Translate this page into:
“Converting a bi-jaw surgery to a single-jaw surgery:” Posterior maxillary dentoalveolar intrusion with microimplants to avoid the need of a maxillary surgery in the surgical management of skeletal Class III vertical malocclusion
Address for Correspondence: Dr. Abhisek Ghosh, Great Lakes Multi-speciality Dental Clinic and Orthodontic Centre, 27, Janak Road (Behind Lake Mall), Kolkata - 700 029, West Bengal, India. E-mail: dr.abhisek24@gmail.com
This article was originally published by Wolters Kluwer and was migrated to Scientific Scholar after the change of Publisher.
How to cite this article: Ghosh A, Ray A. “Converting a bi-jaw surgery to a single-jaw surgery:” Posterior maxillary dentoalveolar intrusion with microimplants to avoid the need of a maxillary surgery in the surgical management of skeletal Class III vertical malocclusion. APOS Trends Orthod 2016;6:218-27.
Abstract
The management of a vertical skeletal Class III malocclusion with mandibular prognathism revolves around the protocol of bi-jaw surgery (maxillary LeFort I impaction and mandibular bilateral sagittal split osteotomy with setback). The maxillary surgery not only provides increased stability to the ultimate surgical outcome but also increases the amount by which the mandibular set back can be done, therefore aiding in greater profile improvement. With the need of maxillary surgery almost inevitable in treating such situations, the complexity and the increased discomfort associated with such surgery can never be ignored. Is it at all possible to convert a bi-jaw surgery into a single-jaw surgery with the aid of microimplants? With increasing number of patients being treated with microimplants for anterior openbite and gummy smiles, our idea was to incorporate this novel protocol in treating Class III vertical situations and therefore avoid the need of a maxillary surgery in treating such a situation, together with achieving optimum treatment outcome.
Keywords
Class III malocclusion
long face
microimplants
orthognathic surgery
vertical growth pattern
INTRODUCTION
The introduction of skeletal anchorage to orthodontic practice has made it possible to correct malocclusions which were otherwise difficult or even impossible to be corrected by regular conventional mechanics.
Among the skeletal anchorage devices which includes microimplants, mini-plates, or even dental implants, the most popular has been the microimplants, thanks to its low cost, easy surgical placement, removal and very few anatomic limitations for its placement.
Microimplants have been effective in bringing tooth movement in all three dimensions of space,[1-5] whether it is anterior tooth retraction, whole arch retraction, whole arch intrusion, single tooth intrusion, molar protraction, or even bringing about skeletal changes in maxillo-mandibular relationships while maintaining absolute anchorage.[6-9] It has therefore brought about a revelation in the field of orthodontics in the past decade.
Each success in clinical scenario brings in new hope for the clinicians to try out something new within safety limits, and same has been the case with microimplants. The effectiveness of microimplants in the correction of occlusal canting[10] or even skeletal anterior openbite[11-13] by intrusion of the posterior maxillary segment followed by counter clock-wise rotation of the mandible has brought us the hope of trying something new.
Can this same principle be used to avoid the need of a maxillary surgery (LeFort I impaction) in treating a Class III vertical skeletal malocclusion actually requiring the need of a bi-jaw surgery (LeFort I impaction, counter clock-wise mandibular rotation and mandibular set back – bilateral sagittal split osteotomy [BSSO])? – A question that can only be answered by successful, predictable, and clinical results.
If standardized treatment results are to be achieved by this method, then there shall be a paradigm change in the very thought process of treating such a situation and from the patient’s perspective, it would significantly reduce the complexity and the discomfort associated with a bi-jaw surgery.
This case report describes in details of one such situation, the treatment protocol, treatment objectives, alternatives, and the results achieved thereafter.
Introducing the T-T (modified transpalatal arch [TPA] and temporary anchorage devices [TAD] combination) technique for selective anterior and posterior maxillary dentoalveolar intrusion - The components of this system involve the use of five microimplants and modified TPA for selective intrusion of the maxillary dentoalveolar segment [Figure 1]. Of the five microimplants, four are placed in the buccal segment and one in the mid-palatal region (in adults). The buccal microimplants are placed mesial to the maxillary canine and in between the second premolar and the first molars, bilaterally. The purpose of the anterior TADs is to provide an intrusive force to the anterior maxillary dentoalveolar unit while the posterior implants help in the retraction of the anteriors and intrusion of the posterior segment.

- The T-T appliance system
It has been commonly noted that with this biomechanical system there is a chance of palatal cusp hang in the first and the second molars which ultimately hinders the true intrusion process. To counter act this, a modified TPA is placed which is soldered to the first and the second molar. An additional mid-palatal microimplant is also placed to provide an intrusive component of force from the palatal aspect and to negate the moment generated from the buccal microimplants causing the palatal cusp hang [Figure 2].

- Biomechanics of the T-T appliance system
The posterior maxillary intrusion process with subsequent slow counter clock-wise rotation of the mandible demands the elimination of the posterior most fulcrum, i.e. the third molars if they are in occlusion, banding and bonding of all dental units both in upper and lower arch and the use of light, optimum intrusive forces during the course of the treatment.
The efficiency of this system lies in the meticulous execution of its intricate biomechanics as the whole system is dependent on the quantum and duration of the force applied from each unit.
CASE REPORT
Chief complaint
An adult female patient of 26 years age reported with a chief complaint of an elongated face, prominent chin, and irregularity in upper and lower front teeth region.
Clinical examination
Extraoral examination
Extraoral examination revealed a dolichocephalic head type, a leptoprosopic facial pattern and mild facial asymmetry with the chin apparently deviated to the right side. There was increased incisal exposure on spontaneous smile [Figure 3]. The figure reflects posed smile. The profile showed an anterior divergence, with a concave facial profile, increased chin prominence, and an acute nasolabial angle.

- Pretreatment extra-oral photographs
Intraoral examination
Intraoral examination revealed angle’s Class III malocclusion with crowding of 9 mm in the maxillary arch and 7 mm in the mandibular arch with reduced overjet and anterior openbite [Figures 4 and 5]. Other dental findings include fractured maxillary left first premolar (24), dental crossbite in the region of upper right, left lateral incisors (21, 22) and upper left first permanent molar (26), blocked out mandibular canine bilaterally (33, 43), and mesioangular impaction of mandibular third molars bilaterally (38, 48). There was the presence of proclination in the upper and lower anterior dentoalveolar segment. Occlusal photographs suggest apparent asymmetry in the upper and lower dental arch.

- Pretreatment intra-oral photographs

- Pretreatment lateral cephalogram
Extra-oral radiographic findings
Lateral cephalogram showed increased mandibular body length, increased lower anterior facial height, proclination of upper and lower incisors with anterior openbite and acute nasolabial angle [Figure 5].
Orthopantomogram revealed mesioangular impaction of mandibular third molars bilaterally (38, 48) [Figure 6]. The severity of impaction was more with left third molar (38) than with the right (48). The right mandibular body segment with relationship to mandibular right second premolar showed an area of increased radio-opacity suggestive of hypercementosis (for conclusive diagnosis a histopathological examination is required, which was not done as both the tooth and the region was asymptomatic).

- Pretreatment orthopantomogram
Cephalometric analysis: Cephalometric analysis for orthognathic surgery (COGS analysis – by Dr. C. Burstone) was done expecting it to be a case of skeletal malocclusion requiring orthognathic surgery [Table 1 and Figure 7]. The significant inference drawn reveals – an increase in lower anterior facial height (76 mm, standard cephalometric norms for female of similar age group (STD) values - 61.3 standard deviations (sd) 3.3 mm), an increase in posterior maxillary height (55 mm, STD values - 50.6 sd 2.2 mm), increased mandibular divergence (30°, STD values - 24.2 sd 5°), increased maxillary anterior dental height (34 mm, STD values - 27.5 sd 1.7 mm), increased mandibular anterior dental height (45 mm, STD values - 23 sd 1.3 mm), mild increase in mandibular ramal length (50 mm, STD values - 46.8 sd 2.5 mm), significant increased mandibular body length (85 mm, STD values - 74.3 sd 5.8 mm), and proclined maxillary incisors (120°, 112 sd 5.7 mm).
| Parameters | Pretreatment | Postdecompensation | Posttreatment |
|---|---|---|---|
| Ar-Ptm (mm) | 33 | 33 | 33 |
| Ptm-N (mm) | 52 | 53 | 53 |
| N-A-Pog (°) | 1 | −3 | 0 |
| N-A (mm) | −5 | −6 | −5 |
| N-B (mm) | −9 | −6 | −13 |
| N-Pog (mm) | −7 | −4 | −11 |
| N-ANS (mm) | 56 | 55 | 55 |
| ANS-Gn (mm) | 76 | 73.5 | 72 |
| PNS-N (mm) | 55 | 55 | 55 |
| MP-HP (°) | 30 | 27 | 28 |
| Maxillary IN-NF (mm) | 34 | 32 | 32 |
| Mandibular IN-MP (mm) | 45 | 45 | 45 |
| Maxillary molar-NF (mm) | 27 | 24 | 24 |
| Mandibular molar-MP (mm) | 34 | 34 | 34 |
| PNS-ANS (mm) | 54 | 54 | 54 |
| Ar-Go (mm) | 50 | 50 | 51 |
| Go-Pog (mm) | 85 | 85 | 78 |
| B-Pog (mm) | 6 | 6 | 5 |
| Ar-Go-Gn (°) | 123 | 123 | 124 |
| OP-HP (°) | 10 | 11 | 12 |
| A-B (mm) | −4 | −9 | −2 |
| Maxillary incisors-NF (°) | 120 | 110 | 111 |
| Mandibular incisors-MP (°) | 90 | 92 | 90 |
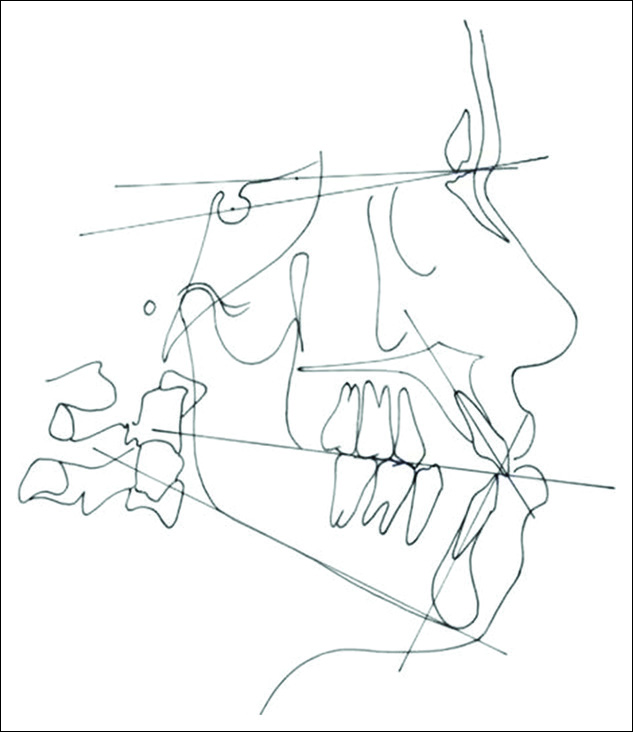
- Pretreatment cephalometric tracing
Diagnosis
The patient was diagnosed as a case of angles Class III malocclusion underlying a Class III skeletal base (increased mandibular body length) and vertical growth pattern (long face), the dental finding include presence of reduced overjet and anterior openbite with significant crowding in both upper and lower dentition, soft tissue findings include an acute nasolabial angle, concave facial profile, and a potential gummy smile.
Treatment objectives
To correct the mandibular prognathism/reduce chin prominence
To resolve crowding and proclination in upper and lower dental arch
To balance the position of the upper lips after positioning the maxillary anterior teeth properly relative to the maxilla
To change the occlusal plane in a clockwise direction by intruding the maxillary posterior teeth about 3 mm to correct the anterior openbite and increase the surgical mandibular setback movement
To establish functional occlusion with normal overbite and overjet
To achieve ideal esthetic outcome, including the correction of - nasolabial angle, concavity of profile, chin prominence, and vertical facial height.
Treatment alternatives
Camoflauge treatment
This treatment includes the extraction of lower first premolars to resolve crowding in the lower arch and nonextraction protocol in the upper arch leading to further proclination of upper incisors and worsening of the nasolabial angle, finally finishing with Class III molars and Class I canine relation (esthetic objectives and skeletal corrections will be left unattended to).
Decompensation and bi-jaw surgery
This shall include the extraction of all first premolars (14, 24, 34, 44) for the purpose of decrowding and correction of proclination followed by a bi-jaw surgery including LeFort I surgical maxillary impaction (selective – more in the posterior and less in the anterior) allowing counter-clockwise rotation of the mandible followed by mandibular set back surgery (BSSO) to achieve ideal esthetic outcome both in the sagittal and vertical dimension (Is complicated and chances of increased patient discomfort).
Decompensation, selective maxillary intrusion with microimplants (T-T technique), and single-jaw surgery (mandibular)
This covers the regular decompensation process such as a bi-jaw surgery with extraction of all 1st premolars (14, 24, 34, and 44) for the purpose of decrowding and correction of proclination followed by slow maxillary selective dentoalveolar impaction and subsequent counter clockwise rotation of the mandible replicating a surgical LeFort I maxillary impaction. This is followed by a single-jaw surgery (mandibular surgical setback-BSSO) for the correction of mandibular prognathism (reduces the complication of bi-jaw surgery provides optimum esthetic outcome).
Treatment plan and sequential progress
The choice of treatment plan was made in a joint discussion with the patient, the orthodontist, and the maxillofacial surgeon and the third treatment alternative was chosen.
After carefully analyzing the case both clinically and looking through the cephalometric parameters, the treatment progressed as follows.
Step 1: Decompensation
The patient was advised to remove the upper and lower first premolars (14, 24, 34, and 44) for the purpose of leveling and alignment and correction of upper anterior proclination. The lower third molars were also advised to be extracted as the patient would at a later date go for a mandibular set back surgery (presence of third molar during BSSO - bilateral sagittal split osteotomy, increases the chances of mandibular angle fracture).
The appliance system (0.022 × 0.028 MBT), ceramic with metal slot, was placed in all the dental units together with the modified TPA soldered on to both the first and second molars. The TPA has a helix bilaterally close to the soldered joint to provide a point of attachment for the intrusive force from the mid-palatal screw.
After the initial leveling and alignment process with sequential change of arch wires starting with the 0.014 Niti, 0.016 Niti, 0.016 Australian Special plus SS wire and ending with 0.018 Australian special plus SS wire, maxillary canine retraction was started. Lower leveling and alignment was also performed in the same way.
End mass retraction process (moderate anchorage) was started in the lower arch on 19 × 25 SS wire when the canine retraction process was in progress in the upper arch on a 0.018 SS Australian wire.
After canine retraction was completed in the upper arch and adequate space was achieved for the placement of the anterior microimplants, 19 × 25 Niti wire followed by 19 × 25 SS posted wire was placed to start the intrusion retraction process (absolute anchorage).
Microimplants were then placed in the upper anterior labial segment mesial to the canine, buccally between the second premolars and first molar and in the mid-palatal region to aid in selective intrusion and retraction process. The labial and buccal microimplants were of 1.5 × 8 mm, whereas the palatal implant was 2 × 6 mm in dimension [Figure 1].
The microimplants were immediately loaded after the placement and active intrusion and retraction forces were applied. The intrusive forces were light, optimum, and maintained within biologic limits. Increased intrusive forces applied on to teeth in adult patients increases the chances of root resorption.[14-17] The retraction forces were maintained to about 100 g per side. E-chains were used as force components, Niti coil spring were not used as they are not self-limiting and have less force decay. In case of missed appointments, this could be an issue as monitoring the intrusion process was vital in achieving differential intrusion between the anteriors and posteriors for changing occlusal plane relationship.
The intrusion retraction process continued for about 6–8 months in which selectively more intrusion was done in the posteriors to change the occlusal plane relationship. The mild upper anterior intrusion reduced the increased incisal exposure on spontaneous smile and significant posterior intrusion corrected the anterior openbite.
After about 20 months of treatment, selective maxillary intrusion was completed together with slow counter clock-wise rotation of the mandible leading to the development of a negative overjet of about 4 mm, closure of the mandibular plane, reduction in vertical facial height, and improvement in upper incisal show on spontaneous smile [Figures 8 and 9].
Cephalometric analysis - Postdecompensation: COGS comparative analysis was done to asses changes brought about by the decompensation process [Table 1 and Figures 10-12]. The significant inference drawn reveals – a decrease in lower anterior facial height - 73.5 mm (pretreatment - 76 mm), no change in posterior maxillary height - 55 mm (pretreatment - 55 mm), decrease in mandibular divergence - 27° (pretreatment - 30°), decrease in maxillary anterior dental height - 32 mm (pretreatment - 34 mm), no change in mandibular anterior dental height - 45 mm (pretreatment - 45 mm), decrease in maxillary posterior dental height - 24 mm (pretreatment - 27 mm), no change in mandibular ramal length - 50 mm (pretreatment - 50 mm), no change in mandibular body length - 85 mm (pretreatment - 85 mm), and correction of inclination of maxillary incisors - 110° (pretreatment - 120°).

- Post decompensation intra-oral photographs

- Postdecompensation extra oral photographs

- Postdecompensation lateral cephalogram

- Postdecompensation cephalometric tracing

- Superimposition of pretreatment and postdecompensation tracings
Step II: Mock surgery and surgical preparation
After adequate negative overjet was achieved as per plan and the objectives of decompensation attained, fresh impressions were taken for setting up for mock surgery.
After mounting in the articulator, the models were then checked for any occlusal interference, especially in the second molar region during the setback process. The midlines were checked for any deviation which may require an asymmetric set back, but was ruled out. The dental and the skeletal midlines matched when dental casts were compared to clinical scenario [Figure 13].
The setback amount was fixed at 7 mm thereby allowing a positive overjet of 3 mm postsurgery which gives a leeway of 1 mm for relapse, which is practically expected.
Mock surgery was performed and postsurgical final occlusion was established at Class I molar and Class I canine.
An acrylic wafer splint was made at this point of time with perforations made on the occlusal periphery to aid in the stabilization during surgical maneuvering.
Surgical preparation was then made in the patient’s mouth, passive 19 × 25 SS rectangular wire with surgical lugs soldered on to it was placed in both the upper and lower arch and consolidated with continuous ligation.

- Mock surgical set up
Step III: Mandibular set back surgery (bilateral sagittal splint osteotomy)
The mandibular set back surgery was performed following the Epker’s modification of Obwegeser’s standard protocol. The wafer splint was used to stabilize the split fragments and then fixed with rigid fixation. The patient was then put on Class III elastics for maintaining the postural mandibular position.
After 6 weeks of rest, the patient was referred back for postsurgical orthodontics.
Step IV: Postsurgical orthodontics
The postsurgical phase involved mild settling of the occlusion and correction of the maxilla-mandibular tooth material discrepancy. Therefore, the patient was put back on thinner wire (0.016 SS Australian A.J. Wilcock) and vertical settling elastic with Class III component.
Mild proximal stripping of 2 mm was done in the lower arch (Bolton discrepancy of 2 mm mandibular tooth material excess) and space closed with elastomeric chains.
The case was finally finished with Class I molar and Class I canine relationship.
Retention protocol involved bonded lingual retainers together with removal thermoplastic retainers in both upper and lower arches. The rationale for the usage of full arch thermoplastic retainers lies in the use of controlled bite forces in maintaining the vertical correction achieved in the decompensation phase[12] [Figure 14].

- Posttreatment intra-oral photographs with thermoplastic retainers
Treatment results
The final treatment results achieved after postsurgical orthodontics was extremely pleasing. The case was finished with Class I molar and canine relationship and good inter-cuspation in static occlusion. The upper and the lower dental midlines perfectly coincided. The overjet and the overbite were within standard limits. Functional occlusion was also well established posttreatment [Figure 15].

- Posttreatment intra-oral photographs
The extraoral features posttreatment was equally pleasing. The frontal face was symmetric and the competency of the lip was established. The smile was consonant and there was ideal incisal exposure at rest and on spontaneous smile. The 45° view also suggested the same. The profile was straight, the excessive chin was prominent and the acuteness of the nasolabial angle was significantly reduced therefore providing in all dimensions an overall balanced face [Figure 16].

- Posttreatment extra-oral photographs
Of the extraoral radiographs, lateral cephalogram suggested all the objectives of the treatment set were achieved thereafter. The orthopantogram showed lower third molars extracted bilaterally, rigid fixation being placed at the surgical site, good root divergence attained throughout the dentition, and no significant root resorption was noted [Figures 17 and 18].

- Posttreatment lateral cephalogram

- Posttreatment orthopantomogram
Cephalometric analysis - Posttreatment: COGS comparative analysis was done to assess changes brought about by the orthognathic surgery (mandibular set back) and decompensation when compared to pretreatment parameters [Table 1, Figures 19 and 20]. The significant inference drawn reveals – a decrease in lower anterior facial height - 72 mm (pretreatment - 76 mm), no change in posterior maxillary height - 55 mm (pretreatment - 55 mm), decrease in mandibular divergence - 28° (pretreatment - 30°), decrease in maxillary anterior dental height - 32 mm (pretreatment - 34 mm), no change in mandibular anterior dental height - 45 mm (pretreatment - 45 mm), decrease in maxillary posterior dental height - 24 mm (pretreatment - 27 mm), mild increase in mandibular ramal length - 51 mm (pretreatment - 50 mm), significant change in mandibular body length - 78 mm (pretreatment - 85 mm), and correction of inclination of maxillary incisors - 111° (pretreatment - 120°).

- Posttreatment cephalometric tracing

- Superimposition of pre- and post-treatment tracings
DISCUSSION
The correction of skeletal Class III vertical malocclusion in adults revolve around bi-jaw surgical protocol which involve LeFort I surgical maxillary impaction followed by mandibular set back surgery. Although correction of skeletal Class III malocclusion would require only a single-jaw surgery (mandibular set back/maxillary advancement), when associated with vertical problems, single-jaw surgery is not sufficient to get optimum esthetic outcome.[18-22]
Single-jaw mandibular surgery is a more predictable procedure as studies suggest no statistical difference in the position of the skeletal hard tissues between the prediction and the actual results.[23-25] However, in single-jaw surgery, the mandible tends to set back with counterclockwise rotation in patients who have a flat occlusal plane.[20] This limits the amount of backward movement of the chin. It has been reported that patients with a flat occlusal plane or increased posterior facial height had insufficient profile changes with single-jaw surgery.[21] Moreover, postsurgical stability after counterclockwise rotation of the mandible is poor because of the increase in posterior facial height and the associated increase in vertical length of the pterygo-masseteric musculature[21,22] [Figure 21].

- Diagram showing the - effect of maxillary posterior dento-alveolar Intrusion on surgical mandibular set-back
Bi-jaw surgery is normally performed in patients who need the position of the maxillary teeth or the cant of the occlusal plane changed. The bi-jaw surgery with clockwise rotation of the maxillary occlusal plane could be considered to achieve the maximum esthetic results.[12,20] Furthermore, the impaction of the posterior segment in Class III orthognathic surgery increases stability by maintaining the total posterior vertical dimension.[12,20,21] However, a surgical procedure involving the maxilla is complicated, variable,[24] and increases the discomfort level by folds. Studies suggest that vertical repositioning of the maxilla although a stable procedure has the highest likelihood of change as compared to prediction values.[26]
The T-T technique in this instance, brought about significant change in the posterior maxillary overall dentoalveolar height (change - 3 mm), anterior maxillary overall dentoalveolar height (change - 2 mm) together with closure of the mandibular plane angle (change - 3°) and thereby positioning the mandible forward for greater setback to be done during the surgical procedure [Table 1].
This exactly replicates the probable changes that would have taken place had maxillary impaction surgery been performed on the patient.
In case of severe anteroposterior deficiency or excessive vertical dimension of the maxilla, surgery of the maxilla is necessary. Impaction of the maxilla with orthognathic surgery has more potential than the intrusion of the posterior teeth with microimplants and associated orthodontic treatment. However, 2–3 mm of intrusion of the posterior teeth can be obtained easily and precisely with microimplants,[27,28] and this small movement of the posterior teeth can produce a considerable change in mandibular setback surgery. Microimplant treatments are less invasive and expensive, and cause less postoperative discomfort compared with maxillary surgical impaction.
It is to be taken into note that maxillary surgery is inevitable in certain clinical situations and cannot be avoided, but whenever there are options to negate it with the use of microimplants, this method be seriously taken as an additive treatment option considering the quality of the results achieved.
CONCLUSION
Mandibular setback surgery accompanied by intrusion of the maxillary posterior teeth with microimplants can provide good facial harmony in skeletal Class III vertical patients.
The intrusion of the maxillary posterior teeth during the retraction of the maxillary incisors with microimplants changes the occlusal plane in a clockwise direction. This increases the amount of surgical mandibular setback or distal movement of the chin, and produces similar effects on a profile as does a bi-jaw surgery that includes maxillary posterior impaction.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- The skeletal cortical anchorage using titanium microscrew implants. Korean J Orthod. 1999;29:699-706.
- [Google Scholar]
- Micro-implant anchorage for treatment of skeletal class I bialveolar protrusion. J Clin Orthod. 2001;35:417-22.
- [Google Scholar]
- Simultaneous incisor retraction and distal molar movement with microimplant anchorage. World J Orthod. 2004;5:164-71.
- [Google Scholar]
- Intrusion of posterior teeth using mini-screw implants. Am J Orthod Dentofacial Orthop. 2003;123:690-4.
- [Google Scholar]
- The use of titanium miniscrews for molar protraction in extraction treatment. Prog Orthod. 2004;5:236-47.
- [Google Scholar]
- Titanium screw anchorage for correction of canted occlusal plane in patients with facial asymmetry. Am J Orthod Dentofacial Orthop. 2007;132:237-42.
- [Google Scholar]
- Skeletal anchorage system for open-bite correction. Am J Orthod Dentofacial Orthop. 1999;115:166-74.
- [Google Scholar]
- Occlusal plane change after intrusion of maxillary posterior teeth by microimplants to avoid maxillary surgery with skeletal class III orthognathic surgery. Am J Orthod Dentofacial Orthop. 2010;138:631-40.
- [Google Scholar]
- Treatment of open bite with microscrew implant anchorage. Am J Orthod Dentofacial Orthop. 2004;126:627-36.
- [Google Scholar]
- Apical root resorption of maxillary first molars after intrusion with zygomatic skeletal anchorage. Angle Orthod. 2005;75:761-7.
- [Google Scholar]
- Intrusion of multiradicular teeth and related root resorption with mini-screw implant anchorage: A radiographic evaluation. Am J Orthod Dentofacial Orthop. 2007;132:647-55.
- [Google Scholar]
- The influences of molar intrusion on the inferior alveolar neurovascular bundle and root using the skeletal anchorage system in dogs. Angle Orthod. 2001;71:60-70.
- [Google Scholar]
- Effects of maxillary molar intrusion on the nasal floor and tooth root using the skeletal anchorage system in dogs. Angle Orthod. 2003;73:158-66.
- [Google Scholar]
- The rotation of the mandible resulting from growth: Its implications in orthodontic treatment. Angle Orthod. 1965;35:36-50.
- [Google Scholar]
- Treatment goals and planning in class III 2-jaw surgery–The contribution of jaw rotation. J Korean Found Gnatho Orthod Res. 2005;7:39-51.
- [Google Scholar]
- Results after mandibular advancement surgery: An analysis of 87 cases. J Oral Surg. 1980;38:265-82.
- [Google Scholar]
- Mandibular advancement surgery in high-angle and low-angle class II patients: Different long-term skeletal responses. Am J Orthod Dentofacial Orthop. 2001;119:368-81.
- [Google Scholar]
- A comparison of a computer-based orthognathic surgery prediction system to postsurgical results. Int J Adult Orthodon Orthognath Surg. 1997;12:55-63.
- [Google Scholar]
- Alteration of the mandibular plane during sagittal split advancement: Short-and long-term stability. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;104:160-9.
- [Google Scholar]
- The predictability of maxillary repositioning in LeFort I orthognathic surgery. Am J Orthod Dentofacial Orthop. 2002;122:142-54.
- [Google Scholar]
- An adult case of skeletal open bite with a large lower anterior facial height. Angle Orthod. 2005;75:465-71.
- [Google Scholar]
- Treatment and post treatment changes following maxillary posterior teeth with miniscrew implants for openbite correction. Korean J Orthod. 2008;38:31-40.
- [Google Scholar]






