring maxillary first premolar extractions, undergoing fixed orthodontic treatment with preadjusted edgewise appliance were selected. All patients were within age group of 18-35 years. Patients having alveolar bone loss, periodontal disease and with diseases like rheumatoid arthritis that require regular doses of nonsteroidal anti-inflammatory drugs, which interfere with the rate of orthodontic tooth movement[16] were excluded.
All the patients were started with the routine orthodontic treatment procedure using preadjusted edgewise appliance. Before orthodontic leveling and alignment, upper first premolar extractions were carried out under local anesthesia. Patients were explained regarding the study, about surgical procedure and an informed consent was obtained. Pretreatment orthopantomogram and intra oral peri-apical radiograph in relation to the maxillary canine and maxillary second premolar teeth from experimental was obtained [Figure 1]. The extraction space having more distance to be traveled by maxillary canine was selected as an experimental site so as to gain the benefit of proposed advantage of the technique. All the procedures were carried out by the same operator using standard surgical technique.

- Preoperative intra oral peri-apical radiograph
The vertical guideline bur holes were performed on the buccal cortex, distal to canine and mesial to second premolar, with a 0.5 mm diameter surgical bur. These bur holes extended through the cortical bone, just minimally penetrating into the spongiosa. A chisel was then used to connect these bur holes and to reach the lingual cortical bone from labial side [Figure 2].
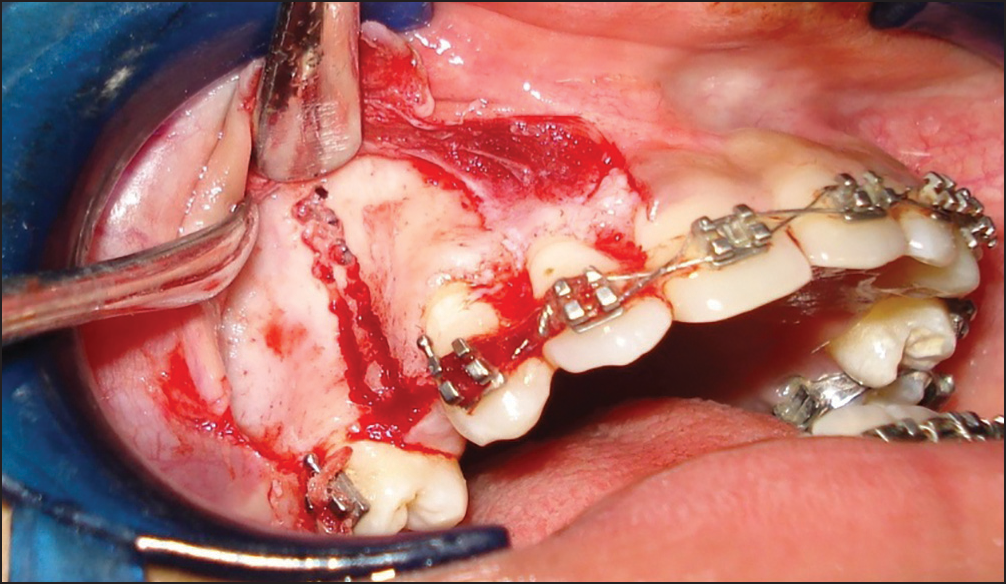
- Defined segment of cortical bone distal to canine
In this modified corticotomy technique, lingual supra-apical horizontal and lingual vertical cuts were not be performed. After bleeding control, the flap was repositioned and closed primarily.
The upper arch was immediately activated after surgical procedure because the time span between surgery and tooth movement is critical.[2] Equal orthodontic forces were applied bilaterally with the help of Dontrix gauge. The amount of the tooth movement was recorded at an interval of every month till the completion of the canine retraction. The rate of canine movement on experimental and control site was compared. The patients were followed for 6 months to check the occurrence of undesired effects such as root resorption, periodontal damage and loss of vitality of teeth on the experimental side [Figure 3].

- Six months postretraction intra oral peri-apical radiograph
RESULTS
This study was conducted to compare the rate of maxillary canine movement with and without modified corticotomy. The baseline readings in millimeters up to the first decimal were recorded on both the extraction spaces of bilateral first premolars. The space having more distance to be traveled by the canine for the completion of retraction was selected as the experimental site whereas the other site was selected as a control site. The space present on both the sites was recorded for both the groups at baseline as well as at an interval of 1 month.
The velocity or the rate of tooth movement (mm/month) was calculated in the samples of both the modified corticotomy as well as conventional groups and was recorded [Table 1].
| Subject number | Modified corticotomy | Conventional |
|---|---|---|
| Subject 1 | 1.20 | 0.93 |
| Subject 2 | 1.00 | 0.85 |
| Subject 3 | 1.00 | 0.78 |
| Subject 4 | 0.99 | 0.74 |
| Subject 5 | 1.00 | 0.77 |
| Subject 6 | 0.98 | 0.76 |
| Subject 7 | 0.99 | 0.76 |
| Subject 8 | 1.20 | 0.92 |
| Subject 9 | 1.00 | 0.75 |
| Subject 10 | 0.86 | 0.80 |
This data were subjected to statistical analysis to compare the velocity or the rate of tooth movement (mm/ month) between the two groups; and the paired t-test was applied [Graph 1].
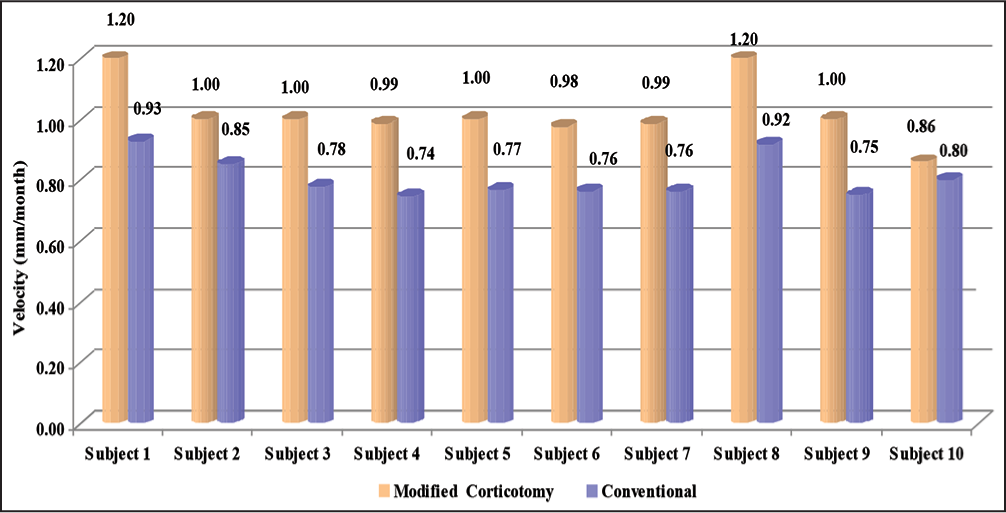
- Velocity (mm/month) in the two groups for each subject
Higher mean velocity (mm/month) is recorded in modified corticotomy group compared to the conventional group. The difference in mean velocity between the two groups is found to be statistically significant (P < 0.001) [Table 2].
| Group | n | Mean | SD | Mean difference | t | P |
|---|---|---|---|---|---|---|
| Modifi ed corticotomy | 10 | 1.02 | 0.10 | 0.216 | 5.488 | <0.001* |
| Conventional | 10 | 0.81 | 0.07 |
*Statistically signifi cant diff erence; SD – Standard deviation
DISCUSSION
The average orthodontic treatment time for extraction therapy is 31 months.[2,17,18] One of the main disadvantages of orthodontic treatment is time. Unfortunately, many potential orthodontic patients jeopardize their dental health and decline treatment, due to this long treatment times and the multitude of appointments that are required. Also, lengthy orthodontic treatment time has been linked to an increased risk of root resorption, gingival inflammation, decalcification, and dental caries.[19,20] Therefore, reducing the treatment time is an appropriate goal, which requires increasing the rate of tooth movement. To shorten the time for orthodontic tooth movement, various attempts have been made. These attempts fall into three categories. The first is local or systemic administration of medicines.[21-25] The second category is mechanical or physical stimulation such as direct electrical current[26] or a samarium-cobalt magnet.[27] The last category is oral surgery, including dental distraction,[28] alveolar surgeries to undermine interseptal bone[29] and alveolar corticotomies, which have been used in conjunction with orthodontics to correct malocclusions for over many years.
Concerns about the possible risks of corticotomy procedure have led to the modification of this technique. The original technique described by Kole included a combined interradicular corticotomy and supra-apical osteotomy. Although the results of the Kole osteotomies were stable, pulp mortifications were not rare.[2] Later, the supra-apical osteotomy was replaced by corticotomy, and labial and lingual corticotomy cuts were used to circumscribe the roots of the teeth.[3,30] Generally, the conventional corticotomy techniques include both labial and lingual cuts[3,4,30] and sometimes require two-stage surgery.[3,31] Some animal experiments and case reports regarding the effects of segmental alveolar movement after corticotomy revealed no damages in the pulp and no adverse effects on the periodontium of the teeth.[4,16,30] It was also reported that reactive inflammation of pulp and vacuolar degeneration in maxillary anterior teeth were observed after protraction with two-stage corticotomy in the maxilla.[32] Ozturg et al.[33] reported that ischemia of the pulp can occur following corticotomy at the Le Fort I level and concluded that corticotomy 5 mm above the dental apices did not have any serious effect on pulpal blood flow. However, in modified mandibular corticotomy technique, which was used in this study, the lingual vertical and supra-apical horizontal cuts were not performed and lingual flap was not elevated, so as to support the blood supply of the dentoalveolar region by lingual mucosa, whereas the access to the lingual cortical bone was achieved from the labial side. In this study, pulp vitality of the maxillary canine and maxillary second premolar on the corticotomy side was checked in all subjects, 6 months after the completion of canine retraction using electronic pulp vitality tester. No loss of vitality was noted with any of the teeth.
In the developmental process of corticotomy procedure, the marginal bone was excluded from the operation side in an attempt to protect the crestal bone and periodontal membrane, which may be highly vulnerable after subapical osteotomies accompanied by vertical corticotomies.[16] In accordance with these instructions, the vertical cuts were advised to begin 2-3 mm below the alveolar crest in a technique proposed by Suya.[34] However, in this study, because the crestal bone and the periodontal membrane were supported by the intact lingual mucosa, the vertical cuts were extended to the gingival margin on the buccal side with no adverse effects at the end of treatment. Subjects were followed 6 months after the completion of canine retraction. Intraoral examination was carried out to check for the occurrence of any obvious periodontal damage. Orthopantomogram as well as intraoral periapical radiographs of the dentoalveolar segment on the experimental side was obtained. There was no clinical evidence of gingival recession, tooth mobility or radiographic evidence of root resorption or any periodontal damage.
The conventional corticotomy techniques sometimes require two-stage surgery.[3,31] Although the clinical healing was uneventful in these conventional techniques, some complications such as subcutaneous hematomas of the face and the neck could occur after intensive corticotomies.[30] In the present study, no such complication was observed. The advantages of this technique over conventional techniques are:
It is a conservative surgery, with the elimination of lingual flap elevation and subsequent lingual vertical and subapical horizontal cuts
It is a one stage surgery
Reduction of the operation time and
Reduced postoperative patient discomfort
Corticotomy has been proposed as an alternative to conventional orthodontic treatment in difficult adult cases for rapid tooth movement. Chung et al. reported that the complete retraction of anterior teeth combined with corticotomy in a case with severe bimaxillary protrusion took <3½ months.[3] According to clinical observations of Duker, the required position of teeth after corticotomy could be achieved even earlier than 1½-3 months.[16] Gantes et al. observed approximately 50% reduction in orthodontic treatment time in corticotomy-facilitated orthodontics.[30] Fischer noted a reduction of orthodontic treatment time of 28-33% with corticotomy-assisted exposure of palatally impacted canines.[13]
In this study, when the rates of canine movement were evaluated, extrapolation of the velocities revealed that the modified corticotomy assisted canines, moved at a rate of 1.02 mm/month versus 0.81 mm/month for the conventionally retracted canines. The difference in mean velocity between the two groups was found to be clinically significant as well as statistically significant (P < 0.001) and was in accordance with the previous reports.
The earlier concept of the rapid tooth movement was based on bony block movement in corticotomy techniques including buccal and lingual vertical and subapical horizontal cuts circumscribing the roots of the teeth. The tooth embedded within a block of medullary bone served as a handle by which the bands of less-dense medullary bone surrounding the teeth were moved block by block. On the other hand, the latest concept on the rapid tooth movement after corticotomy is supported by the regional acceleratory phenomenon (RAP), described as accelerated bone turnover and decreased regional bone density.[31,35-38] The RAP mechanism potentiating tissue healing was shown to occur in the mandible as well as in long bones.[38] Wilcko et al. presented cases treated in approximately 6 months with combined corticotomy-facilitated orthodontics and periodontal alveolar augmentation called accelerated osteogenic orthodontics.[39] In most of their nonextraction cases, both labial and lingual vertical and subapical corticotomies and selective decortication were performed, and a bone augmentation procedure was added to protect the periodontium during expansive tooth movements.[31,39] In an attempt to clarify the mode of tooth movement after corticotomy, pre- and post-treatment computed tomography (CT) scans were compared, and the findings indicated a demineralization-remineralization phenomenon rather than a bony block movement. Because the CT scans or histolologic findings were not available in the present study, it was not likely to definitely state the nature of tooth movement. However, the rapid tooth movement seemed to mostly depend on RAP rather than bony block movement because the lingual cortical bone was left intact, and bone blocks surrounding teeth were not formed. Furthermore, labial vertical cuts, which were deepened into the spongiosa reaching lingual cortical bone, might help RAP diffuse in the lingual cortical bone. The wounding of the lingual cortical bone to stimulate RAP was performed from the labial side in contrast to the two-sided corticotomies. It was also demonstrated that, during healing of bone defects, a systemic acceleratory phenomenon occurs in the cancellous bone compartment in addition to RAP.[40] Unfortunately, the published data on the explanation of the accelerated tooth movement concept during corticotomy-facilitated orthodontics are based on few case reports. Therefore, controlled studies with an increased number of subjects are required. Furthermore, the need for double-sided corticotomies should be investigated because the single-sided approach followed in this study was found to be sufficient to stimulate rapid tooth movement.
References
- Surgical operations on the alveolar ridge to correct occlusal abnormalities. Oral Surg Oral Med Oral Pathol. 1959;12:515-29.
- [Google Scholar]
- Lower incisor retraction with a modified corticotomy. Angle Orthod. 2006;76:882-90.
- [Google Scholar]
- Combined surgical and orthodontic management of anterior open bite using corticotomy. J Oral Surg. 1978;36:216-9.
- [Google Scholar]
- Treatment outcomes of orthodontic treatment, corticotomy-assisted orthodontic treatment, and anterior segmental osteotomy for bimaxillary dentoalveolar protrusion. Plast Reconstr Surg. 2007;120:1027-36.
- [Google Scholar]
- An adult bimaxillary protrusion treated with corticotomy-facilitated orthodontics and titanium miniplates. Angle Orthod. 2006;76:1074-82.
- [Google Scholar]
- Intrusion of overerupted molars by corticotomy and orthodontic skeletal anchorage. Angle Orthod. 2007;77:1119-25.
- [Google Scholar]
- The use of segmental corticotomy to enhance molar distalization. J Clin Orthod. 2007;41:693-9.
- [Google Scholar]
- Enhanced effect of combined treatment with corticotomy and skeletal anchorage in open bite correction. J Oral Maxillofac Surg. 2009;67:563-9.
- [Google Scholar]
- Corticotomy and compression osteogenesis in the posterior maxilla for treating severe anterior open bite. Int J Oral Maxillofac Surg. 2007;36:354-7.
- [Google Scholar]
- Unilateral cross bite treated by corticotomy-assisted expansion: Two case reports. Head Face Med. 2010;6:6.
- [Google Scholar]
- Maxillary expansion following modified maxillary corticotomy — Its efficacy and long-term stability. J Oral Maxillofac Surg. 1991;49(1):93-4.
- [Google Scholar]
- Orthodontic treatment acceleration with corticotomy-assisted exposure of palatally impacted canines. Angle Orthod. 2007;77:417-20.
- [Google Scholar]
- Biomechanical effects of orthodontic treatment by using anchorage device combined with corticotomy. J Craniomaxillofac Surg. 2006;34(1):208.
- [Google Scholar]
- Segmental corticotomy for retracting the anterior maxilla. J Craniomaxillofac Surg. 2008;36(1):103.
- [Google Scholar]
- Experimental animal research into segmental alveolar movement after corticotomy. J Maxillofac Surg. 1975;3:81-4.
- [Google Scholar]
- The duration of orthodontic treatment for patients with and without extraction. Am J Orthod Dentofacial Orthop. 1990;97:45-51.
- [Google Scholar]
- Changes in soft tissue profile after orthodontic treatment with and without extractions. Am J Orthod Dentofacial Orthop. 2002;122:67-72.
- [Google Scholar]
- Prevalence of carious white spots after orthodontic treatment with multibonded appliances. Eur J Orthod. 1986;8:229-34.
- [Google Scholar]
- Time-related root resorption after application of a controlled continuous orthodontic force. Am J Orthod Dentofacial Orthop. 1996;110:303-10.
- [Google Scholar]
- Differences in mandibular distraction osteogenesis after corticotomy and osteotomy. Int J Oral Maxillofac Surg. 2002;31:185-9.
- [Google Scholar]
- Experimental study of the effect of prostaglandin administration on tooth movement — with particular emphasis on the relationship to the method of PGE1 administration. Am J Orthod Dentofacial Orthop. 1990;98:231-41.
- [Google Scholar]
- Leukotrienes in orthodontic tooth movement. Am J Orthod Dentofacial Orthop. 1989;95:231-7.
- [Google Scholar]
- The role of cyclic AMP, calcium, and prostaglandins in the induction of osteoclastic bone resorption associated with experimental tooth movement. J Dent Res. 1983;62:877-81.
- [Google Scholar]
- The local use of vitamin D to increase the rate of orthodontic tooth movement. Am J Orthod Dentofacial Orthop. 1988;94:278-84.
- [Google Scholar]
- Electric currents, bone remodeling, and orthodontic tooth movement. II. Increase in rate of tooth movement and periodontal cyclic nucleotide levels by combined force and electric current. Am J Orthod. 1980;77:33-47.
- [Google Scholar]
- The effects of samarium-cobalt magnets and pulsed electromagnetic fields on tooth movement. Am J Orthod Dentofacial Orthop. 1995;107:578-88.
- [Google Scholar]
- Rapid canine retraction through distraction of periodontal ligament. Am J Orthod Dentofacial Orthop. 1998;114:372-82.
- [Google Scholar]
- Rapid orthodontic tooth movement aided by alveolar surgery in beagles. Am J Orthod Dentofacial Orthop. 2007;131:160.e1-10.
- [Google Scholar]
- Effects on the periodontium following corticotomy-facilitated orthodontics. Case reports. J Periodontol. 1990;61:234-8.
- [Google Scholar]
- Rapid orthodontics with alveolar reshaping: Two case reports of decrowding. Int J Periodontics Restorative Dent. 2001;21:9-19.
- [Google Scholar]
- Acceleration of orthodontic tooth movement by alveolar corticotomy in the dog. Am J Orthod Dentofacial Orthop. 2007;131:448.e1-8.
- [Google Scholar]
- Pulpal blood flow: Effects of corticotomy and midline osteotomy in surgically assisted rapid palatal expansion. J Craniomaxillofac Surg. 2003;31:97-100.
- [Google Scholar]
- Corticotomy in orthodontics In: Hosl E, Bauldhauf A, eds. Mechanical and Biological Basis in Orthodontic Therapy. Heidelberg, Germany: Huthig Buch Verlag GmbH; 1991. p. :207-26.
- [Google Scholar]
- Modeling of trabecular bone and lamina dura following selective alveolar decortication in rats. J Periodontol. 2008;79:1679-88.
- [Google Scholar]
- Comparison of corticotomy-facilitated vs standard tooth-movement techniques in dogs with miniscrews as anchor units. Am J Orthod Dentofacial Orthop. 2009;136:570-7.
- [Google Scholar]
- Corticotomy-/osteotomy-assisted tooth movement microCTs differ. J Dent Res. 2008;87:861-7.
- [Google Scholar]
- Regional accelerated phenomenon in the mandible following mucoperiosteal flap surgery. J Periodontol. 1994;65:79-83.
- [Google Scholar]
- Rapid orthodontic decrowding with alveolar augmentation: Case report. World J Orthod. 2003;4:197-205.
- [Google Scholar]
- A systemic acceleratory phenomenon (SAP) accompanies the regional acceleratory phenomenon (RAP) during healing of a bone defect in the rat. J Bone Miner Res. 1991;6:401-10.
- [Google Scholar]






